T-cell responses induced by allergen-specific immunotherapy
- PMID: 20408857
- PMCID: PMC2940143
- DOI: 10.1111/j.1365-2249.2010.04148.x
T-cell responses induced by allergen-specific immunotherapy
Abstract
Allergen-specific immunotherapy is recognized as a highly effective practice in the treatment of patients with severe allergic rhinitis and/or asthma and is recommended by World Health Organization as an integrated part of allergy management strategy. Several studies have shown that allergen-specific immunotherapy, based on the administration of increasing doses of allergen, achieves a hyposensitization and reduces both early and late responses occurring during the natural exposure to the allergen itself. This is the unique antigen-specific immunomodulatory treatment in current use for human diseases. Successful immunotherapy is associated with reductions in symptoms and medication scores and improved quality of life. After interruption it usually confers long-term remission of symptoms and prevents the onset of new sensitizations in children up to a number of years. Subcutaneous immunotherapy usually suppresses the allergen-induced late response in target organs, likely due to the reduction of the infiltration of T cells, eosinophils, basophils, mast cells and neutrophils. In addition to the reduction of cells of allergic inflammation, immunotherapy also decreases inflammatory mediators at the site of allergen exposure. This review provides an update on the immunological T cell responses induced by conventional subcutaneous and sublingual immunotherapy, and gives a unifying view to reconciling the old dualism between immunoredirecting and immunoregulating mechanisms.
Figures
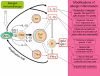
Similar articles
-
Methods for Experimental Allergen Immunotherapy: Subcutaneous and Sublingual Desensitization in Mouse Models of Allergic Asthma.Methods Mol Biol. 2021;2223:295-335. doi: 10.1007/978-1-0716-1001-5_20. Methods Mol Biol. 2021. PMID: 33226602
-
Immunologic responses to subcutaneous allergen immunotherapy.Clin Allergy Immunol. 2008;21:59-70. Clin Allergy Immunol. 2008. PMID: 18828498 Review. No abstract available.
-
Update on mechanisms of allergen injection immunotherapy.Clin Exp Allergy. 2008 Jul;38(7):1074-88. doi: 10.1111/j.1365-2222.2008.02976.x. Clin Exp Allergy. 2008. PMID: 18691292 Review.
-
T-cell responses during allergen-specific immunotherapy.Curr Opin Allergy Clin Immunol. 2012 Feb;12(1):1-6. doi: 10.1097/ACI.0b013e32834ecc9a. Curr Opin Allergy Clin Immunol. 2012. PMID: 22157159 Review.
-
Allergen immunotherapy, routes of administration and cytokine networks: an update.Immunotherapy. 2014;6(6):775-86. doi: 10.2217/imt.14.47. Immunotherapy. 2014. PMID: 25186606 Review.
Cited by
-
Differentiation stage determines pathologic and protective allergen-specific CD4+ T-cell outcomes during specific immunotherapy.J Allergy Clin Immunol. 2012 Feb;129(2):544-51, 551.e1-7. doi: 10.1016/j.jaci.2011.08.034. Epub 2011 Oct 5. J Allergy Clin Immunol. 2012. PMID: 21975176 Free PMC article. Clinical Trial.
-
The role of basophils as innate immune regulatory cells in allergy and immunotherapy.Hum Vaccin Immunother. 2018 Apr 3;14(4):815-831. doi: 10.1080/21645515.2017.1417711. Epub 2018 Jan 18. Hum Vaccin Immunother. 2018. PMID: 29257936 Free PMC article. Review.
-
Cutaneous vaccination with coated microneedles prevents development of airway allergy.J Control Release. 2017 Nov 10;265:75-82. doi: 10.1016/j.jconrel.2017.08.012. Epub 2017 Aug 15. J Control Release. 2017. PMID: 28821461 Free PMC article.
-
Toxoplasma gondii serine-protease inhibitor-1: A new adjuvant candidate for asthma therapy.PLoS One. 2017 Oct 26;12(10):e0187002. doi: 10.1371/journal.pone.0187002. eCollection 2017. PLoS One. 2017. PMID: 29073215 Free PMC article.
-
Elevated and cross-responsive CD1a-reactive T cells in bee and wasp venom allergic individuals.Eur J Immunol. 2016 Jan;46(1):242-52. doi: 10.1002/eji.201545869. Epub 2015 Nov 17. Eur J Immunol. 2016. PMID: 26518614 Free PMC article.
References
-
- Creticos PS. Immunotherapy with allergens. JAMA. 1992;268:2834–9. - PubMed
-
- Malling H-J, Weeke B. EAACI position paper: immunotherapy. Allergy. 1993;48:9–35. - PubMed
-
- Bousquet J, Lockey R, Malling HJ, et al. Allergen immunotherapy: therapeutic vaccines for allergic diseases. World Health Organization. American Academy of Allergy, Asthma and Immunology. Ann Allergy Asthma Immunol. 1998;81:401–5. - PubMed
-
- Durham SR, Walker SM, Varga EM, et al. Long-term clinical efficacy of grass-pollen immunotherapy. N Engl J Med. 1999;341:468–75. - PubMed
-
- Eng PA, Borer-Reinhold M, Heijnen IA, Gnehm HP. Twelve-year follow-up after discontinuation of preseasonal grass pollen immunotherapy in childhood. Allergy. 2006;61:198–201. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources

