Magnetic resonance molecular imaging of thrombosis in an arachidonic acid mouse model using an activated platelet targeted probe
- PMID: 20139362
- PMCID: PMC2864133
- DOI: 10.1161/ATVBAHA.109.198556
Magnetic resonance molecular imaging of thrombosis in an arachidonic acid mouse model using an activated platelet targeted probe
Abstract
Objective: Atherosclerotic plaque rupture leads to acute thrombus formation and may trigger serious clinical events such as myocardial infarction or stroke. Therefore, it would be valuable to identify atherothrombosis and vulnerable plaques before the onset of such clinical events. We sought to determine whether the noninvasive in vivo visualization of activated platelets was effective when using a target-specific MRI contrast agent to identify thrombi, hallmarks of vulnerable or high-risk atherosclerotic plaques.
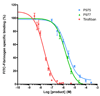
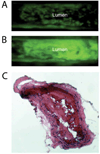
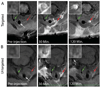
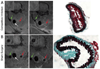
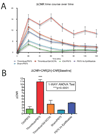
Methods and results: Inflammatory thrombi were induced in mice via topical application of arachidonic acid on the carotid. Thrombus formation was imaged with intravital fluorescence microscopy and molecular MRI. To accomplish the latter, a paramagnetic contrast agent (P975) that targets the glycoprotein alpha(IIb)beta(3), expressed on activated platelets, was investigated. The specificity of P975 for activated platelets was studied in vitro. In vivo, high spatial-resolution MRI was performed at baseline and longitudinally over 2 hours after injecting P975 or a nonspecific agent. The contralateral carotid, a sham surgery group, and a competitive inhibition experiment served as controls. P975 showed a good affinity for activated platelets, with an IC(50) (concentration of dose that produces 50% inhibition) value of 2.6 micromol/L. In thrombosed animals, P975 produced an immediate and sustained increase in MRI signal, whereas none of the control groups revealed any significant increase in MRI signal 2 hours after injection. More important, the competitive inhibition experiment with an alpha(IIb)beta(3) antagonist suppressed the MRI signal enhancement, which is indicative for the specificity of P975 for the activated platelets.
Conclusions: P975 allowed in vivo target-specific noninvasive MRI of activated platelets.
Figures
References
-
- Sanz J, Fayad ZA. Imaging of atherosclerotic cardiovascular disease. Nature. 2008;451:953–957. - PubMed
-
- Fuster V, Moreno PR, Fayad ZA, Corti R, Badimon JJ. Atherothrombosis and high-risk plaque: part I: evolving concepts. J Am Coll Cardiol. 2005;46:937–954. - PubMed
-
- Anderson JL, Adams CD, Antman EM, Bridges CR, Califf RM, Casey DE, Chavey WE, Fesmire FM, Hochman JS, Levin TN, Lincoff AM, Peterson ED, Theroux P, Wenger NK, Wright RS, Smith SC, Jacobs AK, Halperin JL, Hunt SA, Krumholz HM, Kushner FG, Lytle BW, Nishimura R, Ornato JP, Page RL, Riegel B. American College of Cardiology, American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 2002 Guidelines for the Management of Patients With Unstable Angina/Non-ST-Elevation Myocardial Infarction), American College of Emergency Physicians, Society for Cardiovascular Angiography and Interventions, Society of Thoracic Surgeons, American Association of Cardiovascular and Pulmonary Rehabilitation Society for Academic Emergency Medicine. ACC/AHA 2007 guidelines for the management of patients with unstable angina/non-ST-Elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 2002 Guidelines for the Management of Patients With Unstable Angina/Non-ST-Elevation Myocardial Infarction) developed in collaboration with the American College of Emergency Physicians, the Society for Cardiovascular Angiography and Interventions, and the Society of Thoracic Surgeons endorsed by the American Association of Cardiovascular and Pulmonary Rehabilitation and the Society for Academic Emergency Medicine. J Am Coll Cardiol. 2007;50:e1–e157. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

