Severe obesity is associated with symptomatic presentation, higher parathyroid hormone levels, and increased gland weight in primary hyperparathyroidism
- PMID: 20685860
- PMCID: PMC3205600
- DOI: 10.1210/jc.2010-0666
Severe obesity is associated with symptomatic presentation, higher parathyroid hormone levels, and increased gland weight in primary hyperparathyroidism
Abstract
Context: A relationship between primary hyperparathyroidism (PHPT) and obesity has been observed but is incompletely understood. Furthermore, obesity has been associated with vitamin D deficiency, suggesting that the three conditions may be linked.
Objective: We hypothesized that PHPT in morbidly obese patients is more severe and that the difference may be explained by vitamin D deficiency. DESIGN AND SETTING, PARTICIPANTS, AND OUTCOME MEASURES: Records of 196 patients with surgically treated PHPT and known body mass index (BMI) were examined. Patients were stratified into three BMI groups: group I (nonobese), BMI < 25 kg/m(2) (n = 54); group II (non-severely obese), BMI 25-34 kg/m(2) (n = 102); and group III (severely obese), BMI 35 kg/m(2) or greater (n = 40).
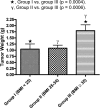
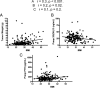
Results: Preoperative PTH levels were higher in group ΙΙΙ compared with group Ι (181 ± 153 vs. 140 ± 80 pg/ml, p = 0.04). Group III patients had larger tumors on average compared with group I (1.8 ± 1.5 vs. 1.04 ± 1.5 g, P = 0.0002). In group III, BMI positively correlated with parathyroid tumor weight (r = 0.5, P = 0.002). Postoperative PTH was higher in group III compared with group Ι (61 ± 41 vs. 44 ± 28 pg/ml, P = 0.02). There was higher frequency of depression, musculoskeletal symptoms, weakness, and gastroesophageal reflux disease in group III patients.
Conclusions: BMI positively correlated with parathyroid tumor weight independent of vitamin D. Severely obese patients have larger parathyroid tumor weight, higher pre- and postoperative PTH, and greater symptoms.
Figures
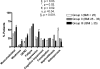

Similar articles
-
The effect of vitamin D status on the severity of bone disease and on the other features of primary hyperparathyroidism (pHPT) in a vitamin D deficient region.J Endocrinol Invest. 2004 Oct;27(9):807-12. doi: 10.1007/BF03346273. J Endocrinol Invest. 2004. PMID: 15648543
-
Association of Obesity on Rates of Multiglandular Disease in Primary Hyperparathyroidism: A Cohort Study.J Surg Res. 2025 Jan;305:349-355. doi: 10.1016/j.jss.2024.12.006. Epub 2024 Dec 28. J Surg Res. 2025. PMID: 39733472
-
Correlations between vitamin D status and biochemical/clinical and pathological parameters in primary hyperparathyroidism.World J Surg. 2006 Mar;30(3):321-6. doi: 10.1007/s00268-005-0239-y. World J Surg. 2006. PMID: 16467981
-
Primary hyperparathyroidism: incidence and clinical and biochemical characteristics. A demographic study.Eur J Surg. 1994 Sep;160(9):485-9. Eur J Surg. 1994. PMID: 7849167 Review.
-
Reappraisal of parathyroid pathology in hyperparathyroidism.Surg Clin North Am. 1974 Apr;54(2):443-7. doi: 10.1016/s0039-6109(16)40290-2. Surg Clin North Am. 1974. PMID: 4593913 Review. No abstract available.
Cited by
-
Bone Remodeling and Energy Metabolism: New Perspectives.Bone Res. 2013 Mar 29;1(1):72-84. doi: 10.4248/BR201301005. eCollection 2013 Mar. Bone Res. 2013. PMID: 26273493 Free PMC article. Review.
-
Association of body mass index and waist circumference with osteocalcin and C-terminal telopeptide in Iranian elderly: results from a cross-sectional study.J Bone Miner Metab. 2019 Jan;37(1):179-184. doi: 10.1007/s00774-018-0912-5. Epub 2018 Feb 23. J Bone Miner Metab. 2019. PMID: 29476244
-
Sex-Stratified Predictors of Prolonged Operative Time and Hospital Admission in Outpatient Parathyroidectomy.Indian J Otolaryngol Head Neck Surg. 2024 Apr;76(2):1910-1920. doi: 10.1007/s12070-023-04444-3. Epub 2024 Jan 8. Indian J Otolaryngol Head Neck Surg. 2024. PMID: 38566654 Free PMC article.
-
Epidemiology, Pathophysiology, and Genetics of Primary Hyperparathyroidism.J Bone Miner Res. 2022 Nov;37(11):2315-2329. doi: 10.1002/jbmr.4665. Epub 2022 Oct 17. J Bone Miner Res. 2022. PMID: 36245271 Free PMC article. Review.
-
Brown Adipose Tissue Biodistribution and Correlations Particularities in Parathyroid Pathology Personalized Diagnosis.Diagnostics (Basel). 2022 Dec 16;12(12):3182. doi: 10.3390/diagnostics12123182. Diagnostics (Basel). 2022. PMID: 36553189 Free PMC article.
References
-
- Ruda JM, Hollenbeak CS, Stack Jr BC 2005 A systematic review of the diagnosis and treatment of primary hyperparathyroidism from 1995 to 2003. Otolaryngol Head Neck Surg 132:359–372 - PubMed
-
- Bilezikian JP, Silverberg SJ 2000 Clinical spectrum of primary hyperparathyroidism. Rev Endocr Metab Disord 1:237–245 - PubMed
-
- Grey AB, Evans MC, Stapleton JP, Reid IR 1994 Body weight and bone mineral density in postmenopausal women with primary hyperparathyroidism. Ann Intern Med 121:745–749 - PubMed
-
- Bolland MJ, Grey AB, Gamble GD, Reid IR 2005 Association between primary hyperparathyroidism and increased body weight: a meta-analysis. J Clin Endocrinol Metab 90:1525–1530 - PubMed
-
- Russell J, Lettieri D, Sherwood LM 1986 Suppression by 1,25(OH)2D3 of transcription of the pre-proparathyroid hormone gene. Endocrinology 119:2864–2866 - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

