Trigeminal antihyperalgesic effect of intranasal carbon dioxide
- PMID: 20561904
- PMCID: PMC2900516
- DOI: 10.1016/j.lfs.2010.05.013
Trigeminal antihyperalgesic effect of intranasal carbon dioxide
Abstract
Aims: Clinical studies demonstrate attenuation of trigeminal-related pain states such as migraine by intranasal CO(2) application. This study investigated the underlying mechanisms of this observation and its potential use to reverse trigeminal pain and hypersensitivity.
Main methods: We used a behavioral rat model of capsaicin-induced trigeminal thermal hyperalgesia, intranasal CO2 application and several pharmacologic agents such as carbonic anhydrase, acid-sensing ion channels (ASICs), and TRPV1 blocker as well as acidic buffer solutions to investigate and mimic the underlying mechanism.
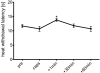
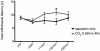
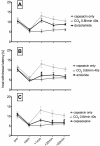
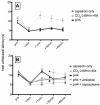
Key findings: Intranasal CO(2) application produced a robust dose-dependent antihyperalgesic effect in rats that lasted at least one hour. Blockade of nasal carbonic anhydrase with a dorzolamide solution (Trusopt ophthalmic solution) showed only a non-significant decrease of the antihyperalgesic effect of intranasal CO(2) application. Pharmacologic blockade of ASICs or TRPV(1) receptor significantly attenuated the antihyperalgesic effect of CO(2) application. The effect of intranasal CO(2) application could be mimicked by application of pH 4, but not pH 5, buffer solution to the nasal mucosa. As with CO(2) application, the antihyperalgesic effect of intranasal pH 4 buffer was blocked by nasal application of antagonists to ASICs and TRPV(1) receptors.
Significance: Our results indicate that intranasal CO(2) application results in a subsequent attenuation of trigeminal nociception, mediated by protonic activation of TRPV(1) and ASIC channels. A potential central mechanism for this attenuation is discussed. The antihyperalgesic effects of intranasal CO(2) application might be useful for the treatment of trigeminal pain states.
Copyright (c) 2010 Elsevier Inc. All rights reserved.
Figures

References
-
- Akaishi T, Odani-Kawabata N, Ishida N, Nakamura M. Ocular hypotensive effects of anti-glaucoma agents in mice. Journal of Ocular Pharmacology and Therapeutics. 2009;25(5):401–408. - PubMed
-
- Anton F, Peppel P, Euchner I, Handwerker HO. Controlled noxious chemical stimulation: responses of rat trigeminal brainstem neurons to CO2 pulses applied to the nasal mucosa. Neuroscience Letters. 1991;123(2):208–211. - PubMed
-
- Bigal M, Rapoport A, Aurora S, Sheftell F, Tepper S, Dahlof C. Satisfaction with current migraine therapy: experience from 3 centers in US and Sweden. Headache. 2007;47(4):475–479. - PubMed
-
- Bouhassira D, Chitour D, Villaneuva L, Le Bars D. The spinal transmission of nociceptive information: modulation by the caudal medulla. Neuroscience. 1995 Dec;69(3):931–8. - PubMed
-
- Cui JG, O’Connor WT, Ungerstedt U, Linderoth B, Meyerson BA. Spinal cord stimulation attenuates augmented dorsal horn release of excitatory amino acids in mononeuropathy via a GABAergic mechanism. Pain. 1997;73(1):87–95. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

