Development of a novel self-microemulsifying drug delivery system for reducing HIV protease inhibitor-induced intestinal epithelial barrier dysfunction
- PMID: 20349948
- PMCID: PMC2882528
- DOI: 10.1021/mp100003r
Development of a novel self-microemulsifying drug delivery system for reducing HIV protease inhibitor-induced intestinal epithelial barrier dysfunction
Abstract
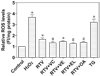
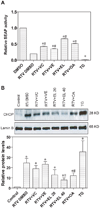
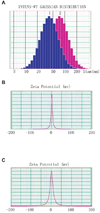
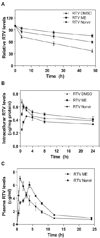
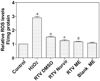
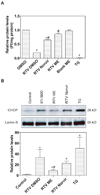
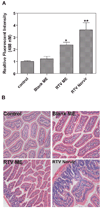
The development of HIV protease inhibitors (PIs) has been one of the most significant advances of the past decade in controlling HIV infection. Unfortunately, the benefits of HIV PIs are compromised by serious side effects. One of the most frequent and deleterious side effects of HIV PIs is severe gastrointestinal (GI) disorders including mucosal erosions, epithelial barrier dysfunction, and leak-flux diarrhea, which occurs in 16-62% of patients on HIV PIs. Although the underlying mechanisms behind HIV PI-associated serious adverse side effects remain to be identified, our recent studies have shown that activation of endoplasmic reticulum (ER) stress response plays a critical role in HIV PI-induced GI complications. The objective of this study was to develop a novel self-microemulsifying drug delivery system (SMEDDS) using various antioxidants as surfactants and cosurfactants to reduce the GI side effects of the most commonly used HIV PI, ritonavir. The biological activities of this SMSDDS of ritonavir were compared with that of Norvir, which is currently used in the clinic. Rat normal intestinal epithelial cells (IEC-6) and mouse Raw 264.7 macrophages were used to examine the effect of new SMEDDS of ritonavir on activation of ER stress and oxidative stress. Sprague-Dawley rats and C57/BL6 mice were used for pharmacokinetic studies and in vivo studies. The intracellular and plasma drug concentrations were determined by HPLC analysis. Activation of ER stress was detected by Western blot analysis and secreted alkaline phosphatase (SEAP) reporter assay. Reactive oxygen species (ROS) was measured using dichlorodihydrofluorescein diacetate as a probe. Cell viability was determined by Roche's cell proliferation reagent WST-1. Protein levels of inflammatory cytokines (TNF-alpha and IL-6) were determined by enzyme-linked immunosorbent assays (ELISA). The intestinal permeability was assessed by luminal enteral administration of fluorescein isothiocyanate conjugated dextran (FITC-dextran, 4 kDa). The pathologic changes in intestine were determined by histological examination. The results indicated that incorporation of antioxidants in this new SMEDDS not only significantly reduced ritonavir-induced ER stress activation, ROS production and apoptosis in intestinal epithelial cells and macrophages, but also improved the solubility, stability and bioavailability of ritonavir, and significantly reduced ritonavir-induced disruption of intestinal barrier function in vivo. In conclusion, this new SMEDDS of ritonavir has less GI side effects compared to Norvir. This new SMEDDS can be used for other HIV PIs and any insoluble antiviral drug with serious GI side effects.
Figures

Similar articles
-
HIV protease inhibitors induce endoplasmic reticulum stress and disrupt barrier integrity in intestinal epithelial cells.Gastroenterology. 2010 Jan;138(1):197-209. doi: 10.1053/j.gastro.2009.08.054. Epub 2009 Sep 2. Gastroenterology. 2010. PMID: 19732776 Free PMC article.
-
Solid self-microemulsifying drug delivery system of ritonavir.Drug Dev Ind Pharm. 2014 Apr;40(4):477-87. doi: 10.3109/03639045.2013.768632. Epub 2013 Mar 7. Drug Dev Ind Pharm. 2014. PMID: 23465049
-
Reduction of the HIV protease inhibitor-induced ER stress and inflammatory response by raltegravir in macrophages.PLoS One. 2014 Mar 13;9(3):e90856. doi: 10.1371/journal.pone.0090856. eCollection 2014. PLoS One. 2014. PMID: 24625618 Free PMC article.
-
Lopinavir/ritonavir: a review of its use in the management of HIV infection.Drugs. 2003;63(8):769-802. doi: 10.2165/00003495-200363080-00004. Drugs. 2003. PMID: 12662125 Review.
-
Combination of protease inhibitors for the treatment of HIV-1-infected patients: a review of pharmacokinetics and clinical experience.Antivir Ther. 2001 Dec;6(4):201-29. Antivir Ther. 2001. PMID: 11878403 Review.
Cited by
-
Inhibition of P-glycoprotein by HIV protease inhibitors increases intracellular accumulation of berberine in murine and human macrophages.PLoS One. 2013;8(1):e54349. doi: 10.1371/journal.pone.0054349. Epub 2013 Jan 23. PLoS One. 2013. PMID: 23372711 Free PMC article.
-
Click hybridization of immune cells and polyamidoamine dendrimers.Adv Healthc Mater. 2014 Sep;3(9):1430-8. doi: 10.1002/adhm.201300515. Epub 2014 Feb 13. Adv Healthc Mater. 2014. PMID: 24574321 Free PMC article.
References
-
- Clotet B, Negredo E. HIV protease inhibitors and dyslipidemia. AIDS Rev. 2003;5:19–24. - PubMed
-
- Spector AA. HIV protease inhibitors and hyperlipidemia: a fatty acid connection. Arterioscler.Thromb.Vasc.Biol. 2006;26:7–9. - PubMed
-
- Kudlow BA, Jameson SA, Kennedy BK. HIV protease inhibitors block adipocyte differentiation independently of lamin A/C. AIDS. 2005;19:1565–1573. - PubMed
-
- Lenhard JM, Furfine ES, Jain RG, Ittoop O, Orband-Miller LA, Blanchard SG, Paulik MA, Weiel JE. HIV protease inhibitors block adipogenesis and increase lipolysis in vitro. Antiviral Res. 2000;47:121–129. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

