Ten-year follow-up of giant basilar aneurysm treated by sole stenting technique: a case report
- PMID: 20175900
- PMCID: PMC2843709
- DOI: 10.1186/1752-1947-4-64
Ten-year follow-up of giant basilar aneurysm treated by sole stenting technique: a case report
Abstract
Introduction: The sole stenting technique has emerged as a new tool for the management of intracranial aneurysms. However, several concerns have emerged about the long-term behavior of intracranial stents, particularly their safety and efficacy.
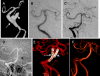
Case presentation: We present the first case of an intracranial aneurysm intentionally treated with the sole stenting technique. After ten years of clinical and imaging follow-up, the lesion has healed and no intrastent stenosis is observed.Several issues concerning this technique are discussed. For instance, the modification of the angle and intra-aneurysmal thrombosis may account as positive effects; negative outcomes include in-stent thrombosis or stenosis.
Conclusions: This case report, involving a long clinical and imaging follow-up, provides an example of the effectiveness, safety, durability and simplicity of the sole stenting technique in the management of intracranial aneurysms.
Figures

Similar articles
-
Sole stenting of large and giant intracranial aneurysms with self-expanding intracranial stents-limits and complications.Acta Neurochir (Wien). 2010 May;152(5):763-9. doi: 10.1007/s00701-009-0592-y. Epub 2010 Jan 27. Acta Neurochir (Wien). 2010. PMID: 20101418
-
Sole stenting technique for the treatment of uncoilable very small aneurysms in the intracranial internal carotid artery.Neurol Med Chir (Tokyo). 2013;53(5):310-7. doi: 10.2176/nmc.53.310. Neurol Med Chir (Tokyo). 2013. PMID: 23708222
-
Efficacy and current limitations of intravascular stents for intracranial internal carotid, vertebral, and basilar artery aneurysms.J Neurosurg. 1999 Oct;91(4):538-46. doi: 10.3171/jns.1999.91.4.0538. J Neurosurg. 1999. PMID: 10507372
-
Nonoverlapping Y-configuration stenting technique with dual closed-cell stents in wide-neck basilar tip aneurysms.Neurosurgery. 2012 Jun;70(2 Suppl Operative):244-9. doi: 10.1227/NEU.0b013e31823bcdc5. Neurosurgery. 2012. PMID: 21993186 Review.
-
Endovascular stenting for treatment of mycotic intracranial aneurysms.J Clin Neurosci. 2014 Jul;21(7):1163-8. doi: 10.1016/j.jocn.2013.11.013. Epub 2013 Dec 14. J Clin Neurosci. 2014. PMID: 24518267 Review.
Cited by
-
Closed-Cell Stent-Assisted Coiling of Intracranial Aneurysms: Evaluation of Changes in Vascular Geometry Using Digital Subtraction Angiography.PLoS One. 2016 Apr 13;11(4):e0153403. doi: 10.1371/journal.pone.0153403. eCollection 2016. PLoS One. 2016. PMID: 27073908 Free PMC article.
-
Rupture of Persistent Primitive Trigeminal Artery-basilar Artery Aneurysm Managed with Stent-assisted Coiling.Asian J Neurosurg. 2018 Jul-Sep;13(3):817-821. doi: 10.4103/ajns.AJNS_53_16. Asian J Neurosurg. 2018. PMID: 30283555 Free PMC article.
-
Disappearance of a small intracranial aneurysm as a result of vessel straightening and in-stent stenosis following use of an Enterprise vascular reconstruction device.BMJ Case Rep. 2013 Jan 17;2013:bcr2012010583. doi: 10.1136/bcr-2012-010583. BMJ Case Rep. 2013. PMID: 23329725 Free PMC article.
References
-
- Zenteno MA, Santos-Franco JA, Freitas-Modenesi JM, Gómez C, Murillo-Bonilla L, Aburto-Murrieta Y, Díaz-Romero R, Nathal E, Gómez-Llata S, Lee A. Use of the sole stenting technique for the management of aneurysms in the posterior circulation in a prospective series of 20 patients. J Neurosurg. 2008;108:1104–1118. doi: 10.3171/JNS/2008/108/6/1104. - DOI - PubMed

