Evaluation of audiometric threshold shift criteria for ototoxicity monitoring
- PMID: 20569665
- PMCID: PMC5588921
- DOI: 10.3766/jaaa.21.5.3
Evaluation of audiometric threshold shift criteria for ototoxicity monitoring
Abstract
Background: There is disagreement about ototoxicity monitoring methods. Controversy exists about what audiometric threshold shift criteria should be used, which frequencies should be tested, and with what step size. An evaluation of the test performance achieved using various criteria and methods for ototoxicity monitoring may help resolve these issues.
Purpose: (1) Evaluate test performance achieved using various significant threshold shift (STS) definitions for ototoxicity monitoring in a predominately veteran population; and (2) determine whether testing in (1/6)- or (1/3)-octave steps improves test performance compared to (1/2)-octave steps.
Research design: A prospective, observational study design was used in which STSs were evaluated at frequencies within an octave of each subject's high-frequency hearing limit at two time points, an early monitoring test and the final monitoring test.
Study sample: Data were analyzed from 78 ears of 41 patients receiving cisplatin and from 53 ears of 28 hospitalized patients receiving nonototoxic antibiotics. Cisplatin-treated subjects received a cumulative dosage > or =350 mg by the final monitoring test. Testing schedule, age, and pre-exposure hearing characteristics were similar between the subject groups.
Data collection and analysis: Threshold shifts relative to baseline were examined to determine whether they met criteria based on magnitudes of positive STS (shifts of > or =5, 10, 15, or 20 dB) and numbers of frequencies affected (shifts at > or =1, 2, or 3 adjacent frequencies) for data collected using approximately (1/6)-, (1/3)-, or (1/2)-octave steps. Thresholds were confirmed during monitoring sessions in which shifts were identified. Test performance was evaluated with receiver operating characteristic (ROC) curves developed using a surrogate "gold standard"; true positive (TP) rates were derived from the cisplatin-exposed group and false positive (FP) rates from the nonexposed, control group. Best STS definitions were identified that achieved the greatest areas under ROC curves or resulted in the highest TP rates for a fixed FP rate near 5%, chosen to minimize the number of patients incorrectly diagnosed with ototoxic hearing loss.
Results: At the early monitoring test, average threshold shifts differed only slightly across groups. Test-frequency step size did not affect performance, and changes at one or more frequencies yielded the best test performance. At the final monitoring test, average threshold shifts were +10.5 dB for the cisplatin group, compared with -0.2 dB for the control group. Compared with the (1/2)-octave step size used clinically, use of smaller frequency steps improved test performance for threshold shifts at > or =2 or > or =3 adjacent frequencies. Best overall test performance was achieved using a criterion cutoff of > or =10 dB threshold shift at > or =2 adjacent frequencies tested in (1/6)-octave steps. Best test performance for the (1/2)-octave step size was achieved for shifts > or =15 dB at one or more frequencies.
Conclusions: An ototoxicity monitoring protocol that uses an individualized, one-octave range of frequencies tested in (1/6)-octave steps is quick to administer and has an acceptable FP rate. Similar test performance can be achieved using (1/3)-octave test frequencies, which further reduces monitoring test time.
American Academy of Audiology.
Figures
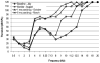




References
-
- American National Standards Institute (ANSI) American National Standard Specification for Audiometers (ANSI S3.6-1989) New York: American National Standards Institute; 1989.
-
- American Speech-Language-Hearing Association (ASHA) Guidelines for the audiologic management of individuals receiving cochleotoxic drug therapy. ASHA. 1994;36:11–19.
-
- Bertolini P, Lassalle M, Mercier G, et al. Platinum compound-related ototoxicity in children: long-term follow-up reveals continuous worsening of hearing loss. J Pediatr Hematol Oncol. 2004;26(10):649–655. - PubMed
-
- Blakley BW, Gupta AK, Myers SF, Schwan S. Risk factors for ototoxicity due to cisplatin. Arch Otolaryngol Head Neck Surg. 1994;120(5):541–546. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous
