Trends in use of opioids for chronic noncancer pain among individuals with mental health and substance use disorders: the TROUP study
- PMID: 20026946
- PMCID: PMC2917238
- DOI: 10.1097/AJP.0b013e3181b99f35
Trends in use of opioids for chronic noncancer pain among individuals with mental health and substance use disorders: the TROUP study
Abstract
Objectives: Use of prescription opioids for chronic pain is increasing, as is abuse of these medications, though the nature of the link between these trends is unclear. These increases may be most marked in patients with mental health (MH) and substance use disorders (SUDs). We analyzed trends between 2000 and 2005 in opioid prescribing among individuals with noncancer pain conditions (NCPC), with and without MH and SUDs.
Methods: Secondary data analysis of longitudinal administrative data from 2 dissimilar populations: a national, commercially insured population and Arkansas Medicaid enrollees. We examined these opioid outcomes: (1) rates of any prescription opioid use in the past year, (2) rates of chronic use of prescription opioids (greater than 90 d in the past year), (3) mean days supply of opioids, (4) mean daily opioid dose in morphine equivalents, and (5) percentage of total opioid dose that was Schedule II opioids.
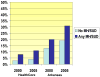
Results: In 2000, among individuals with NCPC, chronic opioid use was more common among those with a MH or SUD than among those without in commercially insured (8% vs. 3%, P<0.001) and Arkansas Medicaid (20% vs. 13%, P<0.001) populations. Between 2000 and 2005, in commercially insured, rates of chronic opioid use increased by 34.9% among individuals with an MH or SUD and 27.8% among individuals without these disorders. In Arkansas Medicaid chronic, opioid use increased by 55.4% among individuals with an MH or SUD and 39.8% among those without.
Discussion: Chronic use of prescription opioids for NCPC is much higher and growing faster in patients with MH and SUDs than in those without these diagnoses. Clinicians should monitor the use of prescription opioids in these vulnerable groups to determine whether opioids are substituting for or interfering with appropriate MH and substance abuse treatment.
Figures
Comment in
-
Comment on Edlund et al "trends in use of opioids for chronic noncancer pain among individuals with mental health and substance abuse disorders: the TROUP study".Clin J Pain. 2010 Sep;26(7):645. doi: 10.1097/AJP.0b013e3181d92d35. Clin J Pain. 2010. PMID: 20716971 No abstract available.
References
-
- Verhaak PF, Kerssens JJ, Dekker J, Sorbi MJ, Bensing JM. Prevalence of chronic benign pain disorder among adults: A review of the literature. Pain. 1998;77:231–239. - PubMed
-
- Gureje O, Von Korff M, Simon GE, Gater R. Persistent pain and well-being: A World Health Organization Study in Primary Care. Journal of the American Medical Association. 1998;280(2):147–151. - PubMed
-
- Zerzan JT, Morden NE, Soumerai S, et al. Trends and geographic variation of opiate medication use in state Medicaid fee-for-service programs, 1996 to 2002. Medical Care. 2006;44(11):1005–1010. - PubMed
-
- Eriksen J, Jensen MK, Sjogren P, Ekholm O, Rasmussen NK. Epidemiology of chronic non-malignant pain in Denmark. Pain. 2003;106(3):221–228. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous