Delirium in the emergency department: an independent predictor of death within 6 months
- PMID: 20363527
- PMCID: PMC3768121
- DOI: 10.1016/j.annemergmed.2010.03.003
Delirium in the emergency department: an independent predictor of death within 6 months
Abstract
Study objective: Delirium's adverse effect on long-term mortality in older hospitalized patients is well documented, whereas its effect in older emergency department (ED) patients remains unclear. Similarly, the consequences of delirium on nursing home patients treated in the ED are also unknown. As a result, we seek to determine whether delirium in the ED is independently associated with 6-month mortality in older patients and whether this relationship is modified by nursing home status.
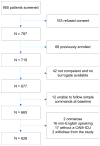
Methods: Our prospective cohort study was conducted at a tertiary care, academic ED, using convenience sampling, and included English-speaking patients who were aged 65 years and older and were in the ED for less than 12 hours at enrollment. Patients were excluded if they refused consent, were previously enrolled, were unable to follow simple commands at baseline, were comatose, or had incomplete data. The Confusion Assessment Method for the Intensive Care Unit was used to determine delirium and was administered by trained research assistants. Cox proportional hazard regression was performed to determine whether delirium in the ED was independently associated with 6-month mortality after adjusting for age, comorbidity burden, severity of illness, dementia, functional dependence, and nursing home residence. To test whether the effect of delirium in the ED on 6-month mortality was modified by nursing home residence, an interaction term (delirium*nursing home) was incorporated into the multivariable model. Hazard ratios with their 95% confidence intervals were reported.
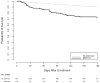
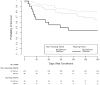
Results: Of the 628 patients enrolled, 108 (17.2%) were delirious in the ED and 58 (9.2%) were from the nursing home. For the entire cohort, the 6-month mortality rate was higher in the delirious group compared with the nondelirious group (37.0% versus 14.3%). Delirium was an independent predictor of increased 6-month mortality (hazard ratio=1.72; 95% confidence interval 1.04 to 2.86) after adjusting for age, comorbidity burden, severity of illness, dementia, functional dependence, and nursing home residence. The "delirium*nursing home" interaction was nonsignificant (P=.86), indicating that place of residence had no effect on the relationship between delirium in the ED and 6-month mortality.
Conclusion: Delirium in older ED patients is an independent predictor of increased 6-month mortality, and this relationship appears to be present regardless of nursing home status.
Copyright (c) 2009 American College of Emergency Physicians. Published by Mosby, Inc. All rights reserved.
Figures
References
-
- Hustey FM, Meldon SW, Smith MD, et al. The effect of mental status screening on the care of elderly emergency department patients. Ann Emerg Med. 2003;41:678–684. - PubMed
-
- American Psychiatric Association., American Psychiatric Association. Diagnostic and statistical manual of mental disorders: DSM-IV. 4. Washington, DC: American Psychiatric Association; 1994. Task Force on DSM-IV.
-
- McCaig LF, Burt CW. National Hospital Ambulatory Medical Care Survey: 2002 emergency department summary. Adv Data. 2004:1–34. - PubMed
-
- Braunwald E, Zipes D, Libby P, et al. Heart disease: a textbook of cardiovascular medicine. 7. Philadelphia: Elsevier Saunders; 2005.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

