Early menopause predicts angina after myocardial infarction
- PMID: 20651619
- PMCID: PMC3088434
- DOI: 10.1097/gme.0b013e3181e41f54
Early menopause predicts angina after myocardial infarction
Abstract
Objective: Population studies have shown that age at menopause (AAM) predicts coronary heart disease. It is unknown, however, whether early menopause predicts post-myocardial infarction (MI) angina. We examined whether younger AAM increases risk of post-MI angina.
Methods: In a prospective multicenter MI registry, 493 postmenopausal women were enrolled (mean +/- SD age, 65.4 +/- 11.3 y, and mean +/- SD AAM, 45.2 ± 7.8 y). We categorized AAM into 40 years or younger, 41 to 49 years, and 50 years or older. In the multivariable analysis, we examined whether AAM predicted 1-year post-MI angina and severity of angina after adjusting for angina before MI, demographics, comorbidities, MI severity, and quality of care (QOC).
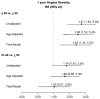
Results: Women with early AAM (> or =40 y; n = 132, 26.8%) were younger and more often smokers but were as likely to have comorbidities as were women with an AAM of 50 years or older. Although there were no differences in pre-MI angina, MI severity, obstructive coronary disease, and QOC based on AAM, the rate of 1-year angina was higher in women with an AAM of 40 years or younger (32.4%) than in women with an AAM of 50 years or older (12.2%). In the multivariable analysis, women with an AAM of 40 years or younger had more than twice the risk of angina (relative risk, 2.09; 95% CI, 1.38-3.17) and a higher severity of angina (odds ratio, 2.65; 95% CI, 1.34-5.22 for a higher severity level) compared with women with an AAM of 50 years or older.
Conclusions: Women with early menopause are at higher risk of angina after MI, independent of comorbidities, severity of MI, and QOC. The use of a simple question regarding AAM may help in the identification of women who need closer follow-up, careful evaluation, and intervention to improve their symptoms and quality of life after MI.
Conflict of interest statement
Financial disclosure/conflicts of interest: None reported.
Figures


Comment in
-
Cardiovascular epidemiology of postinfarction angina and menopause age.Menopause. 2010 Sep-Oct;17(5):896-7. doi: 10.1097/gme.0b013e3181ea1e66. Menopause. 2010. PMID: 20613674 No abstract available.
References
-
- Atsma F, Bartelink M, Grobbee DE, van der Schouw YT. Postmenopausal status and early menopause as independent risk factors for cardiovascular disease: a meta-analysis. Menopause. 2006;13:265–279. - PubMed
-
- Mendelsohn ME, Karas RH. The protective effect of estrogen on the cardiovascular system. N Engl J Med. 1999;340:1801–1811. - PubMed
-
- Shaw LJ, Merz CNB, Pepine CJ, et al. Insights from the NHLBI-sponsored Women’s Ischemia Syndrome Evaluation (WISE) study part I: gender differences in traditional and novel risk factors, symptom evaluation, and gender-optimized diagnostic strategies. J Am Coll Cardiol. 2006;47:4S–20S. - PubMed
-
- Gibbons RJ, Abrams J, Chatterjee K, et al. ACC/AHA 2002 guideline update for the management of patients with chronic stable angina—summary article—a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on the Management of Patients with Chronic Stable Angina) Circulation. 2003;107:149–158. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

