Predictors of time to death after terminal withdrawal of mechanical ventilation in the ICU
- PMID: 20363840
- PMCID: PMC2913765
- DOI: 10.1378/chest.10-0289
Predictors of time to death after terminal withdrawal of mechanical ventilation in the ICU
Abstract
Background: Little information exists about the expected time to death after terminal withdrawal of mechanical ventilation. We sought to determine the independent predictors of time to death after withdrawal of mechanical ventilation.
Methods: We conducted a secondary analysis from a cluster randomized trial of an end-of-life care intervention. We studied 1,505 adult patients in 14 hospitals in Washington State who died within or shortly after discharge from an ICU following terminal withdrawal of mechanical ventilation (August 2003 to February 2008). Time to death and its predictors were abstracted from the patients' charts and death certificates. Predictors included demographics, proxies of severity of illness, life-sustaining therapies, and International Classification of Diseases, 9th ed., Clinical Modification codes.
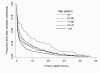
Results: The median (interquartile range [IQR]) age of the cohort was 71 years (58-80 years), and 44% were women. The median (IQR) time to death after withdrawal of ventilation was 0.93 hours (0.25-5.5 hours). Using Cox regression, the independent predictors of a shorter time to death were nonwhite race (hazard ratio [HR], 1.17; 95% CI, 1.01-1.35), number of organ failures (per-organ HR, 1.11; 95% CI, 1.04-1.19), vasopressors (HR, 1.67; 95% CI, 1.49-1.88), IV fluids (HR, 1.16; 95% CI, 1.01-1.32), and surgical vs medical service (HR, 1.29; 95% CI, 1.06-1.56). Predictors of longer time to death were older age (per-decade HR, 0.95; 95% CI, 0.90-0.99) and female sex (HR, 0.86; 95% CI, 0.77-0.97).
Conclusions: Time to death after withdrawal of mechanical ventilation varies widely, yet the majority of patients die within 24 hours. Subsequent validation of these predictors may help to inform family counseling at the end of life.
Figures

References
-
- Angus DC, Barnato AE, Linde-Zwirble WT, et al. Robert Wood Johnson Foundation ICU End-Of-Life Peer Group Use of intensive care at the end of life in the United States: an epidemiologic study. Crit Care Med. 2004;32(3):638–643. - PubMed
-
- Prendergast TJ, Claessens MT, Luce JM. A national survey of end-of-life care for critically ill patients. Am J Respir Crit Care Med. 1998;158(4):1163–1167. - PubMed
-
- Cook D, Rocker G, Marshall J, et al. Level of Care Study Investigators and the Canadian Critical Care Trials Group Withdrawal of mechanical ventilation in anticipation of death in the intensive care unit. N Engl J Med. 2003;349(12):1123–1132. - PubMed
-
- Stapleton RD, Wang BM, Hudson LD, Rubenfeld GD, Caldwell ES, Steinberg KP. Causes and timing of death in patients with ARDS. Chest. 2005;128(2):525–532. - PubMed
-
- Levy MM. End-of-life care in the intensive care unit: can we do better? Crit Care Med. 2001;29(2 suppl):N56–N61. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

