Markedly reduced toxicity of a hydrogen sulphide-releasing derivative of naproxen (ATB-346)
- PMID: 20128814
- PMCID: PMC2848928
- DOI: 10.1111/j.1476-5381.2009.00611.x
Markedly reduced toxicity of a hydrogen sulphide-releasing derivative of naproxen (ATB-346)
Abstract
Background and purpose: Hydrogen sulphide is an important mediator of gastric mucosal defence. The use of non-steroidal anti-inflammatory drugs continues to be limited by their toxicity, particularly in the upper gastrointestinal tract. We evaluated the gastrointestinal safety and anti-inflammatory efficacy of a novel hydrogen sulphide-releasing derivative of naproxen, ATB-346 [2-(6-methoxy-napthalen-2-yl)-propionic acid 4-thiocarbamoyl-phenyl ester].
Experimental approach: The ability of ATB-346 versus naproxen to cause gastric damage was evaluated in healthy rats and in rats with compromised gastric mucosal defence. Effects on the small intestine and on the healing of ulcers were also assessed. The ability of ATB-346 to inhibit cyclooxygenase-1 and 2 and to reduce inflammation in vivo was also evaluated.
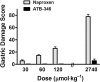
Key results: ATB-346 suppressed gastric prostaglandin E(2) synthesis as effectively as naproxen, but produced negligible damage in the stomach and intestine. In situations in which the gastric mucosa was rendered significantly more susceptible to naproxen-induced damage (e.g. ablation of sensory afferent nerves, inhibition of endogenous nitric oxide or hydrogen sulphide synthesis, co-administration with aspirin, antagonism of K(IR)6.x channels), ATB-346 did not cause significant damage. Unlike naproxen and celecoxib, ATB-346 accelerated healing of pre-existing gastric ulcers. In a mouse airpouch model, ATB-346 suppressed cyclooxygenase-2 activity and inhibited leukocyte infiltration more effectively than naproxen. ATB-346 was as effective as naproxen in adjuvant-induced arthritis in rats, with a more rapid onset of activity. Unlike naproxen, ATB-346 did not elevate blood pressure in hypertensive rats.
Conclusions and implications: ATB-346 exhibits anti-inflammatory properties similar to naproxen, but with substantially reduced gastrointestinal toxicity.
Figures







Similar articles
-
Gastroprotective and ulcer healing effects of nitric oxide-releasing non-steroidal anti-inflammatory drugs.Dig Liver Dis. 2000 Oct;32(7):583-94. doi: 10.1016/s1590-8658(00)80840-3. Dig Liver Dis. 2000. PMID: 11142556
-
Physiological healing of chronic gastric ulcer is not impaired by the hydrogen sulphide (H2S)-releasing derivative of acetylsalicylic acid (ATB-340): functional and proteomic approaches.Inflammopharmacology. 2024 Jun;32(3):2049-2060. doi: 10.1007/s10787-024-01458-3. Epub 2024 Apr 3. Inflammopharmacology. 2024. PMID: 38570398
-
The effect of hydrogen sulfide-releasing naproxen (ATB-346) versus naproxen on formation of stress-induced gastric lesions, the regulation of systemic inflammation, hypoxia and alterations in gastric microcirculation.J Physiol Pharmacol. 2017 Oct;68(5):749-756. J Physiol Pharmacol. 2017. PMID: 29375050
-
NSAIDs, coxibs, CINOD and H2S-releasing NSAIDs: what lies beyond the horizon.Dig Liver Dis. 2007 Dec;39(12):1043-51. doi: 10.1016/j.dld.2007.09.001. Epub 2007 Nov 7. Dig Liver Dis. 2007. PMID: 17997373 Review.
-
New insight into the mechanisms of gastroduodenal injury induced by nonsteroidal anti-inflammatory drugs: practical implications.Pol Arch Med Wewn. 2015;125(3):191-8. doi: 10.20452/pamw.2715. Epub 2015 Feb 10. Pol Arch Med Wewn. 2015. PMID: 25666703 Review.
Cited by
-
Hydrogen Sulfide in Physiology and Diseases of the Digestive Tract.Microorganisms. 2015 Nov 12;3(4):866-89. doi: 10.3390/microorganisms3040866. Microorganisms. 2015. PMID: 27682122 Free PMC article. Review.
-
Hydrogen sulfide-based therapeutics: exploiting a unique but ubiquitous gasotransmitter.Nat Rev Drug Discov. 2015 May;14(5):329-45. doi: 10.1038/nrd4433. Epub 2015 Apr 7. Nat Rev Drug Discov. 2015. PMID: 25849904 Review.
-
Hydrogen sulfide: a rescue molecule for mucosal defence and repair.Dig Dis Sci. 2012 Jun;57(6):1432-4. doi: 10.1007/s10620-012-2119-2. Dig Dis Sci. 2012. PMID: 22427131 No abstract available.
-
Exposure to non-steroid anti-inflammatory drugs (NSAIDs) and suppressing hydrogen sulfide synthesis leads to altered structure and impaired function of the oesophagus and oesophagogastric junction.Inflammopharmacology. 2015 Jun;23(2-3):91-9. doi: 10.1007/s10787-015-0230-7. Epub 2015 Feb 25. Inflammopharmacology. 2015. PMID: 25711289
-
Homeostatic impact of sulfite and hydrogen sulfide on cysteine catabolism.Br J Pharmacol. 2019 Feb;176(4):554-570. doi: 10.1111/bph.14464. Epub 2018 Sep 27. Br J Pharmacol. 2019. PMID: 30088670 Free PMC article. Review.
References
-
- Andruski B, McCafferty DM, Ignacy T, Millen B, McDougall JJ. Leukocyte trafficking and pain behavioral responses to a hydrogen sulphide donor in acute monoarthritis. Am J Physiol. 2008;295:R814–R820. - PubMed
-
- Brand SJ, Morise Z, Tagerud S, Mazzola L, Granger DN, Grisham MB. Role of the proteasome in rat indomethacin-induced gastropathy. Gastroenterology. 1999;116:865–873. - PubMed
-
- Brown JF, Keates AC, Hanson PJ, Whittle BJ. Nitric oxide generators and cGMP stimulate mucus secretion by rat gastric mucosal cells. Am J Physiol. 1993;265:G418–G422. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

