Central venous oxygen saturation and blood lactate levels during cardiopulmonary bypass are associated with outcome after pediatric cardiac surgery
- PMID: 20684758
- PMCID: PMC2945132
- DOI: 10.1186/cc9217
Central venous oxygen saturation and blood lactate levels during cardiopulmonary bypass are associated with outcome after pediatric cardiac surgery
Abstract
Introduction: Central venous oxygen saturation and blood lactate are different indices of the adequacy of oxygen delivery to the oxygen needs. In pediatric cardiac surgery, lactate level and kinetics during and after cardiopulmonary bypass are associated with outcome variables. The aim of this study was to explore the hypothesis that the lowest central venous oxygen saturation and the peak lactate value during cardiopulmonary bypass, used alone or in combination, may be predictive of major morbidity and mortality in pediatric cardiac surgery.
Methods: We conducted a retrospective analysis of 256 pediatric (younger than 6 years) patients who had undergone cardiac surgery with continuous monitoring of central venous oxygen saturation and serial measurement of blood lactate.
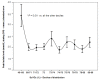
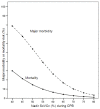
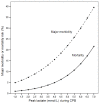
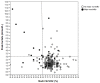
Results: Peak lactate was significantly increased when the nadir central venous oxygen saturation was < 68%. Both nadir central venous oxygen saturation and peak lactate during cardiopulmonary bypass were independently associated with major morbidity and mortality, with the same accuracy for major morbidity and a higher accuracy of peak lactate for mortality. A combined index (central venous oxygen saturation < 68% and peak lactate > 3 mmol/L) provided the highest sensitivity and specificity for major morbidity, with a positive predictive value of 89%.
Conclusions: The combination of a continuous monitoring of central venous oxygen saturation and serial measurements of blood lactate during cardiopulmonary bypass may offer a predictive index for major morbidity after cardiac operations in pediatric patients. This study generates the hypothesis that strategies aimed to preserve oxygen delivery during cardiopulmonary bypass may reduce the occurrence of low values of central venous oxygen saturation and elevated lactate levels. Further studies should consider this hypothesis and take into account other time-related factors, such as time of exposure to low values of central venous oxygen saturation and kinetics of lactate formation.
Figures


Similar articles
-
Central Venous to Arterial CO2 Difference After Cardiac Surgery in Infants and Neonates.Pediatr Crit Care Med. 2017 Mar;18(3):228-233. doi: 10.1097/PCC.0000000000001085. Pediatr Crit Care Med. 2017. PMID: 28121832 Free PMC article.
-
Regional differences in tissue oxygenation during cardiopulmonary bypass for correction of congenital heart disease in neonates and small infants: relevance of near-infrared spectroscopy.J Thorac Cardiovasc Surg. 2008 Oct;136(4):962-7. doi: 10.1016/j.jtcvs.2007.12.058. J Thorac Cardiovasc Surg. 2008. PMID: 18954637
-
Isolated high lactate or low central venous oxygen saturation after cardiac surgery and association with outcome.J Cardiothorac Vasc Anesth. 2013 Dec;27(6):1271-6. doi: 10.1053/j.jvca.2013.02.031. Epub 2013 Sep 5. J Cardiothorac Vasc Anesth. 2013. PMID: 24011873
-
A Review of Goal-Directed Cardiopulmonary Bypass Management in Pediatric Cardiac Surgery.World J Pediatr Congenit Heart Surg. 2018 Sep;9(5):565-572. doi: 10.1177/2150135118775964. World J Pediatr Congenit Heart Surg. 2018. PMID: 30157729 Review.
-
Objective assessment of cardiac output in infants after cardiac surgery.Semin Thorac Cardiovasc Surg Pediatr Card Surg Annu. 2011;14(1):19-23. doi: 10.1053/j.pcsu.2011.01.002. Semin Thorac Cardiovasc Surg Pediatr Card Surg Annu. 2011. PMID: 21444044 Review.
Cited by
-
Predictors of extubation in the operating room after pediatric cardiac surgery: A single-center retrospective study.Turk Gogus Kalp Damar Cerrahisi Derg. 2023 Oct 19;31(4):446-453. doi: 10.5606/tgkdc.dergisi.2023.24911. eCollection 2023 Oct. Turk Gogus Kalp Damar Cerrahisi Derg. 2023. PMID: 38076000 Free PMC article.
-
Year in review 2010: Critical Care--Cardiology.Crit Care. 2011;15(6):241. doi: 10.1186/cc10542. Epub 2011 Dec 5. Crit Care. 2011. PMID: 22152086 Free PMC article. Review.
-
Factors affecting on serum lactate after cardiac surgery.Anesth Pain Med. 2014 Oct 14;4(4):e18514. doi: 10.5812/aapm.18514. eCollection 2014 Oct. Anesth Pain Med. 2014. PMID: 25632379 Free PMC article.
-
Outcome effectiveness of the severe sepsis resuscitation bundle with addition of lactate clearance as a bundle item: a multi-national evaluation.Crit Care. 2011;15(5):R229. doi: 10.1186/cc10469. Epub 2011 Sep 27. Crit Care. 2011. PMID: 21951322 Free PMC article.
-
High central venous saturation after cardiac surgery is associated with increased organ failure and long-term mortality: an observational cross-sectional study.Crit Care. 2015 Apr 16;19(1):168. doi: 10.1186/s13054-015-0889-6. Crit Care. 2015. PMID: 25888321 Free PMC article.
References
-
- Tweddell JS, Hoffman GM, Mussatto KA, Fedderly RT, Berger S, Jaquiss RD, Ghanayem NS, Frisbee SJ, Litwin SB. Improved survival of patients undergoing palliation of hypoplastic left heart syndrome: lessons learned from 115 consecutive patients. Circulation. 2002;106:I82–I89. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

