Simvastatin attenuates ventilator-induced lung injury in mice
- PMID: 20673352
- PMCID: PMC2945124
- DOI: 10.1186/cc9209
Simvastatin attenuates ventilator-induced lung injury in mice
Abstract
Introduction: Mechanical ventilation (MV) is a life saving intervention in acute respiratory failure without alternative. However, particularly in pre-injured lungs, even protective ventilation strategies may evoke ventilator-induced lung injury (VILI), which is characterized by pulmonary inflammation and vascular leakage. Adjuvant pharmacologic strategies in addition to lung protective ventilation to attenuate VILI are lacking. Simvastatin exhibited anti-inflammatory and endothelial barrier stabilizing properties in vitro and in vivo.
Methods: Mice were ventilated (12 ml/kg; six hours) and subjected to simvastatin (20 mg/kg) or sham treatment. Pulmonary microvascular leakage, oxygenation, pulmonary and systemic neutrophil and monocyte counts and cytokine release in lung and blood plasma were assessed. Further, lung tissue was analyzed by electron microscopy.
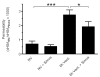
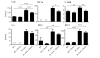
Results: Mechanical ventilation induced VILI, displayed by increased pulmonary microvascular leakage and endothelial injury, pulmonary recruitment of neutrophils and Gr-1high monocytes, and by liberation of inflammatory cytokines in the lungs. Further, VILI associated systemic inflammation characterized by blood leukocytosis and elevated plasma cytokines was observed. Simvastatin treatment limited pulmonary endothelial injury, attenuated pulmonary hyperpermeability, prevented the recruitment of leukocytes to the lung, reduced pulmonary cytokine levels and improved oxygenation in mechanically ventilated mice.
Conclusions: High-dose simvastatin attenuated VILI in mice by reducing MV-induced pulmonary inflammation and hyperpermeability.
Figures



Comment in
-
Protective role of statins against ventilator-induced lung injury.Crit Care. 2010;14(5):441. doi: 10.1186/cc9245. Epub 2010 Sep 16. Crit Care. 2010. PMID: 20860852 Free PMC article. No abstract available.
-
Statins STAT for (over)ventilated patients?Crit Care. 2010;14(6):1014. doi: 10.1186/cc9318. Epub 2010 Dec 20. Crit Care. 2010. PMID: 21211068 Free PMC article. Review.
Similar articles
-
Inhibition of HMGCoA reductase by simvastatin protects mice from injurious mechanical ventilation.Respir Res. 2015 Feb 14;16(1):24. doi: 10.1186/s12931-015-0173-y. Respir Res. 2015. PMID: 25848815 Free PMC article.
-
Adrenomedullin attenuates ventilator-induced lung injury in mice.Thorax. 2010 Dec;65(12):1077-84. doi: 10.1136/thx.2010.135996. Epub 2010 Oct 22. Thorax. 2010. PMID: 20971983
-
Simvastatin mitigates ventilator-induced lung injury in mice with acute respiratory distress syndrome via a mechanism partly dependent on neutrophil extracellular traps.Eur J Med Res. 2025 Apr 17;30(1):302. doi: 10.1186/s40001-025-02544-0. Eur J Med Res. 2025. PMID: 40247369 Free PMC article.
-
Statins STAT for (over)ventilated patients?Crit Care. 2010;14(6):1014. doi: 10.1186/cc9318. Epub 2010 Dec 20. Crit Care. 2010. PMID: 21211068 Free PMC article. Review.
-
Endothelial cell signaling and ventilator-induced lung injury: molecular mechanisms, genomic analyses, and therapeutic targets.Am J Physiol Lung Cell Mol Physiol. 2017 Apr 1;312(4):L452-L476. doi: 10.1152/ajplung.00231.2016. Epub 2016 Dec 15. Am J Physiol Lung Cell Mol Physiol. 2017. PMID: 27979857 Free PMC article. Review.
Cited by
-
Cyclooxygenase-2 Activity Regulates Recruitment of VEGF-Secreting Ly6Chigh Monocytes in Ventilator-Induced Lung Injury.Int J Mol Sci. 2019 Apr 10;20(7):1771. doi: 10.3390/ijms20071771. Int J Mol Sci. 2019. PMID: 30974834 Free PMC article.
-
Reference Gene Selection for Gene Expression Analyses in Mouse Models of Acute Lung Injury.Int J Mol Sci. 2021 Jul 22;22(15):7853. doi: 10.3390/ijms22157853. Int J Mol Sci. 2021. PMID: 34360619 Free PMC article.
-
Ventilator-induced lung injury is aggravated by antibiotic mediated microbiota depletion in mice.Crit Care. 2018 Oct 29;22(1):282. doi: 10.1186/s13054-018-2213-8. Crit Care. 2018. PMID: 30373626 Free PMC article.
-
Nanoparticle delivery of microRNA-146a regulates mechanotransduction in lung macrophages and mitigates injury during mechanical ventilation.Nat Commun. 2021 Jan 12;12(1):289. doi: 10.1038/s41467-020-20449-w. Nat Commun. 2021. PMID: 33436554 Free PMC article.
-
Targeting delivery of simvastatin using ICAM-1 antibody-conjugated nanostructured lipid carriers for acute lung injury therapy.Drug Deliv. 2017 Nov;24(1):402-413. doi: 10.1080/10717544.2016.1259369. Drug Deliv. 2017. PMID: 28165814 Free PMC article.
References
-
- Esteban A, Anzueto A, Frutos F, Alia I, Brochard L, Stewart TE, Benito S, Epstein SK, Apezteguia C, Nightingale P, Arroliga AC, Tobin MJ. Characteristics and outcomes in adult patients receiving mechanical ventilation: a 28-day international study. JAMA. 2002;287:345–355. doi: 10.1001/jama.287.3.345. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

