The costs and cost-effectiveness of allogeneic peripheral blood stem cell transplantation versus bone marrow transplantation in pediatric patients with acute leukemia
- PMID: 20348004
- PMCID: PMC2919628
- DOI: 10.1016/j.bbmt.2010.03.016
The costs and cost-effectiveness of allogeneic peripheral blood stem cell transplantation versus bone marrow transplantation in pediatric patients with acute leukemia
Abstract
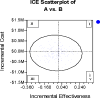
In a retrospective study, we evaluated the cost and cost-effectiveness of allogeneic peripheral blood stem cell transplantation (PBSCT) (n = 30) compared with bone marrow transplantation (BMT) (n = 110) in children with acute leukemia after 1 year of follow-up. Treatment success was defined as disease-free survival at 1 year posttransplantation. For patients at standard risk for disease, the treatment success rate was 57.1% for PBSCT recipients and 80.3% for BMT recipients (P = not significant [NS]). The average total cost per treatment success at 1 year in the standard-risk disease group was $512,294 for PBSCT recipients and $352,885 for BMT recipients (P = NS). For patients with high-risk disease, the treatment success rate was 18.8% for PBSCT recipients and 23.5% for BMT recipients (P = NS). The cumulative average cost was $457,078 in BMT recipients and $377,316 in PBSCT recipients (P = NS). Point estimates of the incremental cost-effectiveness ratio (ICER) indicate that in patients with standard-risk disease, allogeneic BMT had lower costs and greater effectiveness than PBSCT (ICER, -$687,108; 95% confidence interval [CI], $2.4 million to dominated). For patients with high-risk disease, BMT was more effective and more costly, and it had an ICER of $1.69 million (95% CI, $29.7 million to dominated) per additional treatment success. The comparative economic evaluation provides support for BMT in standard-risk patients, but much uncertainty precludes a clear advantage of either treatment option in patients with high-risk disease. More studies using larger and randomized controlled trials are needed to confirm the long-term cost-effectiveness of each procedure.
Copyright (c) 2010 American Society for Blood and Marrow Transplantation. Published by Elsevier Inc. All rights reserved.
Figures

Similar articles
-
Children with acute leukemia: a comparison of outcomes from allogeneic blood stem cell and bone marrow transplantation.Pediatr Blood Cancer. 2011 Jan;56(1):143-51. doi: 10.1002/pbc.22677. Pediatr Blood Cancer. 2011. PMID: 21108446
-
PBSCT is associated with poorer survival and increased chronic GvHD than BMT in Japanese paediatric patients with acute leukaemia and an HLA-matched sibling donor.Pediatr Blood Cancer. 2013 Sep;60(9):1513-9. doi: 10.1002/pbc.24524. Epub 2013 Mar 19. Pediatr Blood Cancer. 2013. PMID: 23512888
-
Transplantation of haematopoietic stem cells derived from cord blood, bone marrow or peripheral blood: a single centre matched-pair analysis in a heterogeneous risk population.Klin Padiatr. 2004 Nov-Dec;216(6):356-63. doi: 10.1055/s-2004-832357. Klin Padiatr. 2004. PMID: 15565551
-
Allogeneic Bone Marrow Transplantation versus Peripheral Blood Stem Cell Transplantation for Hematologic Malignancies in Children: A Systematic Review and Meta-Analysis.Biol Blood Marrow Transplant. 2020 Jan;26(1):88-93. doi: 10.1016/j.bbmt.2019.07.025. Epub 2019 Aug 5. Biol Blood Marrow Transplant. 2020. PMID: 31394270
-
Allogeneic peripheral blood stem cell and bone marrow transplantation for hematologic malignancies: meta-analysis of randomized controlled trials.Leuk Res. 2012 Apr;36(4):431-7. doi: 10.1016/j.leukres.2011.10.016. Epub 2011 Nov 1. Leuk Res. 2012. PMID: 22050904
Cited by
-
Costs and cost-effectiveness of hematopoietic cell transplantation.Biol Blood Marrow Transplant. 2012 Nov;18(11):1620-8. doi: 10.1016/j.bbmt.2012.04.001. Epub 2012 Apr 3. Biol Blood Marrow Transplant. 2012. PMID: 22484549 Free PMC article. Review.
-
Comparison of in-patient costs for children treated on the AAML0531 clinical trial: A report from the Children's Oncology Group.Pediatr Blood Cancer. 2015 Oct;62(10):1775-81. doi: 10.1002/pbc.25569. Epub 2015 May 6. Pediatr Blood Cancer. 2015. PMID: 25946708 Free PMC article. Clinical Trial.
-
Cost and cost-effectiveness of immunotherapy in childhood ALL: A systematic review.EJHaem. 2023 Nov 13;5(1):166-177. doi: 10.1002/jha2.814. eCollection 2024 Feb. EJHaem. 2023. PMID: 38406535 Free PMC article. Review.
-
Costs of hematopoietic stem cell transplantation in a developing country.Int J Hematol. 2017 Oct;106(4):573-580. doi: 10.1007/s12185-017-2278-1. Epub 2017 Jun 14. Int J Hematol. 2017. PMID: 28616698
-
Allogeneic Hematopoietic Cell Transplantation for Children with Sickle Cell Disease Is Beneficial and Cost-Effective: A Single-Center Analysis.Biol Blood Marrow Transplant. 2015 Jul;21(7):1258-65. doi: 10.1016/j.bbmt.2015.01.010. Epub 2015 Jan 20. Biol Blood Marrow Transplant. 2015. PMID: 25615608 Free PMC article.
References
-
- Schmitz N, Linch DC, Dreger P, et al. Randomised trial of filgrastim-mobilised peripheral blood progenitor cell transplantation versus autologous bone-marrow transplantation in lymphoma patients. Lancet. 1996;347:353–357. - PubMed
-
- To LB, Roberts MM, Haylock DN, et al. Comparison of heamatological recovery times and supportive care requirements of autologous recovery phase peripheral blood stem cell transplants, autologous bone marrow transplants and allogeneic bone marrow transplants. Bone Marrow Transplant. 1992;9:277–284. - PubMed
-
- Roberts MM, To LB, Gillis D, et al. Immune reconstitution following peripheral blood stem cell transplantation, autologous bone marrow transplantation and allogeneic bone marrow transplantation. Bone Marrow Transplant. 1993;12:469–475. - PubMed
-
- Nademanee A, Schmidt GM, Parker P, et al. The outcome of matched unrelated donor bone marrow transplantation in patients with hematologic malignancies using molecular typing for donor selection and graft-versus-host disease prophylaxis regimen of cyclosporine, methotrexate and prednisone. Blood. 1995;86:1228–1234. - PubMed
-
- Nash RA, Piñeiro LA, Storb R, et al. FK506 in combination with methotrexate for the prevention of graft-versus-host disease after marrow transplantation from matched unrelated donors. Blood. 1996;88:3634–3641. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

