Antibiotics for pre-term pre-labour rupture of membranes: prevention of neonatal deaths due to complications of pre-term birth and infection
- PMID: 20348116
- PMCID: PMC2845869
- DOI: 10.1093/ije/dyq030
Antibiotics for pre-term pre-labour rupture of membranes: prevention of neonatal deaths due to complications of pre-term birth and infection
Abstract
Background: In high-income countries, it is standard practice to give antibiotics to women with pre-term, pre-labour rupture of membranes (pPROM) to delay birth and reduce the risk of infection. In low and middle-income settings, where some 2 million neonatal deaths occur annually due to complications of pre-term birth or infection, many women do not receive antibiotic therapy for pPROM.
Objectives: To review the evidence for and estimate the effect on neonatal mortality due to pre-term birth complications or infection, of administration of antibiotics to women with pPROM, in low and middle-income countries.
Methods: We performed a systematic review to update a Cochrane review. Standardized abstraction forms were used. The quality of the evidence provided by individual studies and overall was assessed using an adapted GRADE approach.
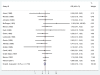
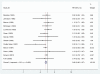
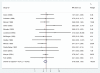
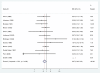
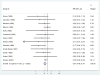
Results: Eighteen RCTs met our inclusion criteria. Most were from high-income countries and provide strong evidence that antibiotics for pPROM reduce the risk of respiratory distress syndrome [risk ratio (RR) = 0.88; confidence interval (CI) 0.80, 0.97], and early onset postnatal infection (RR = 0.61; CI 0.48, 0.77). The data are consistent with a reduction in neonatal mortality (RR = 0.90; CI 0.72, 1.12).
Conclusion: Antibiotics for pPROM reduce complications due to pre-term delivery and post-natal infection in high-income settings. There is moderate quality evidence that, in low-income settings, where access to other interventions (antenatal steroids, surfactant therapy, ventilation, antibiotic therapy) may be low, antibiotics for pPROM could prevent 4% of neonatal deaths due to complications of prematurity and 8% of those due to infection.
Figures
References
-
- Lawn JE, Cousens S, Zupan J. 4 million neonatal deaths: When? Where? Why? Lancet. 2005;365:891–900. - PubMed
-
- Mercer B, Arheart K. Antimicrobial therapy in expectant management of preterm premature rupture of the membranes. Lancet. 1995;346:1271–79. - PubMed
-
- Kenyon S, Boulvain M, Neilson JP. Antibiotics for preterm rupture of membranes. Cochr Database Syst Rev. 2003 doi: 10.1002/14651858.CD001058. - PubMed
-
- Lewis DF, Adair D, Robichaux AG, et al. Antibiotic therapy in preterm premature rupture of membranes: are seven days necessary? A preliminary, randomized clinical trial. Am J Obst Gynecol. 2003;188:1413–17. - PubMed
-
- Segel SY, Miles AM, Clothier B, et al. Duration of antibiotic therapy after preterm premature rupture of fetal membranes. Am J Obst Gynecol. 2003;189:799–802. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

