Antibiotic susceptibility patterns of Pseudomonas aeruginosa at a tertiary care hospital in Gujarat, India
- PMID: 20040963
- PMCID: PMC2792624
- DOI: 10.4103/0253-7613.44156
Antibiotic susceptibility patterns of Pseudomonas aeruginosa at a tertiary care hospital in Gujarat, India
Abstract
Objectives: The present study was undertaken to assess the antibiotic susceptibility patterns of Pseudomonas aeruginosa at a tertiary care hospital in Gujarat, India. Due to significant changes in microbial genetic ecology, as a result of indiscriminate use of anti-microbials, the spread of anti-microbial resistance is now a global problem.
Materials and methods: Out of 276 culture positive samples, 56 samples of Pseudomonas aeruginosa were examined and 10 different types of specimen were collected. Microbial sensitivity testing was done using disk diffusion test with Pseudomonas species NCTC 10662, as per CLSI guidelines.
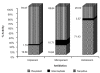
Results: The highest number of Pseudomonas infections was found in urine, followed by pus and sputum. Pseudomonas species demonstrated marked resistance against monotherapy of penicillins, cephalosporins, fluoroquinolones, tetracyclines and macrolides. Only combination drugs like Ticarcillin + Clavulanic acid, Piperacillin + Tazobactum, Cefoperazone + Sulbactum, Cefotaxime + Sulbactum, Ceftriaxome + Sulbactum and monotherapy of amikacin showed higher sensitivity to Pseudomonas infections; however, the maximum sensitivity was shown by the Carbapenems.
Conclusion: From the present study, we conclude that urinary tract infection was the most common hospital acquired infection. Also, co-administration of beta -lactamase inhibitors markedly expanded the anti-microbial sensitivity of semi-synthetic penicillins and cephalosporins. The aminoglycoside group of antibiotics - amikacin - demonstrated maximum sensitivity against pseudomonas species. Therefore, use of amikacin should be restricted to severe nosocomial infections, in order to avoid rapid emergence of resistant strains. Periodic susceptibility testing should be carried out over a period of two to three years, to detect the resistance trends. Also, a rational strategy on the limited and prudent use of anti-Pseudomonal agents is urgently required.
Keywords: Antimicrobial susceptibility; Pseudomonas aeruginosa; carbapenem sensitivity; combination antibiotics; disk diffusion technique.
Figures

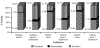
Similar articles
-
[Investigation of the frequency of PER-1 type beta-lactamase and antimicrobial resistance rates in nosocomial isolates of Pseudomonas aeruginosa].Mikrobiyol Bul. 2012 Jan;46(1):1-8. Mikrobiyol Bul. 2012. PMID: 22399165 Turkish.
-
Prevalence and Antimicrobial Susceptibility Pattern of Pseudomonas aeruginosa Isolates From Various Clinical Specimens in a Tertiary Care Hospital: An Analysis of Resistance Trends and Implications for Treatment Strategies.Cureus. 2024 Oct 28;16(10):e72556. doi: 10.7759/cureus.72556. eCollection 2024 Oct. Cureus. 2024. PMID: 39610569 Free PMC article.
-
Pseudomonas aeruginosa: Evaluation of Pathogen Burden and Drug-Resistance Trends in a Tertiary Care Hospital.J Coll Physicians Surg Pak. 2018 Apr;28(4):279-283. doi: 10.29271/jcpsp.2018.04.279. J Coll Physicians Surg Pak. 2018. PMID: 29615167
-
Antibiotic use in neonatal sepsis.Turk J Pediatr. 1998 Jan-Mar;40(1):17-33. Turk J Pediatr. 1998. PMID: 9722468 Review.
-
Aminoglycosides plus beta-lactams against gram-negative organisms. Evaluation of in vitro synergy and chemical interactions.Am J Med. 1986 Jun 30;80(6B):126-37. doi: 10.1016/0002-9343(86)90490-0. Am J Med. 1986. PMID: 3088998 Review.
Cited by
-
Incidence and Molecular Characterization of Carbapenemase Genes in Association with Multidrug-Resistant Clinical Isolates of Pseudomonas aeruginosa from Tertiary Healthcare Facilities in Southwest Nigeria.Curr Microbiol. 2021 Dec 14;79(1):27. doi: 10.1007/s00284-021-02706-3. Curr Microbiol. 2021. PMID: 34905085
-
Clinical Specimens are the Pool of Multidrug- resistant Pseudomonas aeruginosa Harbouring oprL and toxA Virulence Genes: Findings from a Tertiary Hospital of Nepal.Emerg Med Int. 2021 Oct 29;2021:4120697. doi: 10.1155/2021/4120697. eCollection 2021. Emerg Med Int. 2021. PMID: 34745664 Free PMC article.
-
Comparison of Antibiofilm Activity of Pseudomonas aeruginosa Phages on Isolates from Wounds of Diabetic and Non-Diabetic Patients.Microorganisms. 2023 Sep 4;11(9):2230. doi: 10.3390/microorganisms11092230. Microorganisms. 2023. PMID: 37764074 Free PMC article.
-
Detection of Metallo Beta-Lactamase (MBL) Producing Pseudomonas aeruginosa in a Tertiary Care Hospital, Ghanpur, Medchal, India.Maedica (Bucur). 2022 Mar;17(1):134-142. doi: 10.26574/maedica.2022.17.1.134. Maedica (Bucur). 2022. PMID: 35733755 Free PMC article.
-
Study of Antimicrobial Resistance, Biofilm Formation, and Motility of Pseudomonas aeruginosa Derived from Urine Samples.Microorganisms. 2023 May 19;11(5):1345. doi: 10.3390/microorganisms11051345. Microorganisms. 2023. PMID: 37317319 Free PMC article.
References
-
- Chastre J, Trouillet JL. Problem pathogens (Pseudomonas aeruginosa and Acinetobacter) Semin Respir Infect. 2000;15:287–98. - PubMed
-
- National Committee for Clinical Laboratory Standards. Approved standard M2 A7 NCCLS. Villanova, PA: 1995. Performance standards for antimicrobial disk susceptibility tests; p. 15.
-
- Das RN, Chandrasekhar TS, Joshi HS, Gurung M, Shrestha N, Shivananda PG. Frequency and susceptibility profile of pathogens causing urinary tract infections at a tertiary care hospital in western Nepal. Singapore Med J. 2006;47:281–5. - PubMed
LinkOut - more resources
Full Text Sources
Molecular Biology Databases

