The prostaglandin D₂ receptor CRTH2 is important for allergic skin inflammation after epicutaneous antigen challenge
- PMID: 20713302
- PMCID: PMC2950231
- DOI: 10.1016/j.jaci.2010.07.006
The prostaglandin D₂ receptor CRTH2 is important for allergic skin inflammation after epicutaneous antigen challenge
Abstract
Background: Cutaneous prostaglandin (PG) D₂ levels increase after scratching. Chemoattractant receptor-homologous molecule expressed on receptor on T(H)2 cells (CRTH2) mediates chemotaxis to PGD₂ and is expressed on T(H)2 cells and eosinophils, which infiltrate skin lesions in patients with atopic dermatitis.
Objective: We sought to examine the role of CRTH2 in a murine model of atopic dermatitis.
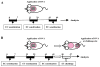
Methods: CRTH2(-/-) mice and wild-type control animals were epicutaneously sensitized by means of repeated application of ovalbumin (OVA) to tape-stripped skin for 7 weeks and then challenged by means of OVA application to tape-stripped previously unsensitized skin for 1 week. Skin histology was assessed by means of hematoxylin and eosin staining and immunohistochemistry. Cytokine mRNA expression was examined by means of quantitative RT-PCR. Levels of PGD₂, antibody, and cytokines were measured by means of ELISA.
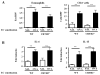
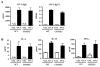
Results: PGD₂ levels significantly increased in skin 24 hours after tape stripping, although not in skin subjected to repeated sensitization with OVA. Allergic skin inflammation developed normally at sites of chronic epicutaneous sensitization with OVA in CRTH2(-/-) mice but was severely impaired in previously unsensitized skin challenged with OVA, as evidenced by significantly decreased skin infiltration with eosinophils and CD4(+) cells and impaired T(H)2 cytokine mRNA expression. Impaired skin inflammation at sites of acute OVA challenge in CRTH2(-/-) mice was not due to an impaired systemic response to epicutaneous sensitization because OVA-specific IgG1 and IgE antibody levels and OVA-driven splenocyte secretion of cytokines in these mice were comparable with those seen in wild-type control animals.
Conclusions: CRTH2 promotes allergic skin inflammation in response to cutaneous exposure to antigen in previously sensitized mice.
Copyright © 2010 American Academy of Allergy, Asthma & Immunology. Published by Mosby, Inc. All rights reserved.
Figures
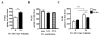

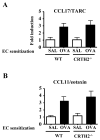
Similar articles
-
Antagonism of CRTH2 ameliorates chronic epicutaneous sensitization-induced inflammation by multiple mechanisms.Int Immunol. 2009 Jan;21(1):1-17. doi: 10.1093/intimm/dxn118. Epub 2008 Dec 9. Int Immunol. 2009. PMID: 19066315 Free PMC article.
-
IL-22 promotes allergic airway inflammation in epicutaneously sensitized mice.J Allergy Clin Immunol. 2019 Feb;143(2):619-630.e7. doi: 10.1016/j.jaci.2018.05.032. Epub 2018 Jun 18. J Allergy Clin Immunol. 2019. PMID: 29920352 Free PMC article.
-
IL-4 acts on skin-derived dendritic cells to promote the TH2 response to cutaneous sensitization and the development of allergic skin inflammation.J Allergy Clin Immunol. 2024 Dec;154(6):1462-1471.e3. doi: 10.1016/j.jaci.2024.06.021. Epub 2024 Jul 10. J Allergy Clin Immunol. 2024. PMID: 38996877
-
CRTH2 and D-type prostanoid receptor antagonists as novel therapeutic agents for inflammatory diseases.Pharmacology. 2010;85(6):372-82. doi: 10.1159/000313836. Epub 2010 Jun 16. Pharmacology. 2010. PMID: 20559016 Review.
-
Antagonists of the prostaglandin D2 receptor CRTH2.Drug News Perspect. 2008 Jul-Aug;21(6):317-22. doi: 10.1358/dnp.2008.21.6.1246831. Drug News Perspect. 2008. PMID: 18836589 Review.
Cited by
-
Mucosal immunology of tolerance and allergy in the gastrointestinal tract.Immunol Res. 2012 Dec;54(1-3):75-82. doi: 10.1007/s12026-012-8308-4. Immunol Res. 2012. PMID: 22447352 Free PMC article. Review.
-
The immunology of atopic dermatitis and its reversibility with broad-spectrum and targeted therapies.J Allergy Clin Immunol. 2017 Apr;139(4S):S65-S76. doi: 10.1016/j.jaci.2017.01.011. J Allergy Clin Immunol. 2017. PMID: 28390479 Free PMC article. Review.
-
Prostaglandin-cytokine crosstalk in chronic inflammation.Br J Pharmacol. 2019 Feb;176(3):337-354. doi: 10.1111/bph.14530. Epub 2018 Dec 18. Br J Pharmacol. 2019. PMID: 30381825 Free PMC article. Review.
-
New and Emerging Therapies for Pediatric Atopic Dermatitis.Paediatr Drugs. 2019 Aug;21(4):239-260. doi: 10.1007/s40272-019-00342-w. Paediatr Drugs. 2019. PMID: 31364023
-
Basophils are required for the induction of Th2 immunity to haptens and peptide antigens.Nat Commun. 2013;4:1739. doi: 10.1038/ncomms2740. Nat Commun. 2013. PMID: 23612279 Free PMC article.
References
-
- Hata AN, Breyer RM. Pharmacology and signaling of prostaglandin receptors: multiple roles in inflammation and immune modulation. Pharmacol Ther. 2004;103:147–66. - PubMed
-
- Roberts LJ, 2nd, Sweetman BJ, Lewis RA, Austen KF, Oates JA. Increased production of prostaglandin D2 in patients with systemic mastocytosis. N Engl J Med. 1980;303:1400–4. - PubMed
-
- Tanaka K, Hirai H, Takano S, Nakamura M, Nagata K. Effects of prostaglandin D2 on helper T cell functions. Biochem Biophys Res Commun. 2004;316:1009–14. - PubMed
-
- Rosenbach T, Czernielewski J, Hecker M, Czarnetzki B. Comparison of eicosanoid generation by highly purified human Langerhans cells and keratinocytes. J Invest Dermatol. 1990;95:104–7. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

