Risk factors for multidrug resistant bacteria and optimization of empirical antibiotic therapy in postoperative peritonitis
- PMID: 20156360
- PMCID: PMC2875535
- DOI: 10.1186/cc8877
Risk factors for multidrug resistant bacteria and optimization of empirical antibiotic therapy in postoperative peritonitis
Abstract
Introduction: The main objective was to determine risk factors for presence of multidrug resistant bacteria (MDR) in postoperative peritonitis (PP) and optimal empirical antibiotic therapy (EA) among options proposed by Infectious Disease Society of America and the Surgical Infection Society guidelines.
Methods: One hundred patients hospitalised in the intensive care unit (ICU) for PP were reviewed. Clinical and microbiologic data, EA and its adequacy were analysed. The in vitro activities of 9 antibiotics in relation to the cultured bacteria were assessed to propose the most adequate EA among 17 regimens in the largest number of cases.
Results: A total of 269 bacteria was cultured in 100 patients including 41 episodes with MDR. According to logistic regression analysis, the use of broad-spectrum antibiotic between initial intervention and reoperation was the only significant risk factor for emergence of MDR bacteria (odds ratio (OR) = 5.1; 95% confidence interval (CI) = 1.7 - 15; P = 0.0031). Antibiotics providing the best activity rate were imipenem/cilastatin (68%) and piperacillin/tazobactam (53%). The best adequacy for EA was obtained by combinations of imipenem/cilastatin or piperacillin/tazobactam, amikacin and a glycopeptide, with values reaching 99% and 94%, respectively. Imipenem/cilastin was the only single-drug regimen providing an adequacy superior to 80% in the absence of broad spectrum antibiotic between initial surgery and reoperation.
Conclusions: Interval antibiotic therapy is associated with the presence of MDR bacteria. Not all regimens proposed by Infectious Disease Society of America and the Surgical Infection Society guidelines for PP can provide an acceptable rate of adequacy. Monotherapy with imipenem/cilastin is suitable for EA only in absence of this risk factor for MDR. For other patients, only antibiotic combinations may achieve high adequacy rates.
Figures
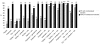
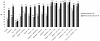
References
-
- Solomkin JS, Mazuski JE, Baron EJ, Sawyer RG, Nathens AB, DiPiro JT, Buchman T, Dellinger EP, Jernigan J, Gorbach S, Chow AW, Bartlett J. Infectious Diseases Society of America. Guidelines for the selection of anti-infective agents for complicated intra-abdominal infections. Clin Infect Dis. 2003;37:997–1005. doi: 10.1086/378702. - DOI - PubMed
-
- Mazuski JE, Sawyer RG, Nathens AB, DiPiro JT, Schein M, Kudsk KA, Yowler C. Therapeutic Agents Committee of the Surgical Infections Society. The Surgical Infection Society guidelines on antimicrobial therapy for intra-abdominal infections: an executive summary. Surg Infect (Larchmt) 2002;3:161–173. doi: 10.1089/109629602761624171. - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

