Pharmacologic modulation of niche accessibility via tyrosine kinase inhibition enhances marrow and thymic engraftment after hematopoietic stem cell transplantation
- PMID: 20231424
- PMCID: PMC2875097
- DOI: 10.1182/blood-2009-10-248898
Pharmacologic modulation of niche accessibility via tyrosine kinase inhibition enhances marrow and thymic engraftment after hematopoietic stem cell transplantation
Abstract
Essential survival signals within hematopoietic stem cell (HSC) and thymic niches are mediated by receptor tyrosine kinases, which can be reversibly inhibited using clinically available drugs. We studied whether sunitinib, a multityrosine kinase inhibitor that inhibits KIT, enhances engraftment after bone marrow transplantation (BMT) in mice. Sunitinib diminished hematopoietic progenitor cell numbers, and sunitinib enhanced marrow, peripheral myeloid, and lymphoid engraftment after BMT in Rag1(-/-) mice. Sunitinib augmented HSC engraftment because recipients displayed increased myeloid and lymphoid engraftment and because sunitinib-treated recipients of purified HSCs showed enhanced engraftment of secondary hosts. However, sunitinib preferentially augmented T-cell engraftment with lesser effects on myeloid and HSC engraftment. Consistent with this, sunitinib preferentially depleted the early thymic progenitor subset in the thymus. Sunitinib did not increase engraftment in mice with deficient KIT signaling, and the pattern of more potent effects on T cell compared with HSC engraftment observed in sunitinib-treated hosts was also observed after BMT into KIT(W/Wv) mice. These results implicate KIT as a critical modulator of thymic niches. We conclude that transient, pharmacologic inhibition of KIT enhances accessibility of marrow and thymic niches, and provides a novel, noncytotoxic approach to accomplish engraftment after stem cell transplantation.
Figures


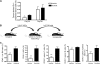


Similar articles
-
Kitlo hematopoietic stem cells exhibit distinct lymphoid-primed chromatin landscapes that enhance thymic reconstitution.Nat Commun. 2025 Jul 4;16(1):6170. doi: 10.1038/s41467-025-61125-1. Nat Commun. 2025. PMID: 40615375 Free PMC article.
-
Characterization of thymic progenitors in adult mouse bone marrow.J Immunol. 2003 Feb 15;170(4):1877-86. doi: 10.4049/jimmunol.170.4.1877. J Immunol. 2003. PMID: 12574354
-
FLT3 ligand regulates thymic precursor cells and hematopoietic stem cells through interactions with CXCR4 and the marrow niche.Exp Hematol. 2017 Aug;52:40-49. doi: 10.1016/j.exphem.2017.05.005. Epub 2017 May 26. Exp Hematol. 2017. PMID: 28552733 Free PMC article.
-
Thymic Engraftment by in vitro-Derived Progenitor T Cells in Young and Aged Mice.Front Immunol. 2020 Aug 18;11:1850. doi: 10.3389/fimmu.2020.01850. eCollection 2020. Front Immunol. 2020. PMID: 32973763 Free PMC article. Review.
-
Homing and Engraftment of Hematopoietic Stem Cells Following Transplantation: A Pre-Clinical Perspective.Curr Oncol. 2024 Jan 23;31(2):603-616. doi: 10.3390/curroncol31020044. Curr Oncol. 2024. PMID: 38392038 Free PMC article. Review.
Cited by
-
Thymus Size and Age-related Thymic Involution: Early Programming, Sexual Dimorphism, Progenitors and Stroma.Aging Dis. 2012 Jun;3(3):280-90. Epub 2012 Mar 14. Aging Dis. 2012. PMID: 22724086 Free PMC article.
-
Emerging strategies to boost thymic function.Curr Opin Pharmacol. 2010 Aug;10(4):443-53. doi: 10.1016/j.coph.2010.04.008. Epub 2010 May 4. Curr Opin Pharmacol. 2010. PMID: 20447867 Free PMC article. Review.
-
Non-genotoxic conditioning for hematopoietic stem cell transplantation using a hematopoietic-cell-specific internalizing immunotoxin.Nat Biotechnol. 2016 Jul;34(7):738-45. doi: 10.1038/nbt.3584. Epub 2016 Jun 6. Nat Biotechnol. 2016. PMID: 27272386 Free PMC article.
-
Modeling promising nonmyeloablative conditioning regimens in nonhuman primates.Hum Gene Ther. 2014 Dec;25(12):1013-22. doi: 10.1089/hum.2014.031. Hum Gene Ther. 2014. PMID: 24937231 Free PMC article.
-
Thymus: the next (re)generation.Immunol Rev. 2016 May;271(1):56-71. doi: 10.1111/imr.12418. Immunol Rev. 2016. PMID: 27088907 Free PMC article. Review.
References
-
- Urso P, Congdon CC. The effect of the amount of isologous bone marrow injected on the recovery of hematopoietic organs, survival and body weight after lethal irradiation injury in mice. Blood. 1957;12(3):251–260. - PubMed
-
- Copelan EA. Hematopoietic stem-cell transplantation. N Engl J Med. 2006;354(17):1813–1826. - PubMed
-
- Slavin S, Nagler A, Naparstek E, et al. Nonmyeloablative stem cell transplantation and cell therapy as an alternative to conventional bone marrow transplantation with lethal cytoreduction for the treatment of malignant and nonmalignant hematologic diseases. Blood. 1998;91(3):756–763. - PubMed
-
- Bhandoola A, Sambandam A, Allman D, Meraz A, Schwarz B. Early T lineage progenitors: new insights, but old questions remain. J Immunol. 2003;171(11):5653–5658. - PubMed
-
- Wang Z, Bunting KD. Hematopoietic stem cell transplant into non-myeloablated W/Wv mice to detect steady-state engraftment defects. Methods Mol Biol. 2008;430:171–181. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases

