Deficit in decision-making in chronic, stable schizophrenia: from a reward and punishment perspective
- PMID: 20046370
- PMCID: PMC2796041
- DOI: 10.4306/pi.2009.6.1.26
Deficit in decision-making in chronic, stable schizophrenia: from a reward and punishment perspective
Abstract
Objective: We compared patients with chronic schizophrenia and normal controls with respect to decision-making ability. Measures were implemented to control for the participants' intelligence levels as well as to ensure to use of a moderate sample size. The goal of this study was to confirm inconsistent results from previous studies which had stemmed from too small of a sample size, highly variable performance of normal controls, and not controlling for intelligence as a confounding factor.
Methods: Fifty-two chronic stable schizophrenic inpatients and 55 healthy controls participated in the study. We controlled for intelligence by including subjects with intelligence quotient's (IQ) between 80 and 120, examining any differences in decision-making performance between groups on the Iowa Gambling Task (IGT). We also addressed several issues relating to performance on the IGT, such as working memory and clinical symptoms.
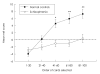
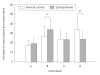
Results: Schizophrenic patients were found to perform poorly on the IGT relative to normal controls (F(1,105)=17.73, p<0.001); however, more importantly, they also displayed the slow yet profitable shift from disadvantageous decks to advantageous decks over time. We also found that when compared with healthy controls, schizophrenic patients showed a poorer performance on the Wisconsin Card Sorting Test (WCST)(t=-5.48, p<0.001 for perseverative error) which was not related to their performance on the IGT.
Conclusion: Based on previous literature and the results of this study, impaired sensitivity to both reward and punishment might be a more plausible explanation for the poor performance on the IGT in the schizophrenic group. We speculated that this impairment seemed related more to the different responsiveness to the magnitude than to the frequency of punishment, and to the different interpretation of less informative verbal cues in the context of the reinforcing schedule.
Keywords: Decision-making; Gambling task; Punishment; Reward; Schizophrenia.
Figures
Similar articles
-
Deficits in emotion based decision-making in schizophrenia; a new insight based on the Iowa Gambling Task.Prog Neuropsychopharmacol Biol Psychiatry. 2015 Mar 3;57:52-9. doi: 10.1016/j.pnpbp.2014.10.007. Epub 2014 Oct 24. Prog Neuropsychopharmacol Biol Psychiatry. 2015. PMID: 25455588
-
[Decision-making and schizophrenia].Encephale. 2011 Dec;37 Suppl 2:S110-6. doi: 10.1016/S0013-7006(11)70036-7. Encephale. 2011. PMID: 22212839 Review. French.
-
The Prominent Deck B Phenomenon in Schizophrenia: An Empirical Study on Iowa Gambling Task.Front Psychol. 2021 Sep 3;12:619855. doi: 10.3389/fpsyg.2021.619855. eCollection 2021. Front Psychol. 2021. PMID: 34539474 Free PMC article.
-
Integrating frequency and magnitude information in decision-making in schizophrenia: An account of patient performance on the Iowa Gambling Task.J Psychiatr Res. 2015 Jul-Aug;66-67:16-23. doi: 10.1016/j.jpsychires.2015.04.007. Epub 2015 Apr 28. J Psychiatr Res. 2015. PMID: 25959618 Free PMC article.
-
Decision-making and cognitive abilities: A review of associations between Iowa Gambling Task performance, executive functions, and intelligence.Clin Psychol Rev. 2010 Jul;30(5):562-81. doi: 10.1016/j.cpr.2010.04.002. Epub 2010 Apr 9. Clin Psychol Rev. 2010. PMID: 20457481 Review.
Cited by
-
Neural mechanisms regulating different forms of risk-related decision-making: Insights from animal models.Neurosci Biobehav Rev. 2015 Nov;58:147-67. doi: 10.1016/j.neubiorev.2015.04.009. Epub 2015 Jun 11. Neurosci Biobehav Rev. 2015. PMID: 26072028 Free PMC article. Review.
-
Similarities and Differences in Decision-Making Impairments between Autism Spectrum Disorder and Schizophrenia.Front Behav Neurosci. 2015 Sep 23;9:259. doi: 10.3389/fnbeh.2015.00259. eCollection 2015. Front Behav Neurosci. 2015. PMID: 26441583 Free PMC article.
-
Prevalence and correlates of diagnosed and undiagnosed epilepsy and migraine headache among people with severe psychiatric disorders in Ethiopia.PLoS One. 2020 Nov 20;15(11):e0241581. doi: 10.1371/journal.pone.0241581. eCollection 2020. PLoS One. 2020. PMID: 33216748 Free PMC article.
-
Motivational Deficits in Schizophrenia and the Representation of Expected Value.Curr Top Behav Neurosci. 2016;27:375-410. doi: 10.1007/7854_2015_385. Curr Top Behav Neurosci. 2016. PMID: 26370946 Free PMC article. Review.
-
Undiagnosed HIV, hepatitis B, and hepatitis C infections in people with severe psychiatric disorders in Ethiopia.BMC Infect Dis. 2020 Feb 27;20(1):180. doi: 10.1186/s12879-020-4907-1. BMC Infect Dis. 2020. PMID: 32106864 Free PMC article.
References
-
- Kraepelin E. Dementia praecox and paraphrenia. Edinburgh: Livingstone; 1919.
-
- Kuperberg G, Heckers S. Schizophrenia and cognitive function. Curr Opin Neurobiol. 2000;10:205–210. - PubMed
-
- Antonova E, Sharma T, Morris R, Kumari V. The relationship between brain structure and neurocognition in schizophrenia: a selective review. Schizophr Res. 2004;70:117–145. - PubMed
-
- Bilder RM, Lipschutz-Broch L, Reiter G, Geisler SH, Mayerhoff DI, Lieberman JA. Intellectual deficits in first-episode schizophrenia: evidence for progressive deterioration. Schizophr Bull. 1992;18:437–448. - PubMed
-
- Riley EM, McGovern D, Mockler D, Doku VC, OCeallaigh S, Fannon DG, et al. Neuropsychological functioning in first-episode psychosis--evidence of specific deficits. Schizophr Res. 2000;43:47–55. - PubMed
LinkOut - more resources
Full Text Sources

