Plasmodium infection and its risk factors in eastern Uganda
- PMID: 20044942
- PMCID: PMC2822788
- DOI: 10.1186/1475-2875-9-2
Plasmodium infection and its risk factors in eastern Uganda
Abstract
Background: Malaria is a leading cause of disease burden in Uganda, although surprisingly few contemporary, age-stratified data exist on malaria epidemiology in the country. This report presents results from a total population survey of malaria infection and intervention coverage in a rural area of eastern Uganda, with a specific focus on how risk factors differ between demographic groups in this population.
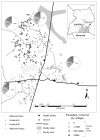
Methods: In 2008, a cross-sectional survey was conducted in four contiguous villages in Mulanda, sub-county in Tororo district, eastern Uganda, to investigate the epidemiology and risk factors of Plasmodium species infection. All permanent residents were invited to participate, with blood smears collected from 1,844 individuals aged between six months and 88 years (representing 78% of the population). Demographic, household and socio-economic characteristics were combined with environmental data using a Geographical Information System. Hierarchical models were used to explore patterns of malaria infection and identify individual, household and environmental risk factors.
Results: Overall, 709 individuals were infected with Plasmodium, with prevalence highest among 5-9 year olds (63.5%). Thin films from a random sample of 20% of parasite positive participants showed that 94.0% of infections were Plasmodium falciparum and 6.0% were P. malariae; no other species or mixed infections were seen. In total, 68% of households owned at least one mosquito although only 27% of school-aged children reported sleeping under a net the previous night. In multivariate analysis, infection risk was highest amongst children aged 5-9 years and remained high in older children. Risk of infection was lower for those that reported sleeping under a bed net the previous night and living more than 750 m from a rice-growing area. After accounting for clustering within compounds, there was no evidence for an association between infection prevalence and socio-economic status, and no evidence for spatial clustering.
Conclusion: These findings demonstrate that mosquito net usage remains inadequate and is strongly associated with risk of malaria among school-aged children. Infection risk amongst adults is influenced by proximity to potential mosquito breeding grounds. Taken together, these findings emphasize the importance of increasing net coverage, especially among school-aged children.
Figures

References
-
- Malaria Control Programme MoH. Uganda Malaria Control Strategic Plan 2005/06 - 2009/10.
-
- Snow RW, Marsh K. The consequences of reducing transmission of Plasmodium falciparum in Africa. Adv Parasitol. 2002;52:235–264. full_text. - PubMed
-
- Idro R, Bitarakwate E, Tumwesigye E, Chandy CJ. Clinical manifestations of severe malaria in the highlands of southwestern Uganda. Am J Trop Med Hyg. 2005;72:561–567. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

