Do radiation-associated soft tissue sarcomas have the same prognosis as sporadic soft tissue sarcomas?
- PMID: 20308666
- PMCID: PMC3651600
- DOI: 10.1200/JCO.2009.25.1728
Do radiation-associated soft tissue sarcomas have the same prognosis as sporadic soft tissue sarcomas?
Abstract
PURPOSE To determine the prognostic significance of histologic type in radiation-associated soft tissue sarcomas (RASs) and determine whether RASs are associated with an inferior prognosis compared with sporadic soft tissue sarcomas (STSs). PATIENTS AND METHODS One hundred thirty primary RASs were identified from 7,649 STS patients from 1982 to 2007. Multivariate analysis of clinicopathologic factors for disease-specific survival (DSS) was performed for RASs, and a multivariate analysis of radiation exposure was also performed for RASs and sporadic sarcomas. A matched-cohort analysis was performed for radiation-associated and sporadic malignant fibrous histiocytoma (MFH). Results Most RASs were high grade (83%), deep (87%), and truncal (61.5%). The median interval between radiation therapy and RAS development was 10 years (range, 1.3 to 74 years), which varied significantly by histologic type (P = .003). The 5-year DSS was 58%, and independent predictors were size > 5 cm, margin positivity, and histologic type. Multivariate analysis of histologic types of primary, high-grade radiation-associated and sporadic STSs showed that RAS was associated with a worse DSS (hazard ratio, 1.7; range, 1.1 to 2.4; P = .007). For pleomorphic MFH-the most common RAS type-the 5-year DSS was 44% versus 66% in a matched cohort of sporadic MFH patients (P = .07). DSS was significantly worse in primary RAS malignant peripheral nerve sheath tumors (MPNSTs) compared with unmatched sporadic MPNSTs (P = .001). CONCLUSION Histologic type, margin status, and tumor size are the most important independent predictors of DSS in patients with RASs. DSS in patients with primary RAS is significantly worse compared with sporadic STS independent of sarcoma histologic type.
Conflict of interest statement
Authors' disclosures of potential conflicts of interest and author contributions are found at the end of this article.
Figures
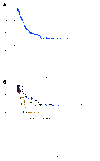
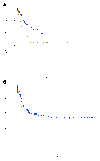
References
-
- Perez CA, Brady LW, editors. Principles and Practice of Radiation Oncology. ed 5. Philadelphia, PA: Lippincott Williams and Wilkins; 2004.
-
- Kirova YM, Gambotti L, De Rycke Y, et al. Risk of second malignancies after adjuvant radiotherapy for breast cancer: A large-scale, single-institution review. Int J Radiat Oncol Biol Phys. 2007;68:359–363. - PubMed
-
- Huang J, Mackillop WJ. Increased risk of soft tissue sarcoma after radiotherapy in women with breast carcinoma. Cancer. 2001;92:172–180. - PubMed
-
- Travis LB, Fossa SD, Schonfeld SJ, et al. Second cancers among 40,576 testicular cancer patients: Focus on long-term survivors. J Natl Cancer Inst. 2005;97:1354–1365. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

