Second-impact syndrome and a small subdural hematoma: an uncommon catastrophic result of repetitive head injury with a characteristic imaging appearance
- PMID: 20536318
- PMCID: PMC2956379
- DOI: 10.1089/neu.2010.1334
Second-impact syndrome and a small subdural hematoma: an uncommon catastrophic result of repetitive head injury with a characteristic imaging appearance
Abstract
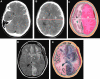
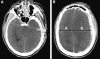
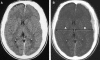
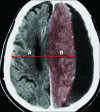
There have been a handful of previously published cases of athletes who were still symptomatic from a prior head injury, and then suffered a second injury in which a thin, acute subdural hematoma (SDH) with unilateral hemisphere vascular engorgement was demonstrated on CT scan. In those cases, the cause of the brain swelling/dysautoregulation was ascribed to the presence of the acute SDH rather than to the acceleration/deceleration forces that caused the SDH. We believe that the brain swelling is due to "second-impact dysautoregulation," rather than due to the effect of the SDH on the underlying hemisphere. To support our hypothesis, we present 10 additional cases of acute hemispheric swelling in association with small SDHs in athletes who received a second head injury while still symptomatic from a previous head injury. The clinical history and the unique neuroimaging features of this entity on CT are described and illustrated in detail. The CT findings included an engorged cerebral hemisphere with initial preservation of grey-white matter differentiation, and abnormal mass effect and midline shift that appeared disproportionately greater than the size of the SDH. In addition, the imaging similarities between our patients and those with non-accidental head trauma (shaken-baby syndrome) will be discussed.
Figures
References
-
- Boden B. Tacchetti R. Cantu R. Knowles S. Mueller F. Catastrophic head injuries in high school and college football players. Am J Sports Medicine. 2000;35:1–7. - PubMed
-
- Cantu R.C. Voy R. Second impact syndrome a risk in any contact sport. Phys. Sportsmed. 1995;23:27–34. - PubMed
-
- Cantu R.C. Neurological Athletic Head and Spine Injuries. WB Saunders; Philadelphia: 2000. p. 135.
-
- Cantu R.C. Second impact syndrome: Immediate management. Phys. Sportsmed. 1995;20:55–58. - PubMed
-
- Delaney J.S. Lacroix V.J. Leclerc S.L. Johnston K.M. Concussions among university football and soccer players. Clin. J. Sportsmed. 2002;12:331–338. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
