Interventions for renal vasculitis in adults. A systematic review
- PMID: 20573267
- PMCID: PMC2914014
- DOI: 10.1186/1471-2369-11-12
Interventions for renal vasculitis in adults. A systematic review
Abstract
Background: Renal vasculitis presents as rapidly progressive glomerulonephritis and comprises of a group of conditions characterised by acute kidney failure, haematuria and proteinuria. Treatment of these conditions involves the use of steroid and non-steroid agents with or without adjunctive plasma exchange. Although immunosuppression has been successful, many questions remain unanswered in terms of dose and duration of therapy, the use of plasma exchange and the role of new therapies. This systematic review was conducted to determine the benefits and harms of any intervention for the treatment of renal vasculitis in adults.
Methods: We searched the Cochrane Central Register of Controlled Trials, the Cochrane Renal Group Specialised Register, MEDLINE and EMBASE to June 2009. Randomised controlled trials investigating any intervention for the treatment of adults were included. Two authors independently assessed study quality and extracted data. Statistical analyses were performed using a random effects model and results expressed as risk ratio with 95% confidence intervals for dichotomous outcomes or mean difference for continuous outcomes.
Results: Twenty two studies (1674 patients) were included. Plasma exchange as adjunctive therapy significantly reduces the risk of end-stage kidney disease at 12 months (five studies: RR 0.47, CI 0.30 to 0.75). Four studies compared the use of pulse and continuous administration of cyclophosphamide. Remission rates were equivalent but pulse treatment causes an increased risk of relapse (4 studies: RR 1.79, CI 1.11 to 2.87) compared with continuous cyclophosphamide. Azathioprine has equivalent efficacy as a maintenance agent to cyclophosphamide with fewer episodes of leukopenia. Mycophenolate mofetil may be equivalent to cyclophosphamide as an induction agent but resulted in a higher relapse rate when tested against Azathioprine in remission maintenance. Rituximab is an effective remission induction agent. Methotrexate or Leflunomide are potential choices in remission maintenance therapy. Oral co-trimoxazole did not reduce relapses significantly in Wegener's granulomatosis.
Conclusions: Plasma exchange is effective in patients with severe ARF secondary to vasculitis. Pulse cyclophosphamide results in an increased risk of relapse when compared to continuous oral use but a reduced total dose. Whilst cyclophosphamide is standard induction treatment, rituximab and mycophenolate mofetil are also effective. Azathioprine, methotrexate and leflunomide are effective as maintenance therapy. Further studies are required to more clearly delineate the appropriate place of newer agents within an evidence-based therapeutic strategy.
Figures







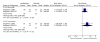
References
-
- Jennette J, Falk R. In: Comprehensive clinical nephrology. Mosby. 2. Johnson R, Feehally J, editor. 2003. Renal and systemic vasculitis; pp. 341–357.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

