Flow measurement by cardiovascular magnetic resonance: a multi-centre multi-vendor study of background phase offset errors that can compromise the accuracy of derived regurgitant or shunt flow measurements
- PMID: 20074359
- PMCID: PMC2818657
- DOI: 10.1186/1532-429X-12-5
Flow measurement by cardiovascular magnetic resonance: a multi-centre multi-vendor study of background phase offset errors that can compromise the accuracy of derived regurgitant or shunt flow measurements
Abstract
Aims: Cardiovascular magnetic resonance (CMR) allows non-invasive phase contrast measurements of flow through planes transecting large vessels. However, some clinically valuable applications are highly sensitive to errors caused by small offsets of measured velocities if these are not adequately corrected, for example by the use of static tissue or static phantom correction of the offset error. We studied the severity of uncorrected velocity offset errors across sites and CMR systems.
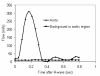
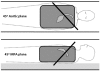
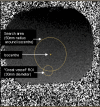
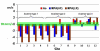
Methods and results: In a multi-centre, multi-vendor study, breath-hold through-plane retrospectively ECG-gated phase contrast acquisitions, as are used clinically for aortic and pulmonary flow measurement, were applied to static gelatin phantoms in twelve 1.5 T CMR systems, using a velocity encoding range of 150 cm/s. No post-processing corrections of offsets were implemented. The greatest uncorrected velocity offset, taken as an average over a 'great vessel' region (30 mm diameter) located up to 70 mm in-plane distance from the magnet isocenter, ranged from 0.4 cm/s to 4.9 cm/s. It averaged 2.7 cm/s over all the planes and systems. By theoretical calculation, a velocity offset error of 0.6 cm/s (representing just 0.4% of a 150 cm/s velocity encoding range) is barely acceptable, potentially causing about 5% miscalculation of cardiac output and up to 10% error in shunt measurement.
Conclusion: In the absence of hardware or software upgrades able to reduce phase offset errors, all the systems tested appeared to require post-acquisition correction to achieve consistently reliable breath-hold measurements of flow. The effectiveness of offset correction software will still need testing with respect to clinical flow acquisitions.
Figures

Similar articles
-
The clinical impact of phase offset errors and different correction methods in cardiovascular magnetic resonance phase contrast imaging: a multi-scanner study.J Cardiovasc Magn Reson. 2020 Sep 17;22(1):68. doi: 10.1186/s12968-020-00659-3. J Cardiovasc Magn Reson. 2020. PMID: 32938483 Free PMC article.
-
In-vivo validation of interpolation-based phase offset correction in cardiovascular magnetic resonance flow quantification: a multi-vendor, multi-center study.J Cardiovasc Magn Reson. 2019 May 20;21(1):30. doi: 10.1186/s12968-019-0538-3. J Cardiovasc Magn Reson. 2019. PMID: 31104632 Free PMC article.
-
Effect of protocol choice on phase contrast cardiac magnetic resonance flow measurement in the ascending aorta: breath-hold and non-breath-hold.Int J Cardiovasc Imaging. 2013 Jan;29(1):113-20. doi: 10.1007/s10554-012-0047-z. Epub 2012 Apr 22. Int J Cardiovasc Imaging. 2013. PMID: 22527258
-
Flow measurement by magnetic resonance: a unique asset worth optimising.J Cardiovasc Magn Reson. 2007;9(4):723-8. doi: 10.1080/10976640701465090. J Cardiovasc Magn Reson. 2007. PMID: 17613655 Review.
-
Comprehensive 4D velocity mapping of the heart and great vessels by cardiovascular magnetic resonance.J Cardiovasc Magn Reson. 2011 Jan 14;13(1):7. doi: 10.1186/1532-429X-13-7. J Cardiovasc Magn Reson. 2011. PMID: 21235751 Free PMC article. Review.
Cited by
-
Cardiac output and cardiac index measured with cardiovascular magnetic resonance in healthy subjects, elite athletes and patients with congestive heart failure.J Cardiovasc Magn Reson. 2012 Jul 28;14(1):51. doi: 10.1186/1532-429X-14-51. J Cardiovasc Magn Reson. 2012. PMID: 22839436 Free PMC article.
-
Inter-study reproducibility of interleaved spiral phase velocity mapping of renal artery haemodynamics.J Cardiovasc Magn Reson. 2015 Feb 4;17(1):8. doi: 10.1186/s12968-014-0105-x. J Cardiovasc Magn Reson. 2015. PMID: 25648103 Free PMC article.
-
Sequence optimization to reduce velocity offsets in cardiovascular magnetic resonance volume flow quantification--a multi-vendor study.J Cardiovasc Magn Reson. 2011 Mar 9;13(1):18. doi: 10.1186/1532-429X-13-18. J Cardiovasc Magn Reson. 2011. PMID: 21388521 Free PMC article.
-
Deep Learning Automated Background Phase Error Correction for Abdominopelvic 4D Flow MRI.Radiology. 2022 Mar;302(3):584-592. doi: 10.1148/radiol.2021211270. Epub 2021 Nov 30. Radiology. 2022. PMID: 34846200 Free PMC article.
-
The measurement of CSF flow through the aqueduct in normal and hydrocephalic children: from where does it come, to where does it go?Childs Nerv Syst. 2012 Jan;28(1):55-63. doi: 10.1007/s00381-011-1617-4. Epub 2011 Oct 27. Childs Nerv Syst. 2012. PMID: 22038153
References
-
- Petersen SE, Voigtlander T, Kreitner KF, Kalden P, Wittlinger T, Scharhag J, Horstick G, Becker D, Hommel G, Thelen M, Meyer J. Quantification of shunt volumes in congenital heart diseases using a breath-hold MR phase contrast technique--comparison with oximetry. Int J Cardiovasc Imaging. 2002;18(1):53–60. doi: 10.1023/A:1014394626363. - DOI - PubMed
-
- Rebergen SA, Chin JGL, Ottenkamp J, Wall EE van der, de Roos A. Pulmonary regurgitation in the late post-operative follow-up of tetralogy of Fallot: volumetric quantification by nuclear magnetic resonance velocity mapping. Circulation. 1993;88:2257–66. - PubMed
-
- Gelfand EV, Hughes S, Hauser TH, Yeon SB, Goepfert L, Kissinger KV, Rofsky NM, Manning WJ. Severity of mitral and aortic regurgitation as assessed by cardiovascular magnetic resonance: optimizing correlation with Doppler echocardiography. J Cardiovasc Magn Reson. 2006;8(3):503–7. doi: 10.1080/10976640600604856. - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

