Revision hip arthroplasty: infection is the most common cause of failure
- PMID: 20195808
- PMCID: PMC2895846
- DOI: 10.1007/s11999-010-1251-6
Revision hip arthroplasty: infection is the most common cause of failure
Abstract
Background: Revision total hip arthroplasty (THA), although relieving pain and restoring function, fails in some patients. In contrast to failures in primary THA, the frequency of the causes of failure in revision THA has been less well established.
Questions/purposes: We therefore determined the rate of each failure mode and the survivorship of revision THAs.
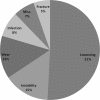
Methods: We retrospectively reviewed the charts of 1366 revision THAs performed between 2000 and 2007. There were 609 (44.5%) men and 757 (55.5%) women with a mean age of 66 years. The indications for the revision surgery were mainly aseptic loosening (51%), instability (15%), wear (14%), and infection (8%). The minimum followup was 1 day (mean, 5.5 years; range, 1 day to 9 years).
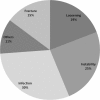
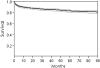
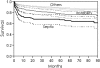
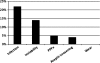
Results: Two hundred fifty-six of the revisions (18.7%) failed with an average time to failure of 16.6 months (range, 1 day to 7.5 years). Among 256 failed hips, infection was the most common cause of failure (30.2%) followed by instability (25.1%) and aseptic loosening (19.4%). At 5 years, the survivorships of septic and aseptic groups were 67% and 84.8%, respectively. Revision for infection or instability appears to have a considerably lower survivorship when compared to revision for aseptic causes.
Conclusions: The lower survivorship of revision for infection or instability highlights the importance of implementing better preventative methods that can minimize the impact of these two major causes of failure.
Level of evidence: Level III, therapeutic study. See the Guidelines for Authors for a complete description of levels of evidence.
Figures

References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

