Prevalence and risk factors for hepatitis C virus infection among young Thai men
- PMID: 20682895
- PMCID: PMC2911198
- DOI: 10.4269/ajtmh.2010.09-0749
Prevalence and risk factors for hepatitis C virus infection among young Thai men
Abstract
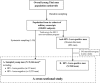
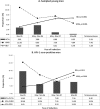
Epidemiologic studies of hepatitis C virus (HCV) infection are unusual in developing countries, especially Thailand. We evaluated the prevalence and risk factors for HCV among military conscripts, including a sample of 5,246 men (1:30 sample), and human immunodeficiency virus (HIV)-1 positive men (N = 500) between 2005 and 2008. The HCV prevalence was 2.2% in the sampled group and 8.4% in HIV-1 sero-positives. Among the sampled group, HIV-1 infection, injection drug use (IDU) history, and unsafe injections were associated with HCV infection; adjusted prevalence rate ratios [RRs; 95% confidence intervals (CIs)] were 3.7 (1.04-12.77), 1.9 (1.04-3.54), and 1.8 (1.02-3.11), respectively. Among HIV-1 sero-positives, an IDU history and residence in southern Thailand were associated with HCV prevalence; adjusted RRs (95% CIs) were 3.5 (1.71-7.24) and 2.6 (1.18-5.61), respectively. Public health measures to prevent HCV in Thailand should focus on reducing injection drug use and other exposures to unsafe injections among young Thai men.
Figures
Similar articles
-
Epidemiology of HIV-1 infection in opiate users in Northern Thailand.J Acquir Immune Defic Syndr Hum Retrovirol. 1998 Jan 1;17(1):73-8. doi: 10.1097/00042560-199801010-00011. J Acquir Immune Defic Syndr Hum Retrovirol. 1998. PMID: 9436762
-
The association between hepatitis C virus and HIV-1 in preparatory cohorts for HIV vaccine trials in Thailand.AIDS. 2003 Jun 13;17(9):1363-7. doi: 10.1097/00002030-200306130-00010. AIDS. 2003. PMID: 12799557
-
Hepatitis C infection among drug users in northern Thailand.Am J Trop Med Hyg. 2006 Jun;74(6):1111-6. Am J Trop Med Hyg. 2006. PMID: 16760529
-
The investigation of HIV and HCV infection and risk factors among opiate drug users in Beijing, China.Am J Drug Alcohol Abuse. 2012 Mar;38(2):140-5. doi: 10.3109/00952990.2011.643984. Epub 2011 Dec 19. Am J Drug Alcohol Abuse. 2012. PMID: 22175771
-
Prevalence of serologic markers of HBV, HDV, HCV and HIV in non-injection drug users compared to injection drug users in Gran Canaria, Spain.Eur J Epidemiol. 1998 Sep;14(6):555-61. doi: 10.1023/a:1007410707801. Eur J Epidemiol. 1998. PMID: 9794122
Cited by
-
Assessment of hepatitis C virus infection in two adjacent Thai provinces with drastically different seroprevalence.PLoS One. 2017 May 5;12(5):e0177022. doi: 10.1371/journal.pone.0177022. eCollection 2017. PLoS One. 2017. PMID: 28475637 Free PMC article.
-
Risk Factors for HIV Infection among Young Thai Men during 2005-2009.PLoS One. 2015 Aug 26;10(8):e0136555. doi: 10.1371/journal.pone.0136555. eCollection 2015. PLoS One. 2015. PMID: 26308085 Free PMC article.
-
Molecular Epidemiology of Hepatitis C Virus Genotypes in Northern Thailand: A Retrospective Study from 2016 to 2024.Infect Dis Rep. 2025 Jun 23;17(4):73. doi: 10.3390/idr17040073. Infect Dis Rep. 2025. PMID: 40700320 Free PMC article.
-
Challenges in Providing Treatment and Care for Viral Hepatitis among Individuals Co-Infected with HIV in Resource-Limited Settings.AIDS Res Treat. 2012;2012:948059. doi: 10.1155/2012/948059. Epub 2012 Mar 26. AIDS Res Treat. 2012. PMID: 22536498 Free PMC article.
-
Predictive factors for acquiring HCV infection in the population residing in high endemic, resource-limited settings.J Family Med Prim Care. 2021 Jan;10(1):167-174. doi: 10.4103/jfmpc.jfmpc_1835_20. Epub 2021 Jan 30. J Family Med Prim Care. 2021. PMID: 34017721 Free PMC article.
References
-
- Fattovich G, Stroffolini T, Zagni I, Donato F. Hepatocellular carcinoma in cirrhosis: incidence and risk factors. Gastroenterology. 2004;127:S35–S50. - PubMed
-
- Shepard CW, Finelli L, Alter MJ. Global epidemiology of hepatitis C virus infection. Lancet Infect Dis. 2005;5:558–567. - PubMed
-
- Centers for Disease Control and Prevention Recommendations for prevention and control of hepatitis C virus (HCV) infection and HCV-related chronic disease. MMWR Recomm Rep. 1998;47:1–39. - PubMed
-
- MacDonald M, Crofts N, Kaldor J. Transmission of hepatitis C virus: rates, routes, and cofactors. Epidemiol Rev. 1996;18:137–148. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

