Community-wide benefits of targeted indoor residual spray for malaria control in the western Kenya highland
- PMID: 20199674
- PMCID: PMC2843726
- DOI: 10.1186/1475-2875-9-67
Community-wide benefits of targeted indoor residual spray for malaria control in the western Kenya highland
Abstract
Background: Interest in indoor residual spray (IRS) has been rekindled in recent years, as it is increasingly considered to be a key component of integrated malaria management. Regular spraying of each human dwelling becomes less and less practical as the control area increases. Where malaria transmission is concentrated around focal points, however, targeted IRS may pose a feasible alternative to mass spraying. Here, the impact of targeted IRS was assessed in the highlands of western Kenya.
Methods: Indoor residual spray using lambda-cyhalothrin insecticide was carried out during the last week of April 2005 in 1,100 targeted houses, located in the valley bottom areas of Iguhu village, Kakamega district of western Kenya. Although the uphill areas are more densely populated, valleys are believed to be malaria transmission hotspots. The aim of the study was to measurably reduce the vector density and malaria transmission in uphill areas by focusing control on these hotspots. A cohort of 1,058 children from 1-5 yrs of age was randomly selected from a 4 km by 6 km study area for the baseline malaria prevalence survey after pre-clearing malaria infections during the third week of April 2005, and the prevalence of Plasmodium infections was tested bi-weekly. Seasonal changes in mosquito densities 12 months before the IRS and 12 months after the IRS was monitored quarterly based on 300 randomly selected houses. Monthly parasitological surveys were also carried out in the same area with 129-661 randomly selected school children of age 6-13 yrs.
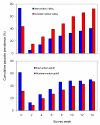
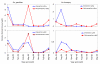
Results: The result of monthly parasitological surveys indicated that malaria prevalence in school children was reduced by 64.4% in the intervention valley area and by 46.3% in the intervention uphill area after 12 months of follow-ups in contrast to nonintervention areas (valley or uphill). The cohort study showed an average of 4.5% fewer new infections biweekly in the intervention valley compare to nonintervention valley and the relative reduction in incidence rate by week 14 was 65.4%. The relative reduction in incidence rate in intervention uphill by week 14 was 46.4%. Anopheles gambiae densities were reduced by 96.8% and 51.6% in the intervention valley and intervention uphill, respectively, and Anopheles funestus densities were reduced by 85.3% and 69.2% in the intervention valley and intervention uphill, respectively.
Conclusion: Vector control had significant indirect impact on the densely populated uphill areas when IRS was targeted to the high-risk valleys. Additionally, the wide-reaching benefits of IRS in reducing vector prevalence and disease incidence was observed for at least six months following spraying, suggesting targeted IRS as an effective tool in malaria control.
Figures


References
-
- Cox J, Craig M, le Sueur D, Sharp B. Mapping Malaria Risk in the Highlands of Africa. MARA/HIMAL Technical Report, Durban, South Africa; 1999. p. 96.
-
- Lindblade KA, Eisele TP, Gimnig JE, Alaii JA, Odhiambo F, ter Kuile FO, Hawley WA, Wannemuehler KA, Phillips-Howard PA, Rosen DH, Nahlen BL, Terlouw DJ, Adazu K, Vulule JM, Slutsker L. Sustainability of reductions in malaria transmission and infant mortality in western Kenya with use of insecticide-treated bednets: 4 to 6 years of follow-up. JAMA. 2004;291:2571–2580. doi: 10.1001/jama.291.21.2571. - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

