Membranoproliferative glomerulonephritis secondary to monoclonal gammopathy
- PMID: 20185597
- PMCID: PMC2863981
- DOI: 10.2215/CJN.06760909
Membranoproliferative glomerulonephritis secondary to monoclonal gammopathy
Abstract
Background and objectives: Membranoproliferative glomerulonephritis (MPGN) is an immune complex-mediated glomerulonephritis characterized by subendothelial and mesangial deposition of immune complexes. Autoimmune diseases and chronic infections, such as hepatitis C, are commonly recognized causes of MPGN; however, monoclonal gammopathy is a less widely recognized cause of MPGN.
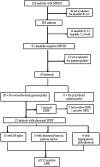
Design, setting, participants, & measurements: We reviewed all renal biopsies of MPGN in Mayo Clinic patients during a 6-year period to determine the association of monoclonal gammopathy with MPGN. Results were correlated with electrophoresis studies and bone marrow biopsies to clarify the relationship between MPGN and gammopathies.
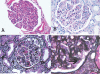
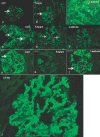
Results: Of 126 patients with MPGN, 20 did not have workup for hepatitis B or C. Of the remaining 106 patients, 25 (23.5%) were positive for hepatitis B or C. Of the 81 hepatitis-negative patients, 13 were not evaluated for gammopathies. Of the remaining 68 patients, 28 (41.1%) had serum and/or urine electrophoresis studies positive for monoclonal gammopathy. Serum immunofixation electrophoresis was the most sensitive method for diagnosing monoclonal gammopathy. Renal biopsy showed a membranoproliferative pattern of injury; immunofluorescence microscopy was often instrumental in diagnosing the underlying gammopathy. On the basis of the bone marrow biopsy, monoclonal gammopathy of undetermined significance was the most common entity associated with MPGN. Other, less common causes included multiple myeloma, low-grade B cell lymphoma, and chronic lymphocytic leukemia.
Conclusions: Monoclonal gammopathy is an important and common cause of MPGN; therefore, all patients with a diagnosis of MPGN should be evaluated for an underlying monoclonal gammopathy.
Figures


References
-
- Smith KD, Alpers CE: Pathogenic mechanisms in membranoproliferative glomerulonephritis. Curr Opin Nephrol Hypertens 14: 396– 403, 2005 - PubMed
-
- Rennke H: Secondary membranoproliferative glomerulonephritis. Kidney Int 47: 643– 656, 1995 - PubMed
-
- Hewins PS, Smith RJH, Savage CO. Idiopathic membranoproliferative glomerulonephritis. In: Therapy in Nephrology and Hypertension, 3rd Ed., edited by Wilcox CS, Berl T, Himmelfarb J, Mitch WE, Murphy B, Salant DJ, Yu ASL.Philadelphia, Saunders/Elsevier, 2008, pp 249– 256
-
- Smith RJ, Alexander J, Barlow PN, Botto M, Cassavant TL, Cook HT, de Cordoba SR, Hageman GS, Jokiranta TS, Kimberling WJ, Lambris JD, Lanning LD, Levidiotis V, Licht C, Lutz HU, Meri S, Pickering MC, Quigg RJ, Rops AL, Salant DJ, Sethi S, Thurman JM, Tully HF, Tully SP, van der Vlag J, Walker PD, Wurzner R, Zipfel PF, Dense Deposit Disease Focus Group: New approaches to the treatment of dense deposit disease. J Am Soc Nephrol 18: 2447– 2456, 2007 - PMC - PubMed
-
- Yamabe H, Johnson RJ, Gretch DR, Fukushi K, Osawa H, Miyata M, Inuma H, Sasaki T, Kaizuka M, Tamura N: Hepatitis C virus infection and membranoproliferative glomerulonephritis in Japan. J Am Soc Nephrol 6: 220– 223, 1995 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

