Do the potential benefits of metal-on-metal hip resurfacing justify the increased cost and risk of complications?
- PMID: 20232182
- PMCID: PMC2914258
- DOI: 10.1007/s11999-010-1301-0
Do the potential benefits of metal-on-metal hip resurfacing justify the increased cost and risk of complications?
Abstract
Background: Metal-on-metal hip resurfacing arthroplasty (MoM HRA) may offer potential advantages over total hip arthroplasty (THA) for certain patients with advanced osteoarthritis of the hip. However, the cost effectiveness of MoM HRA compared with THA is unclear.
Questions/purposes: The purpose of this study was to compare the clinical effectiveness and cost-effectiveness of MoM HRA to THA.
Methods: A Markov decision model was constructed to compare the quality-adjusted life-years (QALYs) and costs associated with HRA versus THA from the healthcare system perspective over a 30-year time horizon. We performed sensitivity analyses to evaluate the impact of patient characteristics, clinical outcome probabilities, quality of life and costs on the discounted incremental costs, incremental clinical effectiveness, and the incremental cost-effectiveness ratio (ICER) of HRA compared to THA.
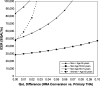
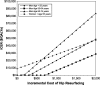
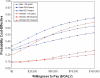
Results: MoM HRA was associated with modest improvements in QALYs at a small incremental cost, and had an ICER less than $50,000 per QALY gained for men younger than 65 and for women younger than 55. MoM HRA and THA failure rates, device costs, and the difference in quality of life after conversion from HRA to THA compared to primary THA had the largest impact on costs and quality of life.
Conclusions: MoM HRA could be clinically advantageous and cost-effective in younger men and women. Further research on the comparative effectiveness of MoM HRA versus THA should include assessments of the quality of life and resource use in addition to the clinical outcomes associated with both procedures.
Level of evidence: Level I, economic and decision analysis. See Guidelines for Authors for a complete description of levels of evidence.
Figures



References
-
- Agency for Healthcare Research and Quality. HCUPnet, Healthcare Cost and Utilization Project. Available at: http://hcupnet.ahrq.gov/. Accessed July 1, 2009.
-
- Amstutz HC, Beaule PE, Dorey FJ, Le Duff MJ, Campbell PA, Gruen TA. Metal-on-metal hybrid surface arthroplasty: two to six-year follow-up study. J Bone Joint Surg Am. 2004;86:28–39. - PubMed
-
- Arias E. United States life tables, 2004. National vital statistics reports; vol 56 no 9. Hyattsville, MD: National Center for Health Statistics, 2007. - PubMed
-
- Australian Orthopaedic Association National Joint Replacement Registry. Annual Report. 2008. Available at: http://www.surfacehippy.info/aoanationalreg08.php. Accessed April 1, 2009.

