Rates of major depressive disorder and clinical outcomes following traumatic brain injury
- PMID: 20483970
- PMCID: PMC3090293
- DOI: 10.1001/jama.2010.599
Rates of major depressive disorder and clinical outcomes following traumatic brain injury
Abstract
Context: Uncertainties exist about the rates, predictors, and outcomes of major depressive disorder (MDD) among individuals with traumatic brain injury (TBI).
Objective: To describe MDD-related rates, predictors, outcomes, and treatment during the first year after TBI.
Design: Cohort from June 2001 through March 2005 followed up by structured telephone interviews at months 1 through 6, 8, 10, and 12 (data collection ending February 2006).
Setting: Harborview Medical Center, a level I trauma center in Seattle, Washington.
Participants: Five hundred fifty-nine consecutively hospitalized adults with complicated mild to severe TBI.
Main outcome measures: The Patient Health Questionnaire (PHQ) depression and anxiety modules were administered at each assessment and the European Quality of Life measure was given at 12 months.
Results: Two hundred ninety-seven of 559 patients (53.1%) met criteria for MDD at least once in the follow-up period. Point prevalences ranged between 31% at 1 month and 21% at 6 months. In a multivariate model, risk of MDD after TBI was associated with MDD at the time of injury (risk ratio [RR], 1.62; 95% confidence interval [CI], 1.37-1.91), history of MDD prior to injury (but not at the time of injury) (RR, 1.54; 95% CI, 1.31-1.82), age (RR, 0.61; 95% CI, 0.44-0.83 for > or = 60 years vs 18-29 years), and lifetime alcohol dependence (RR, 1.34; 95% CI, 1.14-1.57). Those with MDD were more likely to report comorbid anxiety disorders after TBI than those without MDD (60% vs 7%; RR, 8.77; 95% CI, 5.56-13.83). Only 44% of those with MDD received antidepressants or counseling. After adjusting for predictors of MDD, persons with MDD reported lower quality of life at 1 year compared with the nondepressed group.
Conclusions: Among a cohort of patients hospitalized for TBI, 53.1% met criteria for MDD during the first year after TBI. Major depressive disorder was associated with history of MDD and was an independent predictor of poorer health-related quality of life.
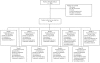
Figures


Comment in
-
Traumatic brain injury and major depressive disorder.JAMA. 2010 Aug 25;304(8):857; author reply 857-8. doi: 10.1001/jama.2010.1170. JAMA. 2010. PMID: 20736467 No abstract available.
References
-
- Langlois JA, Rutland-Brown W, Wald MM. The epidemiology and impact of traumatic brain injury: a brief overview. J Head Trauma Rehabil. 2006;21:375–378. - PubMed
-
- Hoge CW, McGurk D, Thomas JL, Cox AL, Engel CC, Castro CA. Mild traumatic brain injury in U.S. Soldiers returning from Iraq. N Engl J Med. 2008;358:453–463. - PubMed
-
- Consensus conference Rehabilitation of persons with traumatic brain injury. NIH Consensus Development Panel on Rehabilitation of Persons With Traumatic Brain Injury. JAMA. 1999;282:974–983. - PubMed
-
- Hibbard MR, Uysal S, Kepler K, Bogdany J, Silver J. Axis I psychopathology in individuals with traumatic brain injury. J Head Trauma Rehabil. 1998;13:24–39. - PubMed
-
- Chamelian L, Feinstein A. The effect of major depression on subjective and objective cognitive deficits in mild to moderate traumatic brain injury. J Neuropsychiatry Clin Neurosci. 2006;18:33–38. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

