The prevalence of fluoroquinolone resistance mechanisms in colonizing Escherichia coli isolates recovered from hospitalized patients
- PMID: 20597679
- PMCID: PMC2897836
- DOI: 10.1086/653931
The prevalence of fluoroquinolone resistance mechanisms in colonizing Escherichia coli isolates recovered from hospitalized patients
Abstract
Background: Fluoroquinolones are the most commonly prescribed antimicrobials. The epidemiology of fecal colonization with Escherichia coli demonstrating reduced susceptibility to fluoroquinolones remains unclear.
Methods: During a 3-year period (15 September 2004 through 19 October 2007), all patients hospitalized for >3 days were approached for fecal sampling. All E. coli isolates with reduced susceptibility to fluoroquinolones (minimum inhibitory concentration [MIC] of levofloxacin, 0.125 microg/mL) were identified. We characterized gyrA and parC mutations and organic solvent tolerance. Isolates were compared using pulsed-field gel electrophoresis.
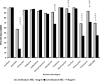
Results: Of 353 patients colonized with E. coli demonstrating reduced fluoroquinolone susceptibility, 300 (85.0%) had 1 gyrA mutation, 161 (45.6%) had 1 parC mutation, and 171 (48.6%) demonstrated organic solvent tolerance. The mean numbers of total mutations (ie, gyrA and parC) for E. coli isolates with a levofloxacin MIC of 8 microg/mL versus <8.0 microg/mL were 2.70 and 0.82 (P < .001). Of the 136 E. coli isolates with a levofloxacin MIC of 8 microg/mL, 90 (66.2%) demonstrated a nalidixic acid MIC of 16 microg/mL. Significant differences were found over time in the proportion of E. coli isolates demonstrating gyrA mutation, parC mutation, and organic solvent tolerance. There was little evidence of clonal spread of isolates. Conclusions. Gastrointestinal tract colonization with E. coli demonstrating reduced susceptibility to levofloxacin is common. Although 40% of study isolates exhibited a levofloxacin MIC of <8 microg/mL (and would thus be missed by current Clinical and Laboratory Standards Institute breakpoints), nalidixic acid resistance may be a useful marker for detection of such isolates. Significant temporal changes occurred in the proportion of isolates exhibiting various resistance mechanisms.
Figures
Comment in
-
Escherichia coli sequence type ST131 as the major cause of serious multidrug-resistant E. coli infections in the United States.Clin Infect Dis. 2010 Aug 1;51(3):286-94. doi: 10.1086/653932. Clin Infect Dis. 2010. PMID: 20572763
References
-
- Linder JA, Huang ES, Steinman MA, Gonzales R, Stafford RS. Fluoroquinolone prescribing in the United States: 1995 to 2002. Am J Med. 2005;118:259–68. - PubMed
-
- Hooper DC. New uses for new and old quinolones and the challenge of resistance. Clin Infect Dis. 2000;30:243–54. - PubMed
-
- Lautenbach E, Strom BL, Nachamkin I, et al. Longitudinal trends in fluoroquinolone resistance among Enterobacteriaceae isolates from inpatients and outpatients, (1989–2000): Differences in the emergence and epidemiology of resistance across organisms. Clin Infect Dis. 2004;38:655–62. - PubMed
-
- Neuhauser MM, Weinstein RA, Rydman R, Danziger LH, Karam G, Quinn JP. Antibiotic resistance among gram-negative bacilli in US intensive care units. JAMA. 2003;289:885–8. - PubMed
-
- Lautenbach E, Metlay JP, Bilker WB, Edelstein PH, Fishman NO. Association between fluoroquinolone resistance and mortality in Escherichia coli and Klebsiella pneumoniae infections: Role of inadequate empiric antimicrobial therapy. Clin Infect Dis. 2005;41:923–9. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical