Walking speed threshold for classifying walking independence in hospitalized older adults
- PMID: 20705685
- PMCID: PMC2967707
- DOI: 10.2522/ptj.20100018
Walking speed threshold for classifying walking independence in hospitalized older adults
Abstract
Background: Walking speed norms and several risk thresholds for poor health outcomes have been published for community-dwelling older adults. It is unclear whether these values apply to hospitalized older adults.
Objective: The purpose of this study was to determine the in-hospital walking speed threshold that best differentiates walking-independent from walking-dependent older adults.
Design: This was a cross-sectional study.
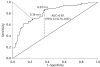
Methods: This study recruited a convenience sample of 174 ambulatory adults aged 65 years and older who had been admitted to a medical-surgical unit of a university hospital. The participants' mean (SD) age was 75 (7) years. Fifty-nine percent were women, 66% were white, and more than 40% were hospitalized for cardiovascular problems. Usual-pace walking speed was assessed over 2.4 m. Walking independence was assessed through self-report. Several methods were used to determine the threshold speed that best differentiated walking-independent patients from walking-dependent patients. Approaches included a receiver operating characteristic (ROC) curve, sensitivity and specificity, and frequency distributions.
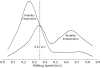
Results: The participants' mean (SD) walking speed was 0.43 (0.23) m/s, and 62% reported walking independence. Nearly 75% of the patients walked more slowly than the lowest community-based risk threshold, yet 90% were discharged home. Overall, cut-point analyses suggested that 0.30 to 0.35 m/s may be a meaningful threshold for maintaining in-hospital walking independence. For simplicity of clinical application, 0.35 m/s was chosen as the optimal cut point for the sample. This threshold yielded a balance between sensitivity and specificity (71% for both). Limitations The limitations of this study were the small size of the convenience sample and the single health outcome measure.
Conclusions: Walking speeds of older adults who are acutely ill are substantially slower than established community-based norms and risk thresholds. The threshold identified, which was approximately 50% lower than the lowest published community-based risk threshold, may serve as an initial risk threshold or target value for maintaining in-hospital walking independence.
Figures
Similar articles
-
Estimating cutpoints of gait speed and sit-to-stand test values for self-reported mobility limitations in a cohort of community-dwelling older adults from Singapore: comparing receiver operating characteristic (ROC) analysis with adjusted predictive modelling.Arch Gerontol Geriatr. 2023 Sep;112:105036. doi: 10.1016/j.archger.2023.105036. Epub 2023 Apr 14. Arch Gerontol Geriatr. 2023. PMID: 37075584
-
Gait Speed and Mobility Disability: Revisiting Meaningful Levels in Diverse Clinical Populations.J Am Geriatr Soc. 2018 May;66(5):954-961. doi: 10.1111/jgs.15331. Epub 2018 Apr 2. J Am Geriatr Soc. 2018. PMID: 29608795 Free PMC article.
-
The impact of testing protocol on recorded gait speed.Gait Posture. 2015 Jan;41(1):329-31. doi: 10.1016/j.gaitpost.2014.10.020. Epub 2014 Oct 28. Gait Posture. 2015. PMID: 25468684 Free PMC article.
-
Outdoor Walking Speeds of Apparently Healthy Adults: A Systematic Review and Meta-analysis.Sports Med. 2021 Jan;51(1):125-141. doi: 10.1007/s40279-020-01351-3. Sports Med. 2021. PMID: 33030707 Free PMC article.
-
A Scoping Review of the Predictive Qualities of Walking Speed in Older Adults.J Geriatr Phys Ther. 2024 Oct-Dec 01;47(4):183-191. doi: 10.1519/JPT.0000000000000398. Epub 2024 Sep 18. J Geriatr Phys Ther. 2024. PMID: 37820357
Cited by
-
Comparison of a Wearable Accelerometer/Gyroscopic, Portable Gait Analysis System (LEGSYS+TM) to the Laboratory Standard of Static Motion Capture Camera Analysis.Sensors (Basel). 2023 Jan 3;23(1):537. doi: 10.3390/s23010537. Sensors (Basel). 2023. PMID: 36617135 Free PMC article.
-
The Correlation between Cognition Screening Scores and Gait Status from Three-Dimensional Gait Analysis.J Clin Neurol. 2019 Apr;15(2):152-158. doi: 10.3988/jcn.2019.15.2.152. Epub 2019 Mar 11. J Clin Neurol. 2019. PMID: 30877689 Free PMC article.
-
Monitoring postures and motions of hospitalized patients using sensor technology: a scoping review.Ann Med. 2024 Dec;56(1):2399963. doi: 10.1080/07853890.2024.2399963. Epub 2024 Sep 6. Ann Med. 2024. PMID: 39239877 Free PMC article.
-
Influences of Spatial Accessibility and Service Capacity on the Utilization of Elderly-Care Facilities: A Case Study of the Main Urban Area of Chongqing.Int J Environ Res Public Health. 2023 Mar 8;20(6):4730. doi: 10.3390/ijerph20064730. Int J Environ Res Public Health. 2023. PMID: 36981639 Free PMC article.
-
Validation of the Activ8 Activity Monitor for Monitoring Postures, Motions, Transfers, and Steps of Hospitalized Patients.Sensors (Basel). 2023 Dec 28;24(1):180. doi: 10.3390/s24010180. Sensors (Basel). 2023. PMID: 38203041 Free PMC article.
References
-
- Berkman LF, Seeman TE, Albert M, et al. High, usual and impaired functioning in community-dwelling older men and women: findings from the MacArthur Foundation Research Network on Successful Aging. J Clin Epidemiol. 1993;46:1129–1140 - PubMed
-
- Cesari M, Kritchevsky SB, Penninx BW, et al. Prognostic value of usual gait speed in well-functioning older people: results from the Health, Aging and Body Composition Study. J Am Geriatr Soc. 2005;53:1675–1680 - PubMed
-
- Guralnik JM, Ferrucci L, Pieper CF, et al. Lower extremity function and subsequent disability: consistency across studies, predictive models, and value of gait speed alone compared with the short physical performance battery. J Gerontol A Biol Sci Med Sci. 2000;55:M221–M231 - PubMed
-
- Haworth JA. Gait, aging and dementia. Rev Clin Gerontol. 2008;18:39–52
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources

