Immune responses to HIV and SIV in mucosal tissues: 'location, location, location'
- PMID: 20543589
- PMCID: PMC2886278
- DOI: 10.1097/COH.0b013e328335c178
Immune responses to HIV and SIV in mucosal tissues: 'location, location, location'
Abstract
Purpose of review: This review summarizes research literature regarding mucosal immunity to HIV and simian immunodeficiency virus (SIV), with an emphasis on work published within the past 18 months.
Recent findings: Notable recent studies have focused on the pivotal events occurring within mucosal tissues during acute HIV/SIV infection that serve to establish a balance between detrimental immune activation and beneficial adaptive responses. In cervicovaginal mucosa, an early inflammatory response leads to recruitment of susceptible target cells. At this acute stage, the in-vivo ratio between CD8 effector cells and infected CD4 T-cells may be critical for limiting viral dissemination. Acute infection is also accompanied by loss of germinal center architecture and T/B cell apoptosis in Peyer's patches of the gastrointestinal tract. During chronic infection, mucosal CD8 T-cells may play a role in immune control, as suggested by studies of elite controllers.
Summary: Mucosal tissues serve as the major portal of entry for HIV, and house a majority of the body's lymphocytes, including CD4 T-cells that are targets for infection. Recent studies have focused renewed attention on events occurring immediately after transmission, and underscore the concept that the balance between inflammation and protective immunity is established by host responses in mucosal tissues.
Figures
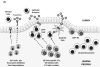

References
-
- Kotler DP. HIV infection and the gastrointestinal tract. AIDS. 2005;19:107–117. - PubMed
-
- Kotler DP, Gaetz HP, Lange M, et al. Enteropathy associated with the acquired immunodeficiency syndrome. Ann Intern Med. 1984;101:421–428. - PubMed
-
- Heise C, Miller CJ, Lackner A, et al. Primary acute simian immunodeficiency virus infection of intestinal lymphoid tissue is associated with gastrointestinal dysfunction. J Infect Dis. 1994;169:1116–1120. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

