Transglutaminase 2, a novel regulator of eicosanoid production in asthma revealed by genome-wide expression profiling of distinct asthma phenotypes
- PMID: 20052409
- PMCID: PMC2797392
- DOI: 10.1371/journal.pone.0008583
Transglutaminase 2, a novel regulator of eicosanoid production in asthma revealed by genome-wide expression profiling of distinct asthma phenotypes
Abstract
Background: A frequent manifestation of asthma, exercise-induced bronchoconstriction (EIB), occurs in 30-50% of asthmatics and is characterized by increased release of inflammatory eicosanoids. The objective of this study was to identify genes differentially expressed in EIB and to understand the function of these genes in the biology of asthma.
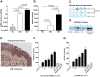
Methodology/principal findings: Genome-wide expression profiling of airway leukocytes and epithelial cells obtained by induced sputum was conducted in two groups of subjects with asthma with and without EIB (n = 7 per group), at baseline and following exercise challenge. Based on the results of the gene expression study, additional comparisons were made with a normal control group (n = 10). Localization studies were conducted on epithelial brushings and biopsies from an additional group of asthmatics with EIB (n = 3). Genes related to epithelial repair and mast cell infiltration including beta-tryptase and carboxypeptidase A3 were upregulated by exercise challenge in the asthma group with EIB. A gene novel to asthma pathogenesis, transglutaminase 2 (TGM2), was the most differentially expressed at baseline between the groups. In vivo studies confirmed the increased expression of TGM2 in airway cells and airway lining fluid, and demonstrate that TGM2 is avidly expressed in the asthmatic airway epithelium. In vitro studies using recombinant human enzymes reveal that TGM2 augments the enzymatic activity of secreted phospholipase A(2) (PLA(2)) group X (sPLA(2)-X), an enzyme recently implicated in asthma pathogenesis.
Conclusions/significance: This study found that TGM2, a mediator that is novel to asthma pathogenesis, is overexpressed in asthmatic airways and functions to increase sPLA(2)-X enzymatic activity. Since PLA(2) serves as the first rate-limiting step leading to eicosanoid formation, these results suggest that TGM2 may be a key initiator of the airway inflammatory cascade in asthma.
Conflict of interest statement
Figures

Similar articles
-
Epithelial regulation of eicosanoid production in asthma.Pulm Pharmacol Ther. 2012 Dec;25(6):432-7. doi: 10.1016/j.pupt.2012.02.004. Pulm Pharmacol Ther. 2012. PMID: 23323271 Free PMC article. Review.
-
New insights into pathogenesis of exercise-induced bronchoconstriction.Curr Opin Allergy Clin Immunol. 2012 Feb;12(1):42-8. doi: 10.1097/ACI.0b013e32834ecc67. Curr Opin Allergy Clin Immunol. 2012. PMID: 22157157 Free PMC article. Review.
-
Secreted phospholipase A2 group X overexpression in asthma and bronchial hyperresponsiveness.Am J Respir Crit Care Med. 2007 Dec 1;176(11):1072-8. doi: 10.1164/rccm.200707-1088OC. Epub 2007 Sep 27. Am J Respir Crit Care Med. 2007. PMID: 17901411 Free PMC article.
-
Exercise-induced alterations in phospholipid hydrolysis, airway surfactant, and eicosanoids and their role in airway hyperresponsiveness in asthma.Am J Physiol Lung Cell Mol Physiol. 2021 May 1;320(5):L705-L714. doi: 10.1152/ajplung.00546.2020. Epub 2021 Feb 3. Am J Physiol Lung Cell Mol Physiol. 2021. PMID: 33533300 Free PMC article.
-
Increased density of intraepithelial mast cells in patients with exercise-induced bronchoconstriction regulated through epithelially derived thymic stromal lymphopoietin and IL-33.J Allergy Clin Immunol. 2014 May;133(5):1448-55. doi: 10.1016/j.jaci.2013.08.052. Epub 2013 Nov 9. J Allergy Clin Immunol. 2014. PMID: 24220317 Free PMC article. Clinical Trial.
Cited by
-
Induced sputum proteome in healthy subjects and asthmatic patients.J Allergy Clin Immunol. 2011 Dec;128(6):1176-1184.e6. doi: 10.1016/j.jaci.2011.07.053. Epub 2011 Sep 8. J Allergy Clin Immunol. 2011. PMID: 21906793 Free PMC article.
-
PLA2G5 regulates transglutaminase activity of human IL-4-activated M2 macrophages through PGE2 generation.J Leukoc Biol. 2016 Jul;100(1):131-41. doi: 10.1189/jlb.3A0815-372R. Epub 2016 Mar 2. J Leukoc Biol. 2016. PMID: 26936936 Free PMC article.
-
Epithelial regulation of eicosanoid production in asthma.Pulm Pharmacol Ther. 2012 Dec;25(6):432-7. doi: 10.1016/j.pupt.2012.02.004. Pulm Pharmacol Ther. 2012. PMID: 23323271 Free PMC article. Review.
-
Transcription factor p63 regulates key genes and wound repair in human airway epithelial basal cells.Am J Respir Cell Mol Biol. 2013 Dec;49(6):978-88. doi: 10.1165/rcmb.2012-0447OC. Am J Respir Cell Mol Biol. 2013. PMID: 23837456 Free PMC article.
-
4,4'-Methylene diphenyl diisocyanate exposure induces expression of alternatively activated macrophage-associated markers and chemokines partially through Krüppel-like factor 4 mediated signaling in macrophages.Xenobiotica. 2023 Dec;53(12):653-669. doi: 10.1080/00498254.2023.2284867. Epub 2023 Dec 26. Xenobiotica. 2023. PMID: 38014489 Free PMC article.
References
-
- Cabral AL, Conceicao GM, Fonseca-Guedes CH, Martins MA. Exercise-induced bronchospasm in children: effects of asthma severity. Am J Respir Crit Care Med. 1999;159:1819–1823. - PubMed
-
- Hallstrand TS, Curtis JR, Koepsell TD, Martin DP, Schoene RB, et al. Effectiveness of screening examinations to detect unrecognized exercise-induced bronchoconstriction. J Pediatr. 2002;141:343–348. - PubMed
-
- Henriksen AH, Tveit KH, Holmen TL, Sue-Chu M, Bjermer L. A study of the association between exercise-induced wheeze and exercise versus methacholine-induced bronchoconstriction in adolescents. Pediatr Allergy Immunol. 2002;13:203–208. - PubMed
-
- Vianna EO, Boaventura LC, Terra-Filho J, Nakama GY, Martinez JA, et al. Morning-to-evening variation in exercise-induced bronchospasm. J Allergy Clin Immunol. 2002;110:236–240. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- R01HL072370/HL/NHLBI NIH HHS/United States
- 1S10RR021108-01/RR/NCRR NIH HHS/United States
- M01RR000037/RR/NCRR NIH HHS/United States
- P30ES07033/ES/NIEHS NIH HHS/United States
- M01 RR000037/RR/NCRR NIH HHS/United States
- 1S10RR019423-01/RR/NCRR NIH HHS/United States
- S10 RR019423/RR/NCRR NIH HHS/United States
- P30 ES007033/ES/NIEHS NIH HHS/United States
- S10 RR021108/RR/NCRR NIH HHS/United States
- R01HL089215/HL/NHLBI NIH HHS/United States
- R01 HL072370/HL/NHLBI NIH HHS/United States
- R01HL036253/HL/NHLBI NIH HHS/United States
- R01 HL089215/HL/NHLBI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases
Miscellaneous

