Drug-induced thrombocytopenia for the hospitalist physician with a focus on heparin-induced thrombocytopenia
- PMID: 20469610
- PMCID: PMC3682781
Drug-induced thrombocytopenia for the hospitalist physician with a focus on heparin-induced thrombocytopenia
Abstract
Acute thrombocytopenia occurs commonly in hospitalized patients. For most, the etiology of an acutely declining platelet count is obvious and includes sepsis with disseminated intravascular coagulation, large-volume crystalloid infusion, or the administration of cytotoxic therapies, such as chemotherapeutic agents. For others, however, the etiology may be less apparent. In these cases, drug-induced thrombocytopenia (DIT), including heparin-induced thrombocytopenia (HIT), must be a diagnostic consideration. The approach to the hospitalized patient with thrombocytopenia, without an obvious cause, includes a careful medication history to identify potential culprits, such as glycoprotein IIb/IIIa inhibitors, vancomycin, linezolid, beta-lactam antibiotics, quinine, antiepileptic drugs, or heparin/low-molecular-weight heparin. Usually, discontinuation of the offending medication is all that is necessary for resolution of thrombocytopenia. Heparin-induced thrombocytopenia, however, is an exception to this general rule given its unique pathogenesis and propensity for thrombotic complications and death. Differentiating between HIT and DIT due to nonheparin medications may prove challenging. Through a careful clinical assessment, consideration of the pre-test probability for HIT, and the thoughtful application of laboratory testing, HIT can be accurately diagnosed. Because patients with HIT have a high risk of thrombosis and bleeding is uncommon, the prompt initiation of an alternative anticoagulant (e.g., a direct thrombin inhibitor) is warranted in these patients.
Conflict of interest statement
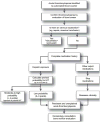
Figures

Similar articles
-
The management of heparin-induced thrombocytopenia.Br J Haematol. 2006 May;133(3):259-69. doi: 10.1111/j.1365-2141.2006.06018.x. Br J Haematol. 2006. PMID: 16643427
-
[Drug-induced thrombocytopenia].Nihon Rinsho. 2007 Oct 28;65 Suppl 8:465-9. Nihon Rinsho. 2007. PMID: 18074583 Review. Japanese. No abstract available.
-
Thrombocytopenia in cardiovascular patients: diagnosis and management.Chest. 2005 Feb;127(2 Suppl):46S-52S. doi: 10.1378/chest.127.2_suppl.46S. Chest. 2005. PMID: 15706030 Review.
-
[Heparin-induced thrombocytopenia (HIT): pathogenesis, laboratory test, and treatment].Rinsho Byori. 2005 Jul;53(7):622-9. Rinsho Byori. 2005. PMID: 16104531 Review. Japanese.
-
[Heparin-induced thrombocytopenia].Internist (Berl). 2010 Sep;51(9):1127-32, 1134-5. doi: 10.1007/s00108-010-2594-5. Internist (Berl). 2010. PMID: 20694716 Review. German.
Cited by
-
Vancomycin-induced thrombocytopenia in endocarditis: A case report and review of literature.World J Clin Cases. 2021 Mar 6;9(7):1696-1704. doi: 10.12998/wjcc.v9.i7.1696. World J Clin Cases. 2021. PMID: 33728314 Free PMC article.
-
Real-Life Evidence for Tedizolid Phosphate in the Treatment of Cellulitis and Wound Infections: A Case Series.Infect Dis Ther. 2018 Sep;7(3):387-399. doi: 10.1007/s40121-018-0207-0. Epub 2018 Jul 12. Infect Dis Ther. 2018. PMID: 30003513 Free PMC article.
-
Vancomycin-Induced Thrombocytopenia: A Narrative Review.Drug Saf. 2017 Jan;40(1):49-59. doi: 10.1007/s40264-016-0469-y. Drug Saf. 2017. PMID: 27848200 Review.
-
Life-Threatening Intrapulmonary Hemorrhage due to Vancomycin-Induced Thrombocytopenia: A Case Report.Case Rep Crit Care. 2020 Sep 30;2020:8890335. doi: 10.1155/2020/8890335. eCollection 2020. Case Rep Crit Care. 2020. PMID: 33062342 Free PMC article.
-
Heparin induced thrombocytopenia in pregnancy: A therapeutic challenge case report and literature review.Clin Case Rep. 2023 Aug 21;11(8):e7839. doi: 10.1002/ccr3.7839. eCollection 2023 Aug. Clin Case Rep. 2023. PMID: 37614288 Free PMC article.
References
-
- Oliveira GB, Crespo EM, Becker RC, et al. Complications After Thrombocytopenia Caused by Heparin (CATCH) Registry Investigators. Incidence and prognostic significance of thrombocytopenia in patients treated with prolonged heparin therapy. Arch Intern Med. 2008;168(1):94–102. - PubMed
-
- Wang TY, Ou FS, Roe MT, et al. Incidence and prognostic significance of thrombocytopenia developed during acute coronary syndrome in contemporary clinical practice. Circulation. 2009;119(18):2454–2462. - PubMed
-
- Hambleton J, Shuman MA. Hemorrhagic and thrombotic disorders in hospital medicine. In: Wachter RM, Goldman L, Hollander H, editors. Hospital Medicine. 2nd. Philadelphia, PA: Lippincott, Williams & Wilkins; 2005. pp. 592–600.
-
- George JN, Raskob GE, Shah SR, et al. Drug-induced thrombocytopenia: a systematic review of published case reports. Ann Intern Med. 1998;129(11):886–890. - PubMed
-
- Laber DA, Martin ME. Etiology of thrombocytopenia in all patients treated with heparin products. Eur J Haematol. 2005;75(2):101–105. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
