Hyperintense MRI lesions in bipolar disorder: A meta-analysis and review
- PMID: 20374153
- PMCID: PMC4098150
- DOI: 10.1080/09540260902962198
Hyperintense MRI lesions in bipolar disorder: A meta-analysis and review
Abstract
Background: Cortical and subcortical hyperintensities in magnetic resonance imaging (MRI) scans are thought to represent areas of ischemic damage to brain tissue. Researchers have focused on the possible role these lesions may have in psychiatric disorders, including bipolar disorder. In 1997, the proposed 'vascular mania' diagnosis suggested utilizing not only the presence of strokes, but also confluent hyperintensities in its diagnostic criteria. This study was conducted to use meta-analytic techniques to investigate the association of hyperintensities and bipolar illness and to evaluate the current state of the literature.
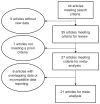
Methods: Using the PubMed and MEDLINE databases, we conducted a systematic literature search of studies investigating hyperintensities in subjects with bipolar disorder and controls or other psychiatric illnesses. We identified 44 publications from which 35 studies were included for review and 27 were selected for meta-analysis. Summary statistics of the prevalence were estimated through odds-ratios and confidence interval. Heterogeneity of the results across studies was tested using Q-statistics.
Results: Meta-analysis identified an odds ratio of 2.5 (95% CI 1.9, 3.3) for hyperintensities in bipolar subjects compared to controls; however, there was significant heterogeneity among the studies (Q-statistics = 32; p = 0.04). This finding was most prominent for adolescents and children where the odds ratio was 5.7 (95% CI 2.3, 13.7). Deep white matter hyperintensities (odd ratio 3.2; 95% CI 2.2, 4.5) and subcortical grey matter hyperintensities (odds ratio 2.7; 95% CI 1.3, 2.9) were more strongly associated with bipolar subjects. There were no differences between bipolar subjects and controls for perivascular hyperintensities (odds ratio 1.3; 95% CI 0.8, 1.9). Though hyperintensities were numerically greater in bipolar subjects, meta-analysis did not demonstrate any significant differences between bipolar subjects and unipolar depression subjects (OR 1.6; 95% CI 0.9, 2.7) nor subjects with schizophrenia (OR 1.5; 95% CI 0.9, 2.7).
Conclusions: This meta-analysis continues to support the association of bipolar disorder and hyperintensities, especially in the deep white matter and subcortical grey matter. It also highlights the increased incidence in children and adolescence with bipolar disorder. However, hyperintensities are not specific to bipolar disorder, but appear at similar rates in unipolar depression and schizophrenia. Thus, the role of hyperintensities in the pathogenesis, pathophysiology, and treatment of bipolar disorder remains unclear. Further studies are required that are large enough to decrease the heterogeneity of the samples and MRI techniques, assess size and location of hyperintensities, and the impact on treatment response. Coordination with newer imaging techniques, such as diffusion tensor imaging (DTI) may be especially helpful in understanding the pathology of these lesions.
Conflict of interest statement
Figures
References
-
- Ahearn EP, Speer MC, Chen YT, Steffens DC, Cassidy F, Van Meter S, et al. Investigation of Notch3 as a candidate gene for bipolar disorder using brain hyperintensities as an endophenotype. American Journal of Medical Genetics. 2002;114:652–658. - PubMed
-
- Ahearn EP, Steffens DC, Cassidy F, Van Meter SA, Provenzale JM, Seldin MF, et al. Familial leukoencephalopathy in bipolar disorder. American Journal of Psychiatry. 1998;155:1605–1607. - PubMed
-
- Ahn KH, Lyoo IK, Lee HK, Song IC, Oh JS, Hwang J, et al. White matter hyperintensities in subjects with bipolar disorder. Psychiatry and Clinical Neurosciences. 2004;58:516–521. - PubMed
-
- Alexopoulos GS, Meyers BS, Young RC, Campbell S, Silbersweig D, Charlson M. ‘Vascular depression’ hypothesis. Archives of General Psychiatry. 1997;54:915–922. - PubMed
-
- Altshuler LL, Curran JG, Hauser P, Mintz J, Denicoff K, Post R. T2 hyperintensities in bipolar disorder: magnetic resonance imaging comparison and literature meta-analysis. American Journal of Psychiatry. 1995;152:1139–1144. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical