Insulin inhibits human erythrocyte cAMP accumulation and ATP release: role of phosphodiesterase 3 and phosphoinositide 3-kinase
- PMID: 20404042
- PMCID: PMC2892266
- DOI: 10.1258/ebm.2009.009206
Insulin inhibits human erythrocyte cAMP accumulation and ATP release: role of phosphodiesterase 3 and phosphoinositide 3-kinase
Abstract
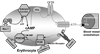
In non-erythroid cells, insulin stimulates a signal transduction pathway that results in the activation of phosphoinositide 3-kinase (PI3K) and subsequent phosphorylation of phosphodiesterase 3 (PDE3). Erythrocytes possess insulin receptors, PI3K and PDE3B. These cells release adenosine triphosphate (ATP) when exposed to reduced O(2) tension via a signaling pathway that requires activation of the G protein, Gi, as well as increases in cAMP. Although insulin inhibits ATP release from human erythrocytes in response to Gi activation by mastoparan 7 (Mas 7), no effect on cAMP was described. Here, we investigated the hypothesis that insulin activates PDE3 in human erythrocytes via a PI3K-mediated mechanism resulting in cAMP hydrolysis and inhibition of ATP release. Incubation of human erythrocytes with Mas 7 resulted in a 62 +/- 7% increase in cAMP (n = 9, P < 0.05) and a 306 +/- 69% increase in ATP release (n = 9, P < 0.05), both of which were attenuated by pre-treatment with insulin. Selective inhibitors of PDE3 (cilostazol) or PI3K (LY294002) rescued these effects of insulin. These results support the hypothesis that insulin activates PDE3 in erythrocytes via a PI3K-dependent mechanism. Once activated, PDE3 limits Mas 7-induced increases in intracellular cAMP. This effect of insulin leads, ultimately, to decreased ATP release in response to Mas 7. Activation of Gi is required for reduced O(2) tension-induced ATP release from erythrocytes and this ATP release has been shown to participate in the matching of O(2) supply with demand in skeletal muscle. Thus, pathological increases in circulating insulin could, via activation of PDE3 in erythrocytes, inhibit ATP release from these cells, depriving the peripheral circulation of one mechanism that could aid in the regulation of the delivery of O(2) to meet tissue metabolic need.
Figures




References
-
- Tooke JE. Microvascular function in human diabetes. A physiological perspective. Diabetes. 1995;44:721–726. - PubMed
-
- Wiernsperger N. Defects in microvascular haemodynamics during prediabetes: contributor or epiphenomenon? Diabetologia. 2000;43:1439–1448. - PubMed
-
- Shrot P, Sahebzamani FM, Brownlee HJ., Jr Case Study: Screening and Treatment of Pre-Diabetes in Primary Care. Clinical Diabetes. 2004;22:98–100.
-
- Benjamin SM, Valdez R, Geiss LS, Rolka DB, Narayan KM. Estimated number of adults with prediabetes in the US in 2000: opportunities for prevention. Diabetes Care. 2003;26:645–649. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

