Ventilation with lower tidal volumes as compared with conventional tidal volumes for patients without acute lung injury: a preventive randomized controlled trial
- PMID: 20055989
- PMCID: PMC2875503
- DOI: 10.1186/cc8230
Ventilation with lower tidal volumes as compared with conventional tidal volumes for patients without acute lung injury: a preventive randomized controlled trial
Abstract
Introduction: Recent cohort studies have identified the use of large tidal volumes as a major risk factor for development of lung injury in mechanically ventilated patients without acute lung injury (ALI). We compared the effect of conventional with lower tidal volumes on pulmonary inflammation and development of lung injury in critically ill patients without ALI at the onset of mechanical ventilation.
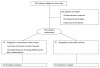
Methods: We performed a randomized controlled nonblinded preventive trial comparing mechanical ventilation with tidal volumes of 10 ml versus 6 ml per kilogram of predicted body weight in critically ill patients without ALI at the onset of mechanical ventilation. The primary end point was cytokine levels in bronchoalveolar lavage fluid and plasma during mechanical ventilation. The secondary end point was the development of lung injury, as determined by consensus criteria for ALI, duration of mechanical ventilation, and mortality.
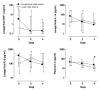
Results: One hundred fifty patients (74 conventional versus 76 lower tidal volume) were enrolled and analyzed. No differences were observed in lavage fluid cytokine levels at baseline between the randomization groups. Plasma interleukin-6 (IL-6) levels decreased significantly more strongly in the lower-tidal-volume group ((from 51 (20 to 182) ng/ml to 11 (5 to 20) ng/ml versus 50 (21 to 122) ng/ml to 21 (20 to 77) ng/ml; P = 0.01)). The trial was stopped prematurely for safety reasons because the development of lung injury was higher in the conventional tidal-volume group as compared with the lower tidal-volume group (13.5% versus 2.6%; P = 0.01). Univariate analysis showed statistical relations between baseline lung-injury score, randomization group, level of positive end-expiratory pressure (PEEP), the number of transfused blood products, the presence of a risk factor for ALI, and baseline IL-6 lavage fluid levels and the development of lung injury. Multivariate analysis revealed the randomization group and the level of PEEP as independent predictors of the development of lung injury.
Conclusions: Mechanical ventilation with conventional tidal volumes is associated with sustained cytokine production, as measured in plasma. Our data suggest that mechanical ventilation with conventional tidal volumes contributes to the development of lung injury in patients without ALI at the onset of mechanical ventilation.
Trial registration: ISRCTN82533884.
Figures


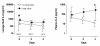

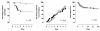
References
-
- Dreyfuss D, Saumon G. Ventilator-induced lung injury: lessons from experimental studies. Am J Respir Crit Care Med. 1998;157:294–323. - PubMed
-
- Amato MB, Barbas CS, Medeiros DM, Magaldi RB, Schettino GP, Lorenzi-Filho G, Kairalla RA, Deheinzelin D, Munoz C, Oliveira R, Takagaki TY, Carvalho CR. Effect of a protective-ventilation strategy on mortality in the acute respiratory distress syndrome. N Engl J Med. 1998;338:347–354. doi: 10.1056/NEJM199802053380602. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

