Predictors of outcome in childhood intracerebral hemorrhage: a prospective consecutive cohort study
- PMID: 20019325
- PMCID: PMC2821039
- DOI: 10.1161/STROKEAHA.109.568071
Predictors of outcome in childhood intracerebral hemorrhage: a prospective consecutive cohort study
Abstract
Background and purpose: The purposes of this study were to describe features of children with intracerebral hemorrhage (ICH) and to determine predictors of short-term outcome in a single-center prospective cohort study.
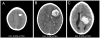
Methods: A single-center prospective consecutive cohort study was conducted of spontaneous ICH in children aged 1 to 18 years from January 2006 to June 2008. Exclusion criteria were inciting trauma; intracranial tumor; isolated epidural, subdural, intraventricular, or subarachnoid hemorrhage; hemorrhagic transformation of ischemic stroke; and cerebral sinovenous thrombosis. Hospitalization records were abstracted. Follow-up assessments included outcome scores using the Pediatric Stroke Outcome Measure and King's Outcome Scale for Childhood Head Injury. ICH volumes and total brain volumes were measured by manual tracing.
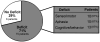
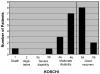
Results: Twenty-two patients, median age 10.3 years (range, 4.2 to 16.6 years), had presenting symptoms of headache in 77%, focal deficits 50%, altered mental status 50%, and seizures 41%. Vascular malformations caused hemorrhage in 91%. Surgical treatment (hematoma evacuation, lesion embolization or excision) was performed during acute hospitalization in 50%. One patient died acutely. At a median follow-up of 3.5 months (range, 0.3 to 7.5 months), 71% of survivors had neurological deficits; 55% had clinically significant disability. Outcome based on Pediatric Stroke Outcome Measure and King's Outcome Scale for Childhood Head Injury scores was worse in patients with ICH volume >2% of total brain volume (P=0.023) and altered mental status at presentation (P=0.005).
Conclusions: Spontaneous childhood ICH was due mostly to vascular malformations. Acute surgical intervention was commonly performed. Although death was rare, 71% of survivors had persisting neurological deficits. Larger ICH volume and altered mental status predicted clinically significant disability.
Conflict of interest statement
None of the authors has any conflict of interest or disclosures.
Figures
References
-
- Fullerton HJ, Wu YW, Zhao S, Johnston SC. Risk of stroke in children: Ethnic and gender disparities. Neurology. 2003;61:189–194. - PubMed
-
- Giroud M, Lemesle M, Gouyon JB, Nivelon JL, Milan C, Dumas R. Cerebrovascular disease in children under 16 years of age in the city of dijon, france: A study of incidence and clinical features from 1985 to 1993. J Clin Epidemiol. 1995;48:1343–1348. - PubMed
-
- Broderick J, Talbot GT, Prenger E, Leach A, Brott T. Stroke in children within a major metropolitan area: The surprising importance of intracerebral hemorrhage. J Child Neurol. 1993;8:250–255. - PubMed
-
- Al-Jarallah A, Al-Rifai MT, Riela AR, Roach ES. Nontraumatic brain hemorrhage in children: Etiology and presentation. J Child Neurol. 2000;15:284–289. - PubMed
-
- Blom I, De Schryver EL, Kappelle LJ, Rinkel GJ, Jennekens-Schinkel A, Peters AC. Prognosis of haemorrhagic stroke in childhood: A long-term follow-up study. Dev Med Child Neurol. 2003;45:233–239. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

