Clinicopathologic findings in failed descemet stripping automated endothelial keratoplasty
- PMID: 20696996
- PMCID: PMC3405987
- DOI: 10.1001/archophthalmol.2010.140
Clinicopathologic findings in failed descemet stripping automated endothelial keratoplasty
Abstract
Objective: To evaluate the clinical features of and histologic findings from failed Descemet stripping automated endothelial keratoplasty (DSAEK).
Methods: This retrospective observational case series evaluated 47 consecutive corneal specimens from 42 patients who underwent either penetrating keratoplasty or repeated DSAEK for failed DSAEK. Clinical information was obtained for the cases. Sections of the specimens were examined using light microscopy. Immunohistochemical staining was performed for cytokeratins AE1/AE3 and for the myogenic marker smooth-muscle actin when indicated. Transmission electron microscopic examination was performed in some cases.
Results: Graft survival ranged from 0.5 to 34 months. Histologic examination showed that 94% of the specimens (44 of 47) had endothelial cell loss. Residual host Descemet membrane (19%; 9 of 47), fibrocellular tissue (19%; 9 of 47), epithelial implantation (15%; 7 of 47), and fungal infection (4%; 2 of 47) were also identified. Immunohistochemical stains were positive for AE1/AE3 in the epithelial implantations and for smooth-muscle actin in cells in the fibrocellular proliferations.
Conclusions: The principal cause of failed DSAEK is endothelial cell loss. Residual host Descemet membrane, fibrocellular tissue at the edge of the lenticule, and epithelial implantation are common histologic findings. Fungal infection may occur in the setting of DSAEK.
Figures






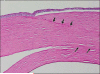
References
-
- Gorovoy MS. Descemet-stripping automated endothelial keratoplasty. Cornea. 2006;25(8):886–889. - PubMed
-
- Lee WB, Jacobs DS, Musch DC, Kaufman SC, Reinhart WJ, Shtein RM. Descemet's stripping endothelial keratoplasty: safety and outcomes: a report by the American Academy of Ophthalmology. Ophthalmology. 2009;116(9):1818–1830. - PubMed
-
- Suh LH, Yoo SH, Deobhakta A, et al. Complications of Descemet's stripping with automated endothelial keratoplasty: survey of 118 eyes at one institute. Ophthalmology. 2008;115(9):1517–1524. - PubMed
-
- Beach RA, Lawson D, Waldrop SM, Cohen C. Rapid immunohistochemistry for cytokeratin in the intraoperative evaluation of sentinel lymph nodes for meta-static breast carcinoma. Appl Immunohistochem Mol Morphol. 2003;11(1):45–50. - PubMed
-
- Williams KK, Noe RL, Grossniklaus HE, Drews-Botsch C, Edelhauser HF. Correlation of histologic corneal endothelial cell counts with specular microscopic cell density. Arch Ophthalmol. 1992;110(8):1146–1149. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

