Brain volume and metabolism in fetuses with congenital heart disease: evaluation with quantitative magnetic resonance imaging and spectroscopy
- PMID: 20026783
- PMCID: PMC2819908
- DOI: 10.1161/CIRCULATIONAHA.109.865568
Brain volume and metabolism in fetuses with congenital heart disease: evaluation with quantitative magnetic resonance imaging and spectroscopy
Abstract
Background: Adverse neurodevelopmental outcome is an important source of morbidity in children with congenital heart disease (CHD). A significant proportion of newborns with complex CHD have abnormalities of brain size, structure, or function, which suggests that antenatal factors may contribute to childhood neurodevelopmental morbidity.
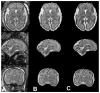
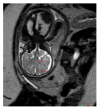
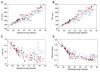
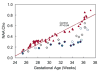
Methods and results: Brain volume and metabolism were compared prospectively between 55 fetuses with CHD and 50 normal fetuses with the use of 3-dimensinal volumetric magnetic resonance imaging and proton magnetic resonance spectroscopy. Fetal intracranial cavity volume, cerebrospinal fluid volume, and total brain volume were measured by manual segmentation. Proton magnetic resonance spectroscopy was used to measure the cerebral N-acetyl aspartate: choline ratio (NAA:choline) and identify cerebral lactate. Complete fetal echocardiograms were performed. Gestational age at magnetic resonance imaging ranged from 25 1/7 to 37 1/7 weeks (median, 30 weeks). During the third trimester, there were progressive and significant declines in gestational age-adjusted total brain volume and intracranial cavity volume in CHD fetuses relative to controls. NAA:choline increased progressively over the third trimester in normal fetuses, but the rate of rise was significantly slower (P<0.001) in CHD fetuses. On multivariable analysis adjusted for gestational age and weight percentile, cardiac diagnosis and percentage of combined ventricular output through the aortic valve were independently associated with total brain volume. Independent predictors of lower NAA:choline included diagnosis, absence of antegrade aortic arch flow, and evidence of cerebral lactate (P<0.001).
Conclusions: Third-trimester fetuses with some forms of CHD have smaller gestational age- and weight-adjusted total brain volumes than normal fetuses and evidence of impaired neuroaxonal development and metabolism. Hemodynamic factors may play an important role in this abnormal development.
Conflict of interest statement
Conflict of Interest Disclosures:
Figures

References
-
- Tabbutt S, Nord AS, Jarvik GP, Bernbaum J, Wernovsky G, Gerdes M, Zackai E, Clancy RR, Nicolson SC, Spray TL, Gaynor JW. Neurodevelopmental outcomes after staged palliation for hypoplastic left heart syndrome. Pediatrics. 2008;121:476–83. - PubMed
-
- Massaro AN, El-Dib M, Glass P, Aly H. Factors associated with adverse neurodevelopmental outcomes in infants with congenital heart disease. Brain Dev. 2008;30:437–46. - PubMed
-
- Ballweg JA, Wernovsky G, Gaynor JW. Neurodevelopmental outcomes following congenital heart surgery. Pediatr Cardiol. 2007;28:126–33. - PubMed
-
- Newburger JW, Jonas RA, Wernovsky G, Wypij D, Hickey PR, Kuban KCK, Farrell DM, Holmes GL, Helmers SL, Constantinou J, Carrazana E, Barlow JK, Walsh AZ, Lucius KC, Share JC, Wessel DL, Hanley FL, Mayer JE, Castaneda AR, Ware JH. A comparison of the perioperative neurologic effects of hypothermic circulatory arrest versus low-flow cardiopulmonary bypass in infant heart surgery. N Eng J Med. 1993;329:1057–64. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

