Carbodiimide-derivatized hyaluronic acid surface modification of lyophilized flexor tendon: a biomechanical study in a canine in vitro model
- PMID: 20124066
- PMCID: PMC6948808
- DOI: 10.2106/JBJS.H.01641
Carbodiimide-derivatized hyaluronic acid surface modification of lyophilized flexor tendon: a biomechanical study in a canine in vitro model
Abstract
Background: Intrasynovial grafts are the ideal solution to replace defects in intrasynovial flexor tendons, but autologous graft sources are rarely available. The purpose of the present study was to test the hypotheses that an intrasynovial tendon prepared with repetitive freeze-thaw cycles and lyophilization (as a means of reducing immunogenicity) has increased frictional force (gliding resistance) in comparison with fresh intrasynovial tendons and that a lyophilized intrasynovial flexor tendon that is modified with carbodiimide-derivatized hyaluronic acid and gelatin has decreased frictional force in comparison with untreated lyophilized tendons.
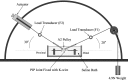
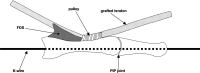
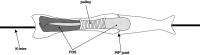
Methods: Thirty-six flexor digitorum profundus tendons from the second and fifth digits of canine hind paws were randomly assigned to three groups. Twelve tendons were immediately assessed both mechanically and morphologically and served as the normal tendon group. The other twenty-four tendons were prepared with repetitive freeze-thaw cycles and lyophilization and were randomly assigned to two groups, including one group in which the tendons were treated with carbodiimide-derivatized hyaluronic acid and gelatin and one group in which the tendons were not treated. The frictional force was measured during 1000 cycles of simulated flexion-extension motion in all tendons, and the mean frictional forces were compared. The tendons were then observed with use of transmitted light microscopy for residual hyaluronic acid on the tendon surface, and the smoothness of the surface was evaluated with use of scanning electron microscopy.
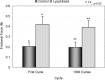
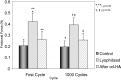
Results: The frictional force after lyophilization was significantly increased by 104.9% after the first cycle and by 99.5% after 1000 cycles in comparison with the normal tendon (p < 0.05). The frictional force of the lyophilized tendons after treatment with carbodiimide-derivatized hyaluronic acid and gelatin was not significantly different from that of normal tendons. The untreated lyophilized tendon surfaces were observed on scanning electron microscopy to be rough in appearance, whereas the normal surface and the surface treated with carbodiimide-derivatized hyaluronic acid and gelatin were smooth, with residual hyaluronic acid present on the gliding surface.
Conclusions: Lyophilization alters tendon surface morphology and increases tendon frictional force. Surface modification with carbodiimide-derivatized hyaluronic acid and gelatin can mitigate this adverse effect.
Clinical relevance: Tendon surface modification with carbodiimide-derivatized hyaluronic acid and gelatin can improve the gliding ability of lyophilized flexor tendons and therefore may improve the utility of lyophilized tendon allografts as a tendon graft substitute.
Figures


Similar articles
-
Improvement of flexor tendon reconstruction with carbodiimide-derivatized hyaluronic acid and gelatin-modified intrasynovial allografts: study of a primary repair failure model.J Bone Joint Surg Am. 2010 Dec 1;92(17):2817-28. doi: 10.2106/JBJS.I.01148. J Bone Joint Surg Am. 2010. PMID: 21123612 Free PMC article.
-
Surface treatment of flexor tendon autografts with carbodiimide-derivatized hyaluronic Acid. An in vivo canine model.J Bone Joint Surg Am. 2006 Oct;88(10):2181-91. doi: 10.2106/JBJS.E.00871. J Bone Joint Surg Am. 2006. PMID: 17015595 Free PMC article.
-
Lubricin surface modification improves extrasynovial tendon gliding in a canine model in vitro.J Bone Joint Surg Am. 2008 Jan;90(1):129-35. doi: 10.2106/JBJS.G.00045. J Bone Joint Surg Am. 2008. PMID: 18171967
-
The use of hyaluronic acid after tendon surgery and in tendinopathies.Biomed Res Int. 2014;2014:783632. doi: 10.1155/2014/783632. Epub 2014 May 8. Biomed Res Int. 2014. PMID: 24895610 Free PMC article. Review.
-
Hyaluronic acid and tendon lesions.Muscles Ligaments Tendons J. 2016 Feb 13;5(4):264-9. doi: 10.11138/mltj/2015.5.4.264. eCollection 2015 Oct-Dec. Muscles Ligaments Tendons J. 2016. PMID: 26958533 Free PMC article. Review.
Cited by
-
The effects of hylan g-f 20 surface modification on gliding of extrasynovial canine tendon grafts in vitro.J Hand Surg Am. 2013 Feb;38(2):231-6. doi: 10.1016/j.jhsa.2012.11.012. Epub 2013 Jan 5. J Hand Surg Am. 2013. PMID: 23294647 Free PMC article.
-
Design strategies for composite matrix and multifunctional polymeric scaffolds with enhanced bioactivity for bone tissue engineering.Front Chem. 2022 Nov 28;10:1051678. doi: 10.3389/fchem.2022.1051678. eCollection 2022. Front Chem. 2022. PMID: 36518978 Free PMC article. Review.
-
Repopulation of intrasynovial flexor tendon allograft with bone marrow stromal cells: an ex vivo model.Tissue Eng Part A. 2014 Feb;20(3-4):566-74. doi: 10.1089/ten.TEA.2013.0284. Epub 2013 Nov 21. Tissue Eng Part A. 2014. PMID: 24024566 Free PMC article.
-
The Effect of Gelatin Molecular Weight on Tendon Lubrication Utilizing an Extrasynovialized Turkey Flexor Tendon Model.Mil Med. 2021 Jan 25;186(Suppl 1):729-736. doi: 10.1093/milmed/usaa265. Mil Med. 2021. PMID: 33499438 Free PMC article.
-
Surface treatment of flexor tendon autograft and allograft decreases adhesion without an effect of graft cellularity: a pilot study.Clin Orthop Relat Res. 2012 Sep;470(9):2522-7. doi: 10.1007/s11999-012-2437-x. Clin Orthop Relat Res. 2012. PMID: 22744202 Free PMC article.
References
-
- Kleinert HE Schepel S Gill T. Flexor tendon injuries. Surg Clin North Am. 1981;61:267-86. - PubMed
-
- Lister GD Kleinert HE Kutz JE Atasoy E. Primary flexor tendon repair followed by immediate controlled mobilization. J Hand Surg Am. 1977;2:441-51. - PubMed
-
- Chow JA Thomes LJ Dovelle S Milnor WH Seyfer AE Smith AC. A combined regimen of controlled motion following flexor tendon repair in "no man's land". Plast Reconstr Surg. 1987;79:447-55. - PubMed
-
- Small JO Brennen MD Colville J. Early active mobilisation following flexor tendon repair in zone 2. J Hand Surg Br. 1989;14:383-91. - PubMed
-
- Strickland JW. Flexor tendon surgery. Part 1: primary flexor tendon repair. J Hand Surg Br. 1989;14:261-72. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

