Clinical features from the history and physical examination that predict the presence or absence of pulmonary embolism in symptomatic emergency department patients: results of a prospective, multicenter study
- PMID: 20045580
- PMCID: PMC2847003
- DOI: 10.1016/j.annemergmed.2009.11.010
Clinical features from the history and physical examination that predict the presence or absence of pulmonary embolism in symptomatic emergency department patients: results of a prospective, multicenter study
Abstract
Study objective: Prediction rules for pulmonary embolism use variables explicitly shown to estimate the probability of pulmonary embolism. However, clinicians often use variables that have not been similarly validated, yet are implicitly believed to modify probability of pulmonary embolism. The objective of this study is to measure the predictive value of 13 implicit variables.
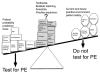
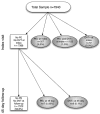
Methods: Patients were enrolled in a prospective cohort study from 12 centers in the United States; all had an objective test for pulmonary embolism (D-dimer, computed tomographic angiography, or ventilation-perfusion scan). Clinical features including 12 predefined previously validated (explicit) variables and 13 variables not part of existing prediction rules (implicit) were prospectively recorded at presentation. The primary outcome was venous thromboembolism (pulmonary embolism or deep venous thrombosis), diagnosed by imaging up to 45 days after enrollment. Variables with adjusted odds ratios from logistic regression with 95% confidence intervals not crossing unity were considered significant.
Results: Seven thousand nine hundred forty patients (7.2% venous thromboembolism positive) were enrolled. Mean age was 49 years (standard deviation 17 years) and 67% were female patients. Eight of 13 implicit variables were significantly associated with venous thromboembolism; those with an adjusted odds ratio (OR) greater than 1.5 included non-cancer-related thrombophilia (OR 1.99), pleuritic chest pain (OR 1.53), and family history of venous thromboembolism (OR 1.51). Implicit variables that predicted no venous thromboembolism outcome included substernal chest pain, female sex, and smoking. Nine of 12 explicit variables predicted a positive outcome of venous thromboembolism, including patient history of pulmonary embolism or deep venous thrombosis in the past, unilateral leg swelling, recent surgery, estrogen, hypoxemia, and active malignancy.
Conclusion: In symptomatic outpatients being considered for possible pulmonary embolism, non-cancer-related thrombophilia, pleuritic chest pain, and family history of venous thromboembolism increase probability of pulmonary embolism or deep venous thrombosis. Other variables that are part of existing pretest probability systems were validated as important predictors in this diverse sample of US emergency department patients.
Keywords: D-dimer; Prediction; decision rules; logistic regression; pulmonary embolism.
Copyright (c) 2009 American College of Emergency Physicians. Published by Mosby, Inc. All rights reserved.
Figures
Comment in
-
Problems with PERC.Ann Emerg Med. 2010 Nov;56(5):584-5; author reply 586-7. doi: 10.1016/j.annemergmed.2010.04.032. Ann Emerg Med. 2010. PMID: 21036302 No abstract available.
References
-
- McCaig LF, Nawar EW. National hospital ambulatory care survey: 2004 emergency department summary. Advance Data. 2006;372:1–29. - PubMed
-
- Kabrhel C, Matts C, McNamara C, et al. A highly sensitive ELISA D-dimer increases testing but not diagnosis of pulmonary embolism. Acad Emerg Med. 2006;13 (5):519–24. - PubMed
-
- Kline JA, Courtney DM, Beam DM, et al. Incidence and predictors of repeated computed tomographic pulmonary angiography in emergency department patients. Ann Emerg Med. 2008 epub ahead of print. - PubMed
-
- Wells PS, Anderson DR, Rodger M, et al. Derivation of a simple clinical model to categorize patients probability of pulmonary embolism: increasing the models utility with the SimpliRED D-dimer. Thromb Haemost. 2000;83 (3):416–20. - PubMed
-
- Wicki J, Perneger TV, Junod AF, et al. Assessing clinical probability of pulmonary embolism in the emergency ward: a simple score. Arch Intern Med. 2001;161 (1):92–7. - PubMed
Publication types
MeSH terms
Grants and funding
- R41HL074415/HL/NHLBI NIH HHS/United States
- 2R42HL074415-02A1/HL/NHLBI NIH HHS/United States
- L30 HL081998/HL/NHLBI NIH HHS/United States
- 1K23HL077404-01/HL/NHLBI NIH HHS/United States
- R41 HL074415/HL/NHLBI NIH HHS/United States
- K23 HL077404/HL/NHLBI NIH HHS/United States
- R01 HL074384/HL/NHLBI NIH HHS/United States
- R42 HL074415/HL/NHLBI NIH HHS/United States
- 5R42HL074415-03/HL/NHLBI NIH HHS/United States
- 5K23HL077404(01-05/HL/NHLBI NIH HHS/United States
- R42HL074415/HL/NHLBI NIH HHS/United States
- R01HL074384/HL/NHLBI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous