Sleep state dependence of ventilatory long-term facilitation following acute intermittent hypoxia in Lewis rats
- PMID: 20360430
- PMCID: PMC2928603
- DOI: 10.1152/japplphysiol.90778.2008
Sleep state dependence of ventilatory long-term facilitation following acute intermittent hypoxia in Lewis rats
Abstract
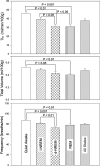
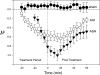
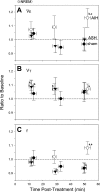
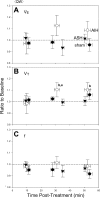
Ventilatory long-term facilitation (vLTF) is a form of respiratory plasticity induced by acute intermittent hypoxia (AIH). Although vLTF has been reported in unanesthetized animals, little is known concerning the effects of vigilance state on vLTF expression. We hypothesized that AIH-induced vLTF is preferentially expressed in sleeping vs. awake male Lewis rats. Vigilance state was assessed in unanesthetized rats with chronically implanted EEG and nuchal EMG electrodes, while tidal volume, frequency, minute ventilation (Ve), and CO(2) production were measured via plethysmography, before, during, and after AIH (five 5-min episodes of 10.5% O(2) separated by 5-min normoxic intervals), acute sustained hypoxia (25 min of 10.5% O(2)), or a sham protocol without hypoxia. Vigilance state was classified as quiet wakefulness (QW), light and deep non-rapid eye movement (NREM) sleep (l-NREM and d-NREM sleep, respectively), or rapid eye movement sleep. Ventilatory variables were normalized to pretreatment baseline values in the same vigilance state. During d-NREM sleep, vLTF was observed as a progressive increase in Ve post-AIH (27 + or - 5% average, 30-60 min post-AIH). In association, Ve/Vco(2) (36 + or - 2%), tidal volume (14 + or - 2%), and frequency (7 + or - 2%) were increased 30-60 min post-AIH during d-NREM sleep. vLTF was significant but less robust during l-NREM sleep, was minimal during QW, and was not observed following acute sustained hypoxia or sham protocols in any vigilance state. Thus, vLTF is state-dependent and pattern-sensitive in unanesthetized Lewis rats, with the greatest effects during d-NREM sleep. Although the physiological significance of vLTF is not clear, its greatest significance to ventilatory control is most likely during sleep.
Figures



References
-
- Aboubakr SE, Taylor A, Ford R, Siddiqi S, Badr MS. Long-term facilitation in obstructive sleep apnea patients during NREM sleep. J Appl Physiol 91: 2751–2757, 2001 - PubMed
-
- Babcock MA, Badr MS. Long-term facilitation of ventilation in humans during NREM sleep. Sleep 21: 709–716, 1998 - PubMed
-
- Babcock M, Shkoukani M, Aboubakr SE, Badr MS. Determinants of long-term facilitation in humans during NREM sleep. J Appl Physiol 94: 53–59, 2003 - PubMed
-
- Bach KB, Mitchell GS. Hypoxia-induced long-term facilitation of respiratory activity is serotonin dependent. Respir Physiol 104: 251–260, 1996 - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

