Pericardial disease: diagnosis and management
- PMID: 20511488
- PMCID: PMC2878263
- DOI: 10.4065/mcp.2010.0046
Pericardial disease: diagnosis and management
Abstract
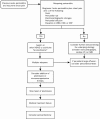
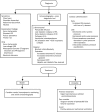
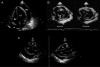
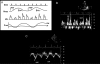
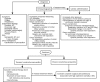
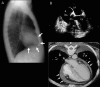
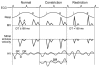
Pericardial diseases can present clinically as acute pericarditis, pericardial effusion, cardiac tamponade, and constrictive pericarditis. Patients can subsequently develop chronic or recurrent pericarditis. Structural abnormalities including congenitally absent pericardium and pericardial cysts are usually asymptomatic and are uncommon. Clinicians are often faced with several diagnostic and management questions relating to the various pericardial syndromes: What are the diagnostic criteria for the vast array of pericardial diseases? Which diagnostic tools should be used? Who requires hospitalization and who can be treated as an outpatient? Which medical management strategies have the best evidence base? When should corticosteroids be used? When should surgical pericardiectomy be considered? To identify relevant literature, we searched PubMed and MEDLINE using the keywords diagnosis, treatment, management, acute pericarditis, relapsing or recurrent pericarditis, pericardial effusion, cardiac tamponade, constrictive pericarditis, and restrictive cardiomyopathy. Studies were selected on the basis of clinical relevance and the impact on clinical practice. This review represents the currently available evidence and the experiences from the pericardial clinic at our institution to help guide the clinician in answering difficult diagnostic and management questions on pericardial diseases.
Figures
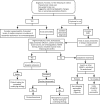

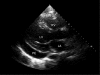
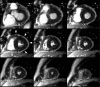
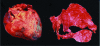



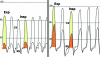
Comment in
-
Tailoring diagnosis and management of pericardial disease to the epidemiological setting.Mayo Clin Proc. 2010 Sep;85(9):866; author reply 866. doi: 10.4065/mcp.2010.0377. Mayo Clin Proc. 2010. PMID: 20810799 Free PMC article. No abstract available.
References
-
- Maisch B, Seferovic PM, Ristic AD, et al. Guidelines on the diagnosis and management of pericardial diseases executive summary: The task force on the diagnosis and management of pericardial diseases of the European Society of Cardiology. Eur Heart J. 2004;25(7):587-610 - PubMed
-
- Spodick DH. Acute cardiac tamponade. N Engl J Med. 2003;349(7):684-690 - PubMed
-
- Zayas R, Anguita M, Torres F, et al. Incidence of specific etiology and role of methods for specific etiologic diagnosis of primary acute pericarditis. Am J Cardiol. 1995;75(5):378-382 - PubMed
-
- Permanyer-Miralda G, Sagrista-Sauleda J, Soler-Soler J. Primary acute pericardial disease: a prospective series of 231 consecutive patients. Am J Cardiol. 1985;56(10):623-630 - PubMed
-
- Lange RA, Hillis LD. Clinical practice: acute pericarditis [published correction appears in N Engl J Med. 2005;352(11):1163] N Engl J Med. 2004;351(21):2195-2202 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

