Genotypic and phenotypic spectrum of pyridoxine-dependent epilepsy (ALDH7A1 deficiency)
- PMID: 20554659
- PMCID: PMC2892945
- DOI: 10.1093/brain/awq143
Genotypic and phenotypic spectrum of pyridoxine-dependent epilepsy (ALDH7A1 deficiency)
Abstract
Pyridoxine-dependent epilepsy was recently shown to be due to mutations in the ALDH7A1 gene, which encodes antiquitin, an enzyme that catalyses the nicotinamide adenine dinucleotide-dependent dehydrogenation of l-alpha-aminoadipic semialdehyde/L-Delta1-piperideine 6-carboxylate. However, whilst this is a highly treatable disorder, there is general uncertainty about when to consider this diagnosis and how to test for it. This study aimed to evaluate the use of measurement of urine L-alpha-aminoadipic semialdehyde/creatinine ratio and mutation analysis of ALDH7A1 (antiquitin) in investigation of patients with suspected or clinically proven pyridoxine-dependent epilepsy and to characterize further the phenotypic spectrum of antiquitin deficiency. Urinary L-alpha-aminoadipic semialdehyde concentration was determined by liquid chromatography tandem mass spectrometry. When this was above the normal range, DNA sequencing of the ALDH7A1 gene was performed. Clinicians were asked to complete questionnaires on clinical, biochemical, magnetic resonance imaging and electroencephalography features of patients. The clinical spectrum of antiquitin deficiency extended from ventriculomegaly detected on foetal ultrasound, through abnormal foetal movements and a multisystem neonatal disorder, to the onset of seizures and autistic features after the first year of life. Our relatively large series suggested that clinical diagnosis of pyridoxine dependent epilepsy can be challenging because: (i) there may be some response to antiepileptic drugs; (ii) in infants with multisystem pathology, the response to pyridoxine may not be instant and obvious; and (iii) structural brain abnormalities may co-exist and be considered sufficient cause of epilepsy, whereas the fits may be a consequence of antiquitin deficiency and are then responsive to pyridoxine. These findings support the use of biochemical and DNA tests for antiquitin deficiency and a clinical trial of pyridoxine in infants and children with epilepsy across a broad range of clinical scenarios.
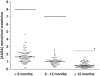
Figures

References
-
- Adam E, Goor M, Delattre B, Farriaux JP, Fontaine G. Les convulsions pyridoxino-dépendantes – a propos d’un noveau cas. Pédiatrie. 1972;27:19–25. - PubMed
-
- Basura GP, Hagland SP, Wiltse AM, Gospe SM., Jr Clinical features and the management of pyridoxine-dependent and pyridoxine-responsive seizures: review of 63 North American cases submitted to a patient registry. Eur J Pediatr. 2009;168:697–704. - PubMed
-
- Baxter P. Pyridoxine dependent/responsive seizures. In: Baxter P, editor. Vitamin responsive conditions in paediatric neurology. London: Mac Keith Press; 2001. pp. 109–165.
-
- Bennett CL, Chen Y, Hahn S, Glass IA, Gospe SM., Jr Prevalence of aldehyde dehydrogenase7A1 mutations in 18 North American pyridoxine-dependent seizure (PDS) patients. Epilepsia. 2009;50:1167–75. - PubMed
-
- Clayton PT. B6-responsive disorders: a model of vitamin dependency. J Inher Metab Dis. 2006a;29:317–26. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

