Plasma bile acid concentrations in patients with human immunodeficiency virus infection receiving protease inhibitor therapy: possible implications for hepatotoxicity
- PMID: 20030469
- PMCID: PMC2856922
- DOI: 10.1592/phco.30.1.17
Plasma bile acid concentrations in patients with human immunodeficiency virus infection receiving protease inhibitor therapy: possible implications for hepatotoxicity
Abstract
Study objectives: To evaluate whether patients with human immunodeficiency virus (HIV) infection who were receiving protease inhibitor therapy had altered bile acid concentrations compared with noninfected control subjects, and whether bile acid concentrations could predict the onset of hepatotoxicity caused by protease inhibitors.
Design: Retrospective sample analysis from a prospectively conducted clinical trial.
Setting: Academic research center.
Patients: Eleven adults with advanced HIV disease who were taking protease inhibitor-based antiretroviral therapy, one of whom had developed protease inhibitor-induced hepatotoxicity.
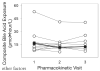
Measurements and main results: Plasma concentrations of cholic acid (CA), chenodeoxycholic acid (CDCA), deoxycholic acid (DCA), lithocholic acid (LCA), ursodeoxycholic acid (UDCA), and taurocholic acid (TC) were analyzed by using a novel high-performance liquid chromatography with tandem mass spectrometry detection method. Comparisons of the relative contribution of each bile acid to the total bile acid pool were made with previously published values and with bile acid concentrations contained in two pooled plasma samples from healthy, non-HIV-infected volunteers analyzed in our laboratory. Each pooled plasma sample used for this analysis contained contributions from three non-HIV-infected volunteers. The LCA and TC concentrations in HIV-infected patients were 3-4-fold higher than those previously reported for non-HIV-infected subjects; concentrations of other bile acids were similar to those of previous reports. The relative contribution of CDCA to the total bile acid pool was 9% in HIV-infected patients compared with 30-50% in noninfected subjects. Total and individual bile acid concentrations in the HIV-infected patient who developed hepatotoxicity were similar to the bile acid concentrations from the other study patients who did not develop hepatotoxicity.
Conclusion: These data suggest that bile acid concentrations may be altered by HIV infection and/or protease inhibitor therapy. However, further investigations should be performed to assess whether antiretroviral-associated hepatotoxicity can be predicted by alterations in individual bile acid concentrations.
Figures



References
-
- Bremmelgaard A, Sjovall J. Hydroxylation of cholic, chenodeoxycholic, and deoxycholic acids in patients with intrahepatic cholestasis. J Lipid Res. 1980;21:1072–81. - PubMed
-
- Bloomer JR, Allen RM, Klatskin G. Serum bile acids in primary biliary cirrhosis. Arch Intern Med. 1976;136:57–61. - PubMed
-
- Magyar I, Loi HG, Feher T. Plasma bile acid levels and liver disease. Acta Med Acad Sci Hung. 1981;38:109–15. - PubMed
-
- Azer SA, Coverdale SA, Byth K, Farrell GC, Stacey NH. Sequential changes in serum levels of individual bile acids in patients with chronic cholestatic liver disease. J Gastroenterol Hepatol. 1996;11:208–15. - PubMed
-
- Okuda H, Obata H, Nakanishi T, Hisamitsu T, Matsubara K, Watanabe H. Quantification of individual serum bile acids in patients with liver diseases using high-performance liquid chromatography. Hepatogastroenterology. 1984;31:168–71. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
