Using multidetector computed tomography in a swine model to assess the effects of sublingual nitroglycerin and intravenous adenosine on epicardial coronary arteries
- PMID: 20034433
- PMCID: PMC2798844
Using multidetector computed tomography in a swine model to assess the effects of sublingual nitroglycerin and intravenous adenosine on epicardial coronary arteries
Abstract
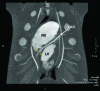
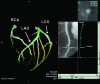
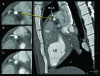
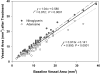
This study examines the effects of intravenous infusion of adenosine and sublingual nitroglycerin on coronary angiograms obtained by current-generation multidetector computed tomography. We assessed coronary vasodilation at baseline and after intravenous adenosine (140 microg/kg/min) or sublingual nitroglycerin spray (800 microg) in 7 female swine (weight, 40.9 +/- 1.4 kg) by using electrocardiogram-gated coronary angiography with a 64-detector scanner (rotation time, 400 ms; 120kV; 400 mA) and intravenous contrast (300 mg/mL iohexol, 4.5 mL/s, 2 mL/kg). Cross-sectional areas of segments in the left anterior descending, circumflex, and right coronary arteries were evaluated in oblique orthogonal views. Images were acquired at an average heart rate of 73 +/- 11 beats per minute. Changes in aortic pressure were not significant with nitroglycerin but decreased (approximately 10%) with adenosine. Of the 76 segments analyzed (baseline range, 2 to 39 mm2), 1 distal segment could not be assessed after adenosine. Segment cross-sectional area increased by 11.3% with nitroglycerin but decreased by 9.6% during adenosine infusion. The results of the present study are consistent with the practice of using sublingual nitroglycerin to enhance visualization of epicardial vessels and suggest that intravenous adenosine may hinder coronary artery visualization. This study is the first repeated-measures electrocardiogram-gated CT evaluation to use the same imaging technology to assess changes in coronary cross-sectional area before and after treatment with a vasodilator. The nitroglycerin-associated changes in our swine model were modest in comparison with previously reported human studies.
Figures

Similar articles
-
Coronary vasodilation by the use of sublingual nitroglycerin using 64-slice dual-source coronary computed tomography angiography.J Cardiol. 2015 Mar;65(3):230-6. doi: 10.1016/j.jjcc.2014.05.012. Epub 2014 Jun 30. J Cardiol. 2015. PMID: 24994019
-
Sublingual Nitroglycerin Administration in Coronary Computed Tomography Angiography: a Systematic Review.Eur Radiol. 2015 Dec;25(12):3536-42. doi: 10.1007/s00330-015-3791-3. Epub 2015 May 21. Eur Radiol. 2015. PMID: 25994194 Free PMC article.
-
Active and passive coronary vasodilation after intracoronary and sublingual nitroglycerin.Z Kardiol. 1983;72 Suppl 3:82-6. Z Kardiol. 1983. PMID: 6421018
-
Effects of nitroglycerin on the diagnostic accuracy of electrocardiogram-gated coronary computed tomography angiography.J Comput Assist Tomogr. 2008 Jan-Feb;32(1):86-92. doi: 10.1097/rct.0b013e318059befa. J Comput Assist Tomogr. 2008. PMID: 18303294
-
Contraindications and side effects of commonly used medications in coronary CT angiography.Int J Cardiovasc Imaging. 2011 Mar;27(3):441-9. doi: 10.1007/s10554-010-9654-8. Epub 2010 Jun 23. Int J Cardiovasc Imaging. 2011. PMID: 20571874 Review.
Cited by
-
The impact of spinal anesthesia on cardiac function in euvolemic vascular surgery patients: insights from echocardiography and biomarkers.Int J Cardiovasc Imaging. 2024 Nov;40(11):2305-2315. doi: 10.1007/s10554-024-03228-2. Epub 2024 Aug 28. Int J Cardiovasc Imaging. 2024. PMID: 39196451
-
Improved enhancement in CT angiography with reduced contrast media iodine concentrations at constant iodine dose.Sci Rep. 2018 Nov 30;8(1):17493. doi: 10.1038/s41598-018-35918-y. Sci Rep. 2018. PMID: 30504863 Free PMC article.
-
The Impact of Combining a Low-Tube Voltage Acquisition with Iterative Reconstruction on Total Iodine Dose in Coronary CT Angiography.Biomed Res Int. 2017;2017:2476171. doi: 10.1155/2017/2476171. Epub 2017 May 23. Biomed Res Int. 2017. PMID: 28620616 Free PMC article.
-
Impact of sublingual nitroglycerin dosage on FFRCT assessment and coronary luminal volume-to-myocardial mass ratio.Eur Radiol. 2019 Dec;29(12):6829-6836. doi: 10.1007/s00330-019-06293-7. Epub 2019 Jun 21. Eur Radiol. 2019. PMID: 31227880
References
-
- Abrams J. 1995. The role of nitrates in coronary heart disease. Arch Intern Med 155:357–364 - PubMed
-
- Asselbergs FW, Monnink SH, Veeger NJ, van Boven AJ, van Haelst PL, Jessurun GA, van Gilst WH, Tio RA. 2004. Coronary vasomotor response is related to the angiographic extent of coronary sclerosis in patients with stable angina pectoris. Clin Sci 106:115–120 - PubMed
-
- Bache RJ. 1998. Vasodilator reserve: a functional assessment of coronary health. Circulation 98:1257–1260 - PubMed
-
- Chun EJ, Lee W, Choi YH, Koo BK, Choi SI, Jae HJ, Kim HC, So YH, Chung JW, Park JH. 2008. Effects of nitroglycerin on the diagnostic accuracy of electrocardiogram-gated coronary computed tomography angiography. J Comput Assist Tomogr 32:86–92 - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
